Eye syndromes and the neuro-ophthalmology of stroke
- PMID: 18804670
- PMCID: PMC2997492
- DOI: 10.1016/S0072-9752(08)93029-3
Eye syndromes and the neuro-ophthalmology of stroke
Figures
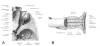
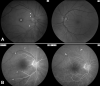
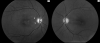


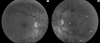
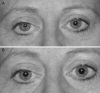
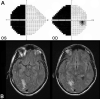
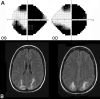
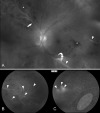
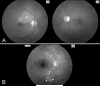
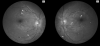
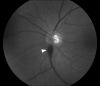
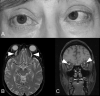
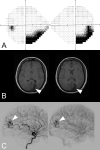
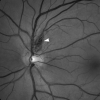

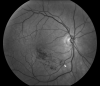

Similar articles
-
Reactions of the elements of retina and optic nerve in common morbid entities of the human eye.Am J Ophthalmol. 1956 Oct;42(4 Part 2):10-27. doi: 10.1016/0002-9394(56)90352-x. Am J Ophthalmol. 1956. PMID: 13372650 No abstract available.
-
Krabbe's disease. Histopathology and ultrastructure of the eye.Am J Ophthalmol. 1972 Sep;74(3):400-6. Am J Ophthalmol. 1972. PMID: 4115450 No abstract available.
-
Intraocular Taenia crassiceps (Cestoda).Trans Am Acad Ophthalmol Otolaryngol. 1973 Nov-Dec;77(6):OP778-83. Trans Am Acad Ophthalmol Otolaryngol. 1973. PMID: 4772538 No abstract available.
-
Neuro-ophthalmology.Arch Ophthalmol. 1971 Jan;85(1):111-26. doi: 10.1001/archopht.1971.00990050113018. Arch Ophthalmol. 1971. PMID: 4321751 Review. No abstract available.
-
NEURO-OPHTHALMOLOGY.Arch Ophthalmol. 1964 Nov;72:679-719. doi: 10.1001/archopht.1964.00970020679019. Arch Ophthalmol. 1964. PMID: 14198895 Review. No abstract available.
Cited by
-
Ocular Circulation and Chronic Ocular Ischemic Syndrome before and after Carotid Artery Revascularization Surgery.J Ophthalmol. 2012;2012:350475. doi: 10.1155/2012/350475. Epub 2012 Dec 20. J Ophthalmol. 2012. PMID: 23316337 Free PMC article.
-
The Role of Ophthalmology in Tele-Stroke Consults for Triaging Acute Vision Loss.Open Access Emerg Med. 2024 Feb 5;16:45-56. doi: 10.2147/OAEM.S395588. eCollection 2024. Open Access Emerg Med. 2024. PMID: 38343729 Free PMC article.
-
Associations among Stroke, Myocardial Infarction, and Amaurosis Fugax in a Tertiary Referral Hospital in Taiwan.J Clin Med. 2022 Aug 30;11(17):5088. doi: 10.3390/jcm11175088. J Clin Med. 2022. PMID: 36079019 Free PMC article.
-
Ocular ischemic syndrome due to severe internal carotid artery stenosis improved by intracranial stent placement: A case report.Surg Neurol Int. 2021 Jun 21;12:294. doi: 10.25259/SNI_361_2021. eCollection 2021. Surg Neurol Int. 2021. PMID: 34221625 Free PMC article.
-
Eyes and stroke: the visual aspects of cerebrovascular disease.Stroke Vasc Neurol. 2017 Jul 6;2(4):210-220. doi: 10.1136/svn-2017-000079. eCollection 2017 Dec. Stroke Vasc Neurol. 2017. PMID: 29507782 Free PMC article. Review.
References
-
- Fisher CM. ‘Transient monocular blindness’ versus ‘amaurosis fugax’. Neurology. 1989;39(12):1622–4. - PubMed
-
- Biousse V, Trobe JD. Transient monocular visual loss. Am J Ophthalmol. 2005;140(4):717–21. - PubMed
-
- Biousse V. Cerebrovascular diseases. In: Miller N, Newman N, Biousse B, Kerrison J, editors. Walsh & Hoyt’s Clinical Neuro-Ophthalmology. 6th edition Williams & Wilkins; Philadelphia: 2005. pp. 1967–2168.
-
- Luneau K, Newman NJ, Biousse V. Ischemic optic neuropathies. Neurologist. 2008;14(6):341–54. - PubMed
-
- Hayreh SS, Zimmerman MB. Fundus changes in central retinal artery occlusion. Retina. 2007;27(3):276–89. - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

