Tissue engineering using autologous microcirculatory beds as vascularized bioscaffolds
- PMID: 19001054
- PMCID: PMC2653982
- DOI: 10.1096/fj.08-114868
Tissue engineering using autologous microcirculatory beds as vascularized bioscaffolds
Abstract
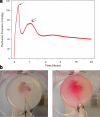
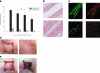
Classic tissue engineering paradigms are limited by the incorporation of a functional vasculature and a reliable means for reimplantation into the host circulation. We have developed a novel approach to overcome these obstacles using autologous explanted microcirculatory beds (EMBs) as bioscaffolds for engineering complex three-dimensional constructs. In this study, EMBs consisting of an afferent artery, capillary beds, efferent vein, and surrounding parenchymal tissue are explanted and maintained for 24 h ex vivo in a bioreactor that preserves EMB viability and function. Given the rapidly advancing field of stem cell biology, EMBs were subsequently seeded with three distinct stem cell populations, multipotent adult progenitor cells (MAPCs), and bone marrow and adipose tissue-derived mesenchymal stem cells (MSCs). We demonstrate MAPCs, as well as MSCs, are able to egress from the microcirculation into the parenchymal space, forming proliferative clusters. Likewise, human adipose tissue-derived MSCs were also found to egress from the vasculature and seed into the EMBs, suggesting feasibility of this technology for clinical applications. We further demonstrate that MSCs can be transfected to express a luciferase protein and continue to remain viable and maintain luciferase expression in vivo. By using the vascular network of EMBs, EMBs can be perfused ex vivo and seeded with stem cells, which can potentially be directed to differentiate into neo-organs or transfected to replace failing organs and deficient proteins.
Figures
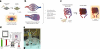



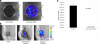
Similar articles
-
Matrix-mediated retention of adipogenic differentiation potential by human adult bone marrow-derived mesenchymal stem cells during ex vivo expansion.Biomaterials. 2005 Nov;26(31):6167-75. doi: 10.1016/j.biomaterials.2005.03.024. Biomaterials. 2005. PMID: 15913765
-
Contrasting effects of vasculogenic induction upon biaxial bioreactor stimulation of mesenchymal stem cells and endothelial progenitor cells cocultures in three-dimensional scaffolds under in vitro and in vivo paradigms for vascularized bone tissue engineering.Tissue Eng Part A. 2013 Apr;19(7-8):893-904. doi: 10.1089/ten.TEA.2012.0187. Epub 2012 Dec 16. Tissue Eng Part A. 2013. PMID: 23102089
-
Engineering of vascular grafts with genetically modified bone marrow mesenchymal stem cells on poly (propylene carbonate) graft.Artif Organs. 2006 Dec;30(12):898-905. doi: 10.1111/j.1525-1594.2006.00322.x. Artif Organs. 2006. PMID: 17181830
-
Tissue engineering technologies: just a quick note about transplantation of bioengineered donor trachea and augmentation cystoplasty by de novo engineered bladder tissue.G Chir. 2009 Nov-Dec;30(11-12):514-9. G Chir. 2009. PMID: 20109384 Review.
-
Adipose-derived stem cells and periodontal tissue engineering.Int J Oral Maxillofac Implants. 2013 Nov-Dec;28(6):e487-93. doi: 10.11607/jomi.te29. Int J Oral Maxillofac Implants. 2013. PMID: 24278946 Review.
Cited by
-
Stem cell recruitment after injury: lessons for regenerative medicine.Regen Med. 2012 Nov;7(6):833-50. doi: 10.2217/rme.12.82. Regen Med. 2012. PMID: 23164083 Free PMC article. Review.
-
Recellularization of Bioengineered Scaffolds for Vascular Composite Allotransplantation.Front Surg. 2022 May 25;9:843677. doi: 10.3389/fsurg.2022.843677. eCollection 2022. Front Surg. 2022. PMID: 35693318 Free PMC article. Review.
-
Biomimetic poly(ethylene glycol)-based hydrogels as scaffolds for inducing endothelial adhesion and capillary-like network formation.Biomacromolecules. 2012 Mar 12;13(3):706-13. doi: 10.1021/bm201596w. Epub 2012 Feb 22. Biomacromolecules. 2012. PMID: 22296572 Free PMC article.
-
In vitro fabrication of functional three-dimensional tissues with perfusable blood vessels.Nat Commun. 2013;4:1399. doi: 10.1038/ncomms2406. Nat Commun. 2013. PMID: 23360990 Free PMC article.
-
Heart regeneration with engineered myocardial tissue.Annu Rev Biomed Eng. 2014 Jul 11;16:1-28. doi: 10.1146/annurev-bioeng-071812-152344. Epub 2014 Apr 24. Annu Rev Biomed Eng. 2014. PMID: 24819474 Free PMC article. Review.
References
-
- Stock U A, Vacanti J P. Tissue engineering: current state and prospects. Annu Rev Med. 2001;52:443–451. - PubMed
-
- Kaihara S, Vacanti J P. Tissue engineering: toward new solutions for transplantation and reconstructive surgery. Arch Surg. 1999;134:1184–1188. - PubMed
-
- Hoganson D M, Pryor H I, 2nd, Vacanti J P. Tissue engineering and organ structure: a vascularized approach to liver and lung. Pediatr Res. 2008;63:520–526. - PubMed
-
- Mikos A G, McIntire L V, Anderson J M, Babensee J E. Host response to tissue engineered devices. Adv Drug Deliv Rev. 1998;33:111–139. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources

