Sources of U.S. physician income: the contribution of government payments to the specialist-generalist income gap
- PMID: 18592323
- PMCID: PMC2517994
- DOI: 10.1007/s11606-008-0660-7
Sources of U.S. physician income: the contribution of government payments to the specialist-generalist income gap
Abstract
Background: Physician income varies threefold among specialties. Lower incomes have produced shortages in primary care fields.
Objective: To investigate the impact of government policy on generating income differentials among specialties.
Design and participants: Cross-sectional analysis of the 2004 MEPS.
Measurements: For outpatient care, total payments made to 27 different types of specialists from five types of payers: Medicare, Medicaid, other government (the Veterans Administration and other state and local programs), private insurance, and out-of-pocket payments. For inpatient care, aggregate (i.e., all-specialty) inpatient physician reimbursement from the five payers.
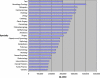
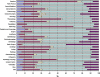
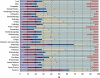
Results: In 2004, physicians derived 78.6% of their practice income ($149,684 million, 95% CI, $140,784 million-$158,584 million) from outpatient sources and 21.4% of their income ($40,782 million, 95% CI, $36,839 million-$44,724 million) from inpatient sources. Government payers accounted for 32.7% of total physician income. Four specialties derived > 50% of their outpatient income from public sources, including both the lowest and highest paid specialties (geriatrics and hematology/oncology, respectively).
Conclusions: Inter-specialty income differences result, in part, from government decisions.
Figures
Comment in
-
The specialist-generalist income gap: can we narrow it?J Gen Intern Med. 2008 Sep;23(9):1539-41. doi: 10.1007/s11606-008-0740-8. J Gen Intern Med. 2008. PMID: 18670827 Free PMC article. No abstract available.
References
-
- {'text': '', 'ref_index': 1, 'ids': [{'type': 'PubMed', 'value': '12564867', 'is_inner': True, 'url': 'https://pubmed.ncbi.nlm.nih.gov/12564867/'}]}
- Campbell RJ, Ramirez AM, Perez K, Roetzheim RG. Cervical cancer rates and the supply of primary care physicians in Florida. Fam Med. 2003;35(1):60–4. - PubMed
-
- {'text': '', 'ref_index': 1, 'ids': [{'type': 'PubMed', 'value': '9722797', 'is_inner': True, 'url': 'https://pubmed.ncbi.nlm.nih.gov/9722797/'}]}
- Franks P, Fiscella K. Primary care physicians and specialists as personal physicians. Health care expenditures and mortality experience. J Fam Pract. 1998;47(2):105–9. - PubMed
-
- {'text': '', 'ref_index': 1, 'ids': [{'type': 'DOI', 'value': '10.1093/pubmed/24.4.252', 'is_inner': False, 'url': 'https://doi.org/10.1093/pubmed/24.4.252'}, {'type': 'PubMed', 'value': '12546200', 'is_inner': True, 'url': 'https://pubmed.ncbi.nlm.nih.gov/12546200/'}]}
- Gulliford MC. Availability of primary care doctors and population health in England: is there an association? J Public Health Med. 2002;24(4):252–4. - PubMed
-
- {'text': '', 'ref_index': 1, 'ids': [{'type': 'PMC', 'value': 'PMC27892', 'is_inner': False, 'url': 'https://pmc.ncbi.nlm.nih.gov/articles/PMC27892/'}, {'type': 'PubMed', 'value': '10356004', 'is_inner': True, 'url': 'https://pubmed.ncbi.nlm.nih.gov/10356004/'}]}
- Jarman B, Gault S, Alves B, et al. Explaining differences in English hospital death rates using routinely collected data. Br Med J (Clinical Research Ed.). 1999;318(7197):1515–20. - PMC - PubMed
-
- {'text': '', 'ref_index': 1, 'ids': [{'type': 'DOI', 'value': '10.1377/hlthaff.24.2.465', 'is_inner': False, 'url': 'https://doi.org/10.1377/hlthaff.24.2.465'}, {'type': 'PubMed', 'value': '15757932', 'is_inner': True, 'url': 'https://pubmed.ncbi.nlm.nih.gov/15757932/'}]}
- O’Malley AS, Forrest CB, Politzer RM, Wulu JT, Shi L. Health center trends, 1994–2001: what do they portend for the federal growth initiative? Health Aff (Millwood). 2005;24(2):465–72. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Miscellaneous

