MRI evaluation of isolated arthroscopic partial meniscectomy patients at a minimum five-year follow-up
- PMID: 18751768
- PMCID: PMC2504089
- DOI: 10.1007/s11420-006-9031-2
MRI evaluation of isolated arthroscopic partial meniscectomy patients at a minimum five-year follow-up
Abstract
Background: The risk of radiographic knee degeneration after partial or total meniscectomy is well documented, but no prior study has employed cartilage-sensitive MRI technology to assess degenerative changes after meniscectomy.
Hypothesis: Arthroscopic partial meniscectomy results in early articular cartilage wear and subchondral bony degeneration, even in the absence of clinical symptoms, and these findings can be evaluated with cartilage-sensitive MRI.
Study design: Retrospective cohort.
Methods: Twenty-nine patients (ages: 15-40) who had undergone isolated arthroscopic partial medial or lateral meniscectomy with at least 5-year follow-up were evaluated. All patients had arthroscopically normal articular cartilage at the time of initial meniscectomy. Seventeen patients (18 knees) underwent partial medial meniscectomy (MM) and 12 patients underwent partial lateral meniscectomy (LM) with mean follow-up of 8.4 and 7.1 years, respectively. Follow-up evaluation included physical examination, outcome questionnaires, and cartilage-sensitive MRI examination with modified Outerbridge grading of articular surfaces.
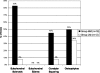
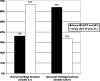
Results: Outerbridge grades II-IV were noted in 64% of medial compartment joint surfaces in group MM knees versus 33% of lateral compartment joint surfaces in group LM knees. Abnormal cartilage surfaces (grades II-IV), subchondral sclerosis, and condylar squaring were all significantly more frequent after medial meniscectomy (p < 0.05). Groups MM and LM had no significant differences among outcome scores, which remained excellent in both groups. A significant negative correlation was found between the severity of cartilage wear and functional scoring in the MM group, suggesting that functional disability lags behind early MRI evidence of degeneration.
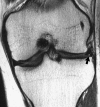
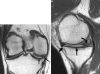
Conclusions: Despite optimal preoperative prognostic factors and excellent functional outcomes, MRI evidence of early articular cartilage degeneration was present in both partial medial and lateral meniscectomy patients at a minimum 5-year follow-up. Results support the use of cartilage-sensitive MRI as a noninvasive screening technique to evaluate cartilage changes after arthroscopic partial meniscectomy and may help to counsel the high-risk patient in regard to postoperative activity.
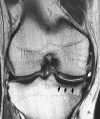
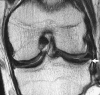
Figures

Similar articles
-
Changes in articular cartilage following arthroscopic partial medial meniscectomy.Knee Surg Sports Traumatol Arthrosc. 2016 May;24(5):1440-7. doi: 10.1007/s00167-015-3542-7. Epub 2015 Feb 20. Knee Surg Sports Traumatol Arthrosc. 2016. PMID: 25697283
-
Arthroscopic partial meniscectomy in young patients with symptomatic discoid lateral meniscus: an average 10-year follow-up study.Arch Orthop Trauma Surg. 2018 Mar;138(3):369-376. doi: 10.1007/s00402-017-2853-1. Epub 2017 Nov 29. Arch Orthop Trauma Surg. 2018. PMID: 29188421
-
Chondral lesions at the medial femoral condyle, meniscal degeneration, anterior cruciate ligament insufficiency, and lateral meniscal tears impair the middle-term results after arthroscopic partial meniscectomy.Knee Surg Sports Traumatol Arthrosc. 2020 Nov;28(11):3488-3496. doi: 10.1007/s00167-020-05883-z. Epub 2020 Feb 8. Knee Surg Sports Traumatol Arthrosc. 2020. PMID: 32036398
-
A comparative study of medial versus lateral arthroscopic partial meniscectomy on stable knees: 10-year minimum follow-up.Arthroscopy. 2003 Oct;19(8):842-9. doi: 10.1016/s0749-8063(03)00735-7. Arthroscopy. 2003. PMID: 14551546 Review.
-
Clinical and radiographic results of partial versus total meniscectomy in patients with symptomatic discoid lateral meniscus: A systematic review and meta-analysis.Orthop Traumatol Surg Res. 2019 Jun;105(4):669-675. doi: 10.1016/j.otsr.2019.02.023. Epub 2019 Apr 23. Orthop Traumatol Surg Res. 2019. PMID: 31027980
Cited by
-
Meniscectomy.Knee Surg Relat Res. 2012 Sep;24(3):129-36. doi: 10.5792/ksrr.2012.24.3.129. Epub 2012 Sep 3. Knee Surg Relat Res. 2012. PMID: 22977789 Free PMC article.
-
Treatment options for the symptomatic post-meniscectomy knee.Knee Surg Sports Traumatol Arthrosc. 2019 Jun;27(6):1817-1824. doi: 10.1007/s00167-019-05424-3. Epub 2019 Mar 11. Knee Surg Sports Traumatol Arthrosc. 2019. PMID: 30859265 Review.
-
Meniscal Allograft Transplantation Concomitant With Cartilage Repair for Symptomatic Lateral Meniscus-Deficient Knees With Over Two Years of Follow-up.Cureus. 2023 Nov 14;15(11):e48774. doi: 10.7759/cureus.48774. eCollection 2023 Nov. Cureus. 2023. PMID: 38024091 Free PMC article.
-
The Interplay of Biomechanical and Biological Changes Following Meniscus Injury.Curr Rheumatol Rep. 2023 Feb;25(2):35-46. doi: 10.1007/s11926-022-01093-3. Epub 2022 Dec 7. Curr Rheumatol Rep. 2023. PMID: 36479669 Free PMC article. Review.
-
Cartilage MRI relaxation times after arthroscopic partial medial meniscectomy reveal localized degeneration.Knee Surg Sports Traumatol Arthrosc. 2015 Jan;23(1):188-97. doi: 10.1007/s00167-014-2997-2. Epub 2014 May 4. Knee Surg Sports Traumatol Arthrosc. 2015. PMID: 24792070
References
-
- {'text': '', 'ref_index': 1, 'ids': [{'type': 'PubMed', 'value': '10380269', 'is_inner': True, 'url': 'https://pubmed.ncbi.nlm.nih.gov/10380269/'}]}
- Aagaard H, Verdonk R (1999) Function of the normal meniscus and consequences of meniscal resection. Scand J Med Sci Sports 9:134–140 - PubMed
-
- {'text': '', 'ref_index': 1, 'ids': [{'type': 'PubMed', 'value': '2379357', 'is_inner': True, 'url': 'https://pubmed.ncbi.nlm.nih.gov/2379357/'}]}
- Abdon P, Turner MS, Pettersson H, Lindstrand A, Stenstrom A, Swanson AJ (1990) A long-term follow-up study of total meniscectomy in children. Clin Orthop 257:166–170 - PubMed
-
- {'text': '', 'ref_index': 1, 'ids': [{'type': 'PubMed', 'value': '3570751', 'is_inner': True, 'url': 'https://pubmed.ncbi.nlm.nih.gov/3570751/'}]}
- Aglietti P, Buzzi R, Bassi PB, Pisaneschi A (1986) Results of arthroscopic meniscectomy. Ital J Orthop Traumatol 12:315–325 - PubMed
-
- {'text': '', 'ref_index': 1, 'ids': [{'type': 'DOI', 'value': '10.1177/036354658601400405', 'is_inner': False, 'url': 'https://doi.org/10.1177/036354658601400405'}, {'type': 'PubMed', 'value': '3755296', 'is_inner': True, 'url': 'https://pubmed.ncbi.nlm.nih.gov/3755296/'}]}
- Baratz ME, Fu FH, Mengato R (1986) Meniscal tears: the effect of meniscectomy and of repair on intraarticular contact areas and stress in the human knee. A preliminary report. Am J Sports Med 14:270–275 - PubMed
-
- {'text': '', 'ref_index': 1, 'ids': [{'type': 'DOI', 'value': '10.1007/BF01560216', 'is_inner': False, 'url': 'https://doi.org/10.1007/bf01560216'}, {'type': 'PubMed', 'value': '8536038', 'is_inner': True, 'url': 'https://pubmed.ncbi.nlm.nih.gov/8536038/'}]}
- Benedetto KP, Rangger C (1993) Arthroscopic partial meniscectomy: 5-year follow-up. Knee Surg Sports Traumatol Arthrosc 1:235–238 - PubMed
LinkOut - more resources
Full Text Sources
Medical

