Antigen-induced immunomodulation in the pathogenesis of atherosclerosis
- PMID: 18551190
- PMCID: PMC2423423
- DOI: 10.1155/2008/723539
Antigen-induced immunomodulation in the pathogenesis of atherosclerosis
Abstract
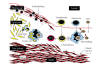
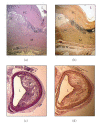
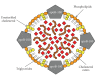
Atherosclerosis is a chronic inflammatory disorder characterised by the accumulation of monocytes/macrophages, smooth muscle cells, and lymphocytes within the arterial wall in response to the release of proinflammatory molecules. Such accumulation results in the formation of the atherosclerotic plaque, which would eventually evolve to complications such as total artery occlusion, rupture, calcification, or aneurysm. Although the molecular mechanism responsible for the development of atherosclerosis is not completely understood, it is clear that the immune system plays a key role in the development of the atherosclerotic plaque and in its complications. There are multiple antigenic stimuli that have been associated with the pathogenesis of atherosclerosis. Most of these stimuli come from modified self-molecules such as oxidised low-density lipoproteins (oxLDLs), beta2glycoprotein1 (beta2GP1), lipoprotein a (LP(a)), heat shock proteins (HSPs), and protein components of the extracellular matrix such as collagen and fibrinogen in the form of advanced glycation-end (AGE) products. In addition, several foreign antigens including bacteria such as Porphyromonas gingivalis and Chlamydia pneumoniae and viruses such as enterovirus and cytomegalovirus have been associated with atherosclerosis as potentially causative or bystander participants, adding another level of complexity to the analysis of the pathophysiology of atherosclerosis. The present review summarises the most important scientific findings published within the last two decades on the importance of antigens, antigen stimulation, and adaptive immune responses in the development of atherosclerotic plaques.
Figures
References
-
- Shashkin P, Dragulev B, Ley K. Macrophage differentiation to foam cells. Current Pharmaceutical Design. 2005;11(23):3061–3072. - PubMed
-
- Shi W, Wang X, Shih DM, Laubach VE, Navab M, Lusis AJ. Paradoxical reduction of fatty streak formation in mice lacking endothelial nitric oxide synthase. Circulation. 2002;105(17):2078–2082. - PubMed
-
- Pan JH, Sukhova GK, Yang JT, et al. Macrophage migration inhibitory factor deficiency impairs atherosclerosis in low-density lipoprotein receptor-deficient mice. Circulation. 2004;109(25):3149–3153. - PubMed
-
- Lucas AD, Greaves DR. Atherosclerosis: role of chemokines and macrophages. Expert Reviews in Molecular Medicine. 2001;3(25):1–18. - PubMed
-
- Fan J, Watanabe T. Inflammatory reactions in the pathogenesis of atherosclerosis. Journal of Atherosclerosis and Thrombosis. 2003;10(2):63–71. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

