Urinary cystatin C as an early biomarker of acute kidney injury following adult cardiothoracic surgery
- PMID: 18650797
- PMCID: PMC2745082
- DOI: 10.1038/ki.2008.341
Urinary cystatin C as an early biomarker of acute kidney injury following adult cardiothoracic surgery
Abstract
There is a need to develop early biomarkers of acute kidney injury following cardiac surgery, where morbidity and mortality are increased by its presence. Plasma cystatin C (CyC) and plasma and urine Neutrophil Gelatinase Associated Lipocalin (NGAL) have been shown to detect kidney injury earlier than changes in plasma creatinine in critically ill patients. In order to determine the utility of urinary CyC levels as a measure of kidney injury, we prospectively collected plasma and urine from 72 adults undergoing elective cardiac surgery for analysis. Acute kidney injury was defined as a 25% or greater increase in plasma creatinine or renal replacement therapy within the first 72 hours following surgery. Plasma CyC and NGAL were not useful predictors of acute kidney injury within the first 6 hours following surgery. In contrast, both urinary CyC and NGAL were elevated in the 34 patients who later developed acute kidney injury, compared to those with no injury. The urinary NGAL at the time of ICU arrival and the urinary CyC level 6 hours after ICU admission were most useful for predicting acute kidney injury. A composite time point consisting of the maximum urinary CyC achieved in the first 6 hours following surgery outperformed all individual time points. Our study suggests that urinary CyC and NGAL are superior to conventional and novel plasma markers in the early diagnosis of acute kidney injury following adult cardiac surgery.
Conflict of interest statement
Figures
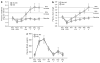


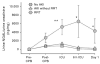
Comment in
-
The hunt for the perfect biomarker for acute kidney injury: back to gamma-trace?Kidney Int. 2008 Oct;74(8):987-9. doi: 10.1038/ki.2008.426. Kidney Int. 2008. PMID: 18827797 Review.
Similar articles
-
Urinary biomarkers and renal near-infrared spectroscopy predict intensive care unit outcomes after cardiac surgery in infants younger than 6 months of age.J Thorac Cardiovasc Surg. 2013 Oct;146(4):861-867.e1. doi: 10.1016/j.jtcvs.2012.12.012. Epub 2013 Jan 12. J Thorac Cardiovasc Surg. 2013. PMID: 23317940 Free PMC article.
-
The clinical utility window for acute kidney injury biomarkers in the critically ill.Crit Care. 2014 Nov 4;18(6):601. doi: 10.1186/s13054-014-0601-2. Crit Care. 2014. PMID: 25366893 Free PMC article. Clinical Trial.
-
Assessment of biochemical markers in the early post-burn period for predicting acute kidney injury and mortality in patients with major burn injury: comparison of serum creatinine, serum cystatin-C, plasma and urine neutrophil gelatinase-associated lipocalin.Crit Care. 2014 Jul 14;18(4):R151. doi: 10.1186/cc13989. Crit Care. 2014. PMID: 25023056 Free PMC article.
-
High-dose fenoldopam reduces postoperative neutrophil gelatinase-associated lipocaline and cystatin C levels in pediatric cardiac surgery.Crit Care. 2011 Jun 29;15(3):R160. doi: 10.1186/cc10295. Crit Care. 2011. PMID: 21714857 Free PMC article. Clinical Trial.
-
Neutrophil gelatinase-associated lipocalin: a promising biomarker for detecting cardiac surgery-associated acute kidney injury.J Thorac Cardiovasc Surg. 2010 May;139(5):1101-6. doi: 10.1016/j.jtcvs.2009.11.007. J Thorac Cardiovasc Surg. 2010. PMID: 20412947 Review.
Cited by
-
Urine interleukin-18 and cystatin-C as biomarkers of acute kidney injury in critically ill neonates.Pediatr Nephrol. 2012 May;27(5):851-60. doi: 10.1007/s00467-011-2072-x. Epub 2012 Jan 8. Pediatr Nephrol. 2012. PMID: 22228436 Free PMC article.
-
Role of new biomarkers: functional and structural damage.Crit Care Res Pract. 2013;2013:361078. doi: 10.1155/2013/361078. Epub 2013 Feb 5. Crit Care Res Pract. 2013. PMID: 23476755 Free PMC article.
-
Serum cystatin C- versus creatinine-based definitions of acute kidney injury following cardiac surgery: a prospective cohort study.Am J Kidney Dis. 2012 Dec;60(6):922-9. doi: 10.1053/j.ajkd.2012.06.002. Epub 2012 Jul 17. Am J Kidney Dis. 2012. PMID: 22809763 Free PMC article.
-
Imperfect gold standards for kidney injury biomarker evaluation.J Am Soc Nephrol. 2012 Jan;23(1):13-21. doi: 10.1681/ASN.2010111124. Epub 2011 Oct 21. J Am Soc Nephrol. 2012. PMID: 22021710 Free PMC article.
-
Neutrophil gelatinase-associated lipocalin--an emerging troponin for kidney injury.Nephrol Dial Transplant. 2008 Dec;23(12):3737-43. doi: 10.1093/ndt/gfn531. Epub 2008 Sep 22. Nephrol Dial Transplant. 2008. PMID: 18809975 Free PMC article. Review. No abstract available.
References
-
- Wijeysundera DN, Karkouti K, Dupuis JY, et al. Derivation and validation of a simplified predictive index for renal replacement therapy after cardiac surgery. JAMA. 2007;297:1801–1809. - PubMed
-
- Abel R, Buckley M, Austen W, et al. Etiology, incidence and prognosis of renal failure following cardiac operations. Results of a prospective analysis of 500 consecutive patients. J Thorac Cardiovasc Surg. 1976;71:323–333. - PubMed
-
- Andersson L, Ekroth R, Bratteby L, et al. Acute renal failure after coronary surgery: a study of incidence and risk factors in 2009 consecutive patients. Thorac Cardiovasc Surg. 1993;41:237–241. - PubMed
-
- Chertow G, Levy E, Hammermeister K, et al. Independent association between acute renal failure and mortality following cardiac surgery. Am J Med. 1998;104:343–348. - PubMed
-
- Conlon P, Strafford-Smith M, WD W, et al. Acute renal failure following cardiac surgery. Nephrol Dial Transplant. 1999;14:1158–1162. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

