Assessment of thyroid function: towards an integrated laboratory--clinical approach
- PMID: 18568049
- PMCID: PMC1853349
Assessment of thyroid function: towards an integrated laboratory--clinical approach
Abstract
Laboratory assessment of thyroid function is now often initiated with a low pre-test probability, by clinicians who may not have a detailed knowledge of current methodology or testing strategies. Skilled laboratory staff can significantly enhance the choice of appropriate tests and the accuracy of clinical response; such involvement requires both appropriate training and relevant information from the clinician. Measurement of the serum thyroid stimulating hormone (TSH) concentration with an assay of adequate sensitivity is now the cornerstone of thyroid function testing; for untreated populations at risk of primary thyroid dysfunction, a normal TSH concentration rules out an abnormality with a high degree of certainty. However, in several important situations, most notably pituitary abnormalities and early treatment of thyroid dysfunction, serum TSH can give a misleading indication of thyroid status. An abnormal TSH concentration alone is never an adequate basis for initiation of treatment, which should be based on the typical relationship between trophic and target gland hormones, based on serum TSH and an estimate of serum free thyroxine (T4). Six basic assumptions, some clinical, some laboratory-based, need to be considered, together with the relevant limiting conditions, for reliable use of this relationship. Current methods of free T4 estimation remain imperfect, especially during critical illness. Diagnostic approach differs significantly between initial diagnosis and follow-up of treated thyroid dysfunction. In some situations, serum triiodothyronine (T3) is also required, but serum T3 lacks sensitivity for diagnosis of hypothyroidism, and has poor specificity during non-thyroidal illness. Where assay results are anomalous, most atypical findings can be resolved by attention to the clinical context, without further investigation.
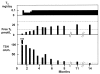
Figures

Similar articles
-
Measurement of serum total thyroxine, triiodothyronine, free thyroxine, and thyrotropin concentrations for diagnosis of hypothyroidism in dogs.J Am Vet Med Assoc. 1997 Dec 1;211(11):1396-402. J Am Vet Med Assoc. 1997. PMID: 9394888
-
Effects of propylthiouracil and bromocryptine on serum concentrations of thyrotrophin and thyroid hormones in normal female horses.Equine Vet J. 2003 May;35(3):296-301. doi: 10.2746/042516403776148309. Equine Vet J. 2003. PMID: 12755434
-
Are thyroid function tests too frequently and inappropriately requested?J Endocrinol Invest. 1999 Mar;22(3):184-90. doi: 10.1007/BF03343539. J Endocrinol Invest. 1999. PMID: 10219885
-
[Thyroxine (T4) and tri-iodothyronine (T3) determinations: techniques and value in the assessment of thyroid function].Ann Biol Clin (Paris). 2003 Jul-Aug;61(4):411-20. Ann Biol Clin (Paris). 2003. PMID: 12915350 Review. French.
-
Overt and subclinical hypothyroidism: who to treat and how.Drugs. 2012 Jan 1;72(1):17-33. doi: 10.2165/11598070-000000000-00000. Drugs. 2012. PMID: 22191793 Review.
Cited by
-
Diagnosis and treatment of hypothyroidism in old people : A new old challenge.Wien Klin Wochenschr. 2020 Mar;132(5-6):161-167. doi: 10.1007/s00508-019-01579-8. Epub 2019 Nov 26. Wien Klin Wochenschr. 2020. PMID: 31773270 Review.
-
The Diagnostic Yield of Thyroid Function Tests and their Cost-effectiveness in the Student Clinic at Sultan Qaboos University: Retrospective chart review.Sultan Qaboos Univ Med J. 2010 Aug;10(2):215-20. Epub 2010 Jul 19. Sultan Qaboos Univ Med J. 2010. PMID: 21509232 Free PMC article.
-
Subclinical hypothyroidism in children: updates for pediatricians.Ann Pediatr Endocrinol Metab. 2021 Jun;26(2):80-85. doi: 10.6065/apem.2040242.121. Epub 2021 Jun 30. Ann Pediatr Endocrinol Metab. 2021. PMID: 34218629 Free PMC article.
-
Reinterpreting patterns of variation in human thyroid function: An evolutionary ecology perspective.Evol Med Public Health. 2020 Nov 10;9(1):93-112. doi: 10.1093/emph/eoaa043. eCollection 2021. Evol Med Public Health. 2020. PMID: 34557302 Free PMC article. Review.
-
The influence of a biopsychosocial-based treatment approach to primary overt hypothyroidism: a protocol for a pilot study.Trials. 2010 Nov 15;11:106. doi: 10.1186/1745-6215-11-106. Trials. 2010. PMID: 21073760 Free PMC article. Clinical Trial.
References
-
- National Academy of Clinical Biochemistry. Laboratory Medicine Practice Guidelines. Laboratory Support for the Diagnosis of Thyroid Disease. Thyroid. 2003;13:1–126. and www.nacb.org/lmpg/thyroid_LMPG_word.stm. - PubMed
-
- For references to specific points in this text see: Thyroid Disease Manager Chapter 6b. Clinical Strategies for Thyroid Function Testing. www.thyroidmanager.org
-
- Haddow JE, Palomaki GE, Allan WC, et al. Maternal thyroid deficiency during pregnancy and subsequent neuropsychological development of the child. New Engl J Med. 1999;341:549–55. - PubMed
-
- Andersen S, Pedersen KM, Bruun NH, Laurberg P. Narrow individual variations in serum T4 and T3 in normal subjects: a clue to the understanding of subclinical thyroid disease. J Clin Endocrinol Metab. 2002;87:1068–72. - PubMed
-
- Vanderpump MPJ, Tunbridge WMG, French JM, et al. The incidence of thyroid disorders in the community: a twenty-year follow-up of the Whickham Survey. Clin Endocrinol. 1995;43:55–68. - PubMed
LinkOut - more resources
Full Text Sources
