Incidence of hepatocellular carcinoma and associated risk factors in hepatitis C-related advanced liver disease
- PMID: 18848939
- PMCID: PMC3749922
- DOI: 10.1053/j.gastro.2008.09.014
Incidence of hepatocellular carcinoma and associated risk factors in hepatitis C-related advanced liver disease
Abstract
Background & aims: Although the incidence of hepatocellular carcinoma (HCC) is increasing in the United States, data from large prospective studies are limited. We evaluated the Hepatitis C Antiviral Long-Term Treatment Against Cirrhosis (HALT-C) cohort for the incidence of HCC and associated risk factors.
Methods: Hepatitis C virus-positive patients with bridging fibrosis or cirrhosis who did not respond to peginterferon and ribavirin were randomized to groups that were given maintenance peginterferon for 3.5 years or no treatment. HCC incidence was determined by Kaplan-Meier analysis, and baseline factors associated with HCC were analyzed by Cox regression.
Results: 1,005 patients (mean age, 50.2 years; 71% male; 72% white race) were studied; 59% had bridging fibrosis, and 41% had cirrhosis. During a median follow-up of 4.6 years (maximum, 6.7 years), HCC developed in 48 patients (4.8%). The cumulative 5-year HCC incidence was similar for peginterferon-treated patients and controls, 5.4% vs 5.0%, respectively (P= .78), and was higher among patients with cirrhosis than those with bridging fibrosis, 7.0% vs 4.1%, respectively (P= .08). HCC developed in 8 (17%) patients whose serial biopsy specimens showed only fibrosis. A multivariate analysis model comprising older age, black race, lower platelet count, higher alkaline phosphatase, esophageal varices, and smoking was developed to predict the risk of HCC.
Conclusions: We found that maintenance peginterferon did not reduce the incidence of HCC in the HALT-C cohort. Baseline clinical and laboratory features predicted risk for HCC. Additional studies are required to confirm our finding of HCC in patients with chronic hepatitis C and bridging fibrosis.
Trial registration: ClinicalTrials.gov NCT00006164.
Conflict of interest statement
Potential investigator conflict of interest had been disclosed to study participants
Figures


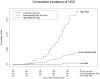


Comment in
-
Hepatitis C and hepatocellular carcinoma: grist for the mill.Gastroenterology. 2009 Jan;136(1):39-42. doi: 10.1053/j.gastro.2008.11.023. Epub 2008 Nov 28. Gastroenterology. 2009. PMID: 19041651 No abstract available.
References
-
- Thomas DL, Seeff LB. Natural history of hepatitis C. Clin Liver Dis. 2005;9(3):383–98. vi. - PubMed
-
- Fattovich G, Giustina G, Degos F, et al. Morbidity and mortality in compensated cirrhosis type C: a retrospective follow-up study of 384 patients. Gastroenterology. 1997;112(2):463–72. - PubMed
-
- Simonetti RG, Camma C, Fiorello F, et al. Hepatitis C virus infection as a risk factor for hepatocellular carcinoma in patients with cirrhosis. A case-control study. Ann Intern Med. 1992;116(2):97–102. - PubMed
Publication types
MeSH terms
Substances
Associated data
Grants and funding
- N01 DK092324/DK/NIDDK NIH HHS/United States
- N01 DK092321/DK/NIDDK NIH HHS/United States
- N01 DK092320/DK/NIDDK NIH HHS/United States
- N01 DK092318/DK/NIDDK NIH HHS/United States
- N01 DK092327/DK/NIDDK NIH HHS/United States
- M01 RR006192/RR/NCRR NIH HHS/United States
- N01 DK092323/DK/NIDDK NIH HHS/United States
- M01 RR001066/RR/NCRR NIH HHS/United States
- N01 DK092326/DK/NIDDK NIH HHS/United States
- M01 RR000633/RR/NCRR NIH HHS/United States
- M01 RR000065/RR/NCRR NIH HHS/United States
- M01 RR000051/RR/NCRR NIH HHS/United States
- M01 RR000043/RR/NCRR NIH HHS/United States
- N01 DK092322/DK/NIDDK NIH HHS/United States
- M01 RR000042/RR/NCRR NIH HHS/United States
- N01 DK092325/DK/NIDDK NIH HHS/United States
- M01 RR000827/RR/NCRR NIH HHS/United States
- N01 DK092319/DK/NIDDK NIH HHS/United States
- N01 DK092328/DK/NIDDK NIH HHS/United States
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Molecular Biology Databases

