The effect of heat on skin permeability
- PMID: 18455889
- PMCID: PMC2464624
- DOI: 10.1016/j.ijpharm.2008.03.032
The effect of heat on skin permeability
Abstract
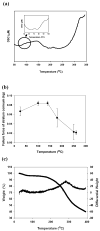
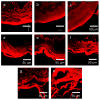
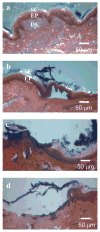
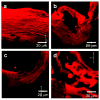
Although the effects of long exposure (>>1s) to moderate temperatures (< or =100 degrees C) have been well characterized, recent studies suggest that shorter exposure (<1s) to higher temperatures (>100 degrees C) can dramatically increase skin permeability. Previous studies suggest that by keeping exposures short, thermal damage can be localized to the stratum corneum without damaging deeper tissue. Initial clinical trials have progressed to Phase II (see http://clinicaltrials.gov), which indicates the procedure can be safe. Because the effect of heating under these conditions has received little systematic or mechanistic study, we heated full-thickness skin, epidermis and stratum corneum samples from human and porcine cadavers to temperatures ranging from 100 to 315 degrees C for times ranging from 100ms to 5s. Tissue samples were analyzed using skin permeability measurements, differential scanning calorimetry, thermomechanical analysis, thermal gravimetric analysis, brightfield and confocal microscopy, and histology. Skin permeability was shown to be a very strong function of temperature and a less strong function of the duration of heating. At optimal conditions used in this study, transdermal delivery of calcein was increased up to 760-fold by rapidly heating the skin at high temperature. More specifically, skin permeability was increased (I) by a few fold after heating to approximately 100-150 degrees C, (II) by one to two orders of magnitude after heating to approximately 150-250 degrees C and (III) by three orders of magnitude after heating above 300 degrees C. These permeability changes were attributed to (I) disordering of stratum corneum lipid structure, (II) disruption of stratum corneum keratin network structure and (III) decomposition and vaporization of keratin to create micron-scale holes in the stratum corneum, respectively. We conclude that heating the skin with short, high temperature pulses can increase skin permeability by orders of magnitude due to structural disruption and removal of stratum corneum.
Figures




References
-
- Badkar AV, Smith AM, Eppstein JA, Banga AK. Transdermal delivery of Interferon Alpha-2B using microporation and iontophoresis in hairless rats. Pharm Res. 2007;24:1389–1395. - PubMed
-
- Birchall J, Coulman S, Anstey A, Gateley C, Sweetland H, Gershonowitz A, Neville L, Levin G. Cutaneous gene expression of plasmid DNA in excised human skin following delivery via microchannels created by radio frequency ablation. Int J Pharm. 2006;312:15–23. - PubMed
-
- Bramson J, Dayball K, Evelegh C, Wan YH, Page D, Smith A. Enabling topical immunization via microporation: a novel method for pain-free and needle-free delivery of adenovirus-based vaccines. Gene Ther. 2003;10:251–260. - PubMed
-
- Cross SE, Roberts MS. Physical enhancement of transdermal drug application: Is delivery technology keeping up with phamaceutical development ? Curr Drug Delivery. 2004;1:81–92. - PubMed
-
- Davis SP, Landis BJ, Adams ZH, Allen MG, Prausnitz MR. Insertion of microneedles into skin: measurement and prediction of insertion force and needle fracture force. J Biomech. 2004;37:1155–1163. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources

