Effects of inhaled iloprost on right ventricular contractility, right ventriculo-vascular coupling and ventricular interdependence: a randomized placebo-controlled trial in an experimental model of acute pulmonary hypertension
- PMID: 18783596
- PMCID: PMC2592739
- DOI: 10.1186/cc7005
Effects of inhaled iloprost on right ventricular contractility, right ventriculo-vascular coupling and ventricular interdependence: a randomized placebo-controlled trial in an experimental model of acute pulmonary hypertension
Abstract
Introduction: Prostacyclin inhalation is increasingly used to treat acute pulmonary hypertension and right ventricular failure, although its pharmacodynamic properties remain controversial. Prostacyclins not only affect vasomotor tone but may also have cAMP-mediated positive inotropic effects and modulate autonomic nervous system tone. We studied the role of these different mechanisms in the overall haemodynamic effects produced by iloprost inhalation in an experimental model of acute pulmonary hypertension.
Methods: In this prospective, randomized, placebo-controlled animal study, twenty-six pigs (mean weight 35 +/- 2 kg) were instrumented with biventricular conductance catheters, a pulmonary artery flow probe and a high-fidelity pulmonary artery pressure catheter. The effects of inhaled iloprost (50 microg) were studied in the following groups: animals with acute hypoxia-induced pulmonary hypertension, and healthy animals with and without blockade of the autonomic nervous system.
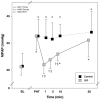
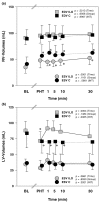
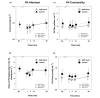
Results: During pulmonary hypertension, inhalation of iloprost resulted in a 51% increase in cardiac output compared with placebo (5.6 +/- 0.7 versus 3.7 +/- 0.8 l/minute; P = 0.0013), a selective reduction in right ventricular afterload (effective pulmonary arterial elastance: 0.6 +/- 0.3 versus 1.2 +/- 0.5 mmHg/ml; P = 0.0005) and a significant increase in left ventricular end-diastolic volume (91 +/- 12 versus 70 +/- 20 ml; P = 0.006). Interestingly, right ventricular contractility was reduced after iloprost-treatment (slope of preload recruitable stroke work: 2.2 +/- 0.5 versus 3.4 +/- 0.8 mWatt.s/ml; P = 0.0002), whereas ventriculo-vascular coupling remained essentially preserved (ratio of right ventricular end-systolic elastance to effective pulmonary arterial elastance: 0.97 +/- 0.33 versus 1.03 +/- 0.15). In healthy animals, inhaled iloprost had only minimal haemodynamic effects and produced no direct effects on myocardial contractility, even after pharmacological blockade of the autonomic nervous system.
Conclusions: In animals with acute pulmonary hypertension, inhaled iloprost improved global haemodynamics primarily via selective pulmonary vasodilatation and restoration of left ventricular preload. The reduction in right ventricular afterload is associated with a paradoxical decrease in right ventricular contractility. Our data suggest that this reflects an indirect mechanism by which ventriculo-vascular coupling is maintained at the lowest possible energetic cost. We found no evidence for a direct negative inotropic effect of iloprost.
Figures


Similar articles
-
Levosimendan improves right ventriculovascular coupling in a porcine model of right ventricular dysfunction.Crit Care Med. 2007 Mar;35(3):707-15. doi: 10.1097/01.CCM.0000257326.96342.57. Crit Care Med. 2007. PMID: 17255859
-
Epoprostenol treatment of acute pulmonary hypertension is associated with a paradoxical decrease in right ventricular contractility.Intensive Care Med. 2008 Jan;34(1):179-89. doi: 10.1007/s00134-007-0831-8. Epub 2007 Aug 21. Intensive Care Med. 2008. PMID: 17710383
-
Thoracic epidural anesthesia impairs the hemodynamic response to acute pulmonary hypertension by deteriorating right ventricular-pulmonary arterial coupling.Crit Care Med. 2007 Jan;35(1):222-9. doi: 10.1097/01.CCM.0000250357.35250.A2. Crit Care Med. 2007. PMID: 17095942
-
Management of adult patients with perioperative pulmonary hypertension: technical aspects and therapeutic options.Cardiology. 2010;116(1):3-9. doi: 10.1159/000313863. Epub 2010 Apr 24. Cardiology. 2010. PMID: 20424446
-
Management of pulmonary hypertension: physiological and pharmacological considerations for anesthesiologists.Anesth Analg. 2003 Jun;96(6):1603-1616. doi: 10.1213/01.ANE.0000062523.67426.0B. Anesth Analg. 2003. PMID: 12760982 Review. No abstract available.
Cited by
-
Effects of acute intravenous iloprost on right ventricular hemodynamics in rats with chronic pulmonary hypertension.Pulm Circ. 2014 Dec;4(4):612-8. doi: 10.1086/677358. Pulm Circ. 2014. PMID: 25610597 Free PMC article.
-
Methods for measuring right ventricular function and hemodynamic coupling with the pulmonary vasculature.Ann Biomed Eng. 2013 Jul;41(7):1384-98. doi: 10.1007/s10439-013-0752-3. Epub 2013 Feb 20. Ann Biomed Eng. 2013. PMID: 23423705 Free PMC article. Review.
-
[Is less always more?: modalities of extended haemodynamic monitoring for single-lung ventilation].Anaesthesist. 2009 Nov;58(11):1081-2. doi: 10.1007/s00101-009-1634-9. Anaesthesist. 2009. PMID: 19885648 German. No abstract available.
-
Reversal of Right Ventricular Hypertrophy and Dysfunction by Prostacyclin in a Rat Model of Severe Pulmonary Arterial Hypertension.Int J Mol Sci. 2022 May 12;23(10):5426. doi: 10.3390/ijms23105426. Int J Mol Sci. 2022. PMID: 35628236 Free PMC article.
-
Right ventricular function in pulmonary (arterial) hypertension.Herz. 2019 Sep;44(6):509-516. doi: 10.1007/s00059-019-4815-6. Herz. 2019. PMID: 31101945 Review. English.
References
-
- Olschewski H, Simonneau G, Galie N, Higenbottam T, Naeije R, Rubin LJ, Nikkho S, Speich R, Hoeper MM, Behr J, Winkler J, Sitbon O, Popov W, Ghofrani HA, Manes A, Kiely DG, Ewert R, Meyer A, Corris PA, Delcroix M, Gomez-Sanchez M, Siedentop H, Seeger W. Inhaled iloprost for severe pulmonary hypertension. N Engl J Med. 2002;347:322–329. doi: 10.1056/NEJMoa020204. - DOI - PubMed
-
- Rex S, Schaelte G, Metzelder S, Flier S, de Waal EE, Autschbach R, Rossaint R, Buhre W. Inhaled iloprost to control pulmonary artery hypertension in patients undergoing mitral valve surgery: a prospective, randomized-controlled trial. Acta Anaesthesiol Scand. 2008;52:65–72. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

