Atorvastatin increases myocardial indices of oxidative stress in a porcine model of hypercholesterolemia and chronic ischemia
- PMID: 18598320
- PMCID: PMC2629376
- DOI: 10.1111/j.1540-8191.2008.00600.x
Atorvastatin increases myocardial indices of oxidative stress in a porcine model of hypercholesterolemia and chronic ischemia
Abstract
Background/aim: Atorvastatin has previously been shown to reduce the endogenous angiogenic response to chronic ischemia in a porcine model. One possible mechanism for this effect is reduced bioavailability of nitric oxide, a key mediator of angiogenesis, secondary to increased oxygen free radicals. We sought to determine if atorvastatin modulates oxidative stress in myocardial tissue.
Methods: Dietary induction of hypercholesterolemia was performed over 20 weeks in Yucatan swine with treated animals receiving atorvastatin 3 mg/kg/day. Chronic myocardial ischemia was induced via surgical placement of an ameroid constrictor ring around the proximal circumflex artery at age 20 weeks, followed by tissue harvest at age 27 weeks. Myocardial levels of protein, lipid, and DNA biomarkers of oxidative stress, serum levels of 8-isoprostane, nitric oxide (NO) dependent, and independent coronary microvascular reactivity, as well as isotope-labeled microsphere myocardial perfusion analysis and histologic analysis for endothelial cell density was performed.
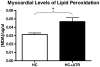
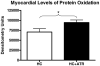
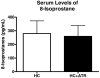
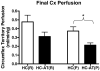
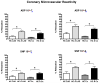
Results: Atorvastatin treatment was associated with elevated levels of myocardial protein oxidation and lipid peroxidation. Conversely, serum oxidant stress biomarkers were not elevated. Atorvastatin treatment improved nitric oxide dependent and independent microvascular reactivity, and was associated with decreased perfusion in the ischemic myocardial territory.
Conclusion: Treatment with atorvastatin was associated with increased levels of myocardial tissue protein and lipid oxidative stress biomarkers and a reduced functional endogenous angiogenic response, but improved coronary microvascular reactivity. Increased oxidative stress in tissues may play a role in the reduced angiogenic response seen with atorvastatin treatment in other studies.
Figures


Similar articles
-
High-dose atorvastatin improves hypercholesterolemic coronary endothelial dysfunction without improving the angiogenic response.Circulation. 2006 Jul 4;114(1 Suppl):I402-8. doi: 10.1161/CIRCULATIONAHA.105.000356. Circulation. 2006. PMID: 16820608
-
Atorvastatin increases oxidative stress and modulates angiogenesis in Ossabaw swine with the metabolic syndrome.J Thorac Cardiovasc Surg. 2012 Dec;144(6):1486-93. doi: 10.1016/j.jtcvs.2012.08.065. Epub 2012 Sep 17. J Thorac Cardiovasc Surg. 2012. PMID: 22995723 Free PMC article.
-
Atorvastatin impairs the myocardial angiogenic response to chronic ischemia in normocholesterolemic swine.J Thorac Cardiovasc Surg. 2008 Jan;135(1):117-22. doi: 10.1016/j.jtcvs.2007.04.021. J Thorac Cardiovasc Surg. 2008. PMID: 18179927
-
Atorvastatin: an updated review of its pharmacological properties and use in dyslipidaemia.Drugs. 2001;61(12):1835-81. doi: 10.2165/00003495-200161120-00012. Drugs. 2001. PMID: 11693468 Review.
-
Atorvastatin.Expert Opin Pharmacother. 2001 May;2(5):819-30. doi: 10.1517/14656566.2.5.819. Expert Opin Pharmacother. 2001. PMID: 11336625 Review.
Cited by
-
Quantitative evaluation of contrast-enhanced ultrasonography in the diagnosis of chronic ischemic renal disease in a dog model.PLoS One. 2013 Aug 1;8(8):e70337. doi: 10.1371/journal.pone.0070337. Print 2013. PLoS One. 2013. PMID: 23936410 Free PMC article.
-
Modulation of Hypercholesterolemia-Induced Oxidative/Nitrative Stress in the Heart.Oxid Med Cell Longev. 2016;2016:3863726. doi: 10.1155/2016/3863726. Epub 2015 Dec 14. Oxid Med Cell Longev. 2016. PMID: 26788247 Free PMC article. Review.
-
Pharmacotherapy for end-stage coronary artery disease.Expert Opin Pharmacother. 2010 Feb;11(2):207-13. doi: 10.1517/14656560903439737. Expert Opin Pharmacother. 2010. PMID: 20088742 Free PMC article. Review.
-
HMG-CoA reductase inhibitors induce apoptosis of lymphoma cells by promoting ROS generation and regulating Akt, Erk and p38 signals via suppression of mevalonate pathway.Cell Death Dis. 2013 Feb 28;4(2):e518. doi: 10.1038/cddis.2013.44. Cell Death Dis. 2013. PMID: 23449454 Free PMC article.
-
Ascorbic acid mitigates the myocardial injury after cardiac arrest and electrical shock.Intensive Care Med. 2011 Dec;37(12):2033-40. doi: 10.1007/s00134-011-2362-6. Epub 2011 Sep 28. Intensive Care Med. 2011. PMID: 21953354
References
-
- Sato K, Wu T, Laham RJ, et al. Efficacy of intracoronary or intravenous VEGF165 in a pig model of chronic myocardial ischemia. J Am Coll Cardiol. 2001;37(2):616–623. - PubMed
-
- Sato K, Laham RJ, Pearlman JD, et al. Efficacy of intracoronary versus intravenous FGF-2 in a pig model of chronic myocardial ischemia. Ann Thorac Surg. 2000;70(6):2113–2118. - PubMed
-
- Laham RJ, Rezaee M, Post M, et al. Intrapericardial delivery of fibroblast growth factor-2 induces neovascularization in a porcine model of chronic myocardial ischemia. J Pharmacol Exp Ther. 2000;292(2):795–802. - PubMed
-
- Lopez JJ, Laham RJ, Stamler A, et al. VEGF administration in chronic myocardial ischemia in pigs. Cardiovasc Res. 1998;40(2):272–281. - PubMed
-
- Simons M, Annex BH, Laham RJ, et al. Pharmacological treatment of coronary artery disease with recombinant fibroblast growth factor-2: Double-blind, randomized, controlled clinical trial. Circulation. 2002;105(7):788–793. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

