Distal radius in adolescent girls with anorexia nervosa: trabecular structure analysis with high-resolution flat-panel volume CT
- PMID: 19011190
- PMCID: PMC2691811
- DOI: 10.1148/radiol.2492080173
Distal radius in adolescent girls with anorexia nervosa: trabecular structure analysis with high-resolution flat-panel volume CT
Abstract
Purpose: To examine trabecular microarchitecture with high-resolution flat-panel volume computed tomography (CT) and bone mineral density (BMD) with dual-energy x-ray absorptiometry (DXA) in adolescent girls with anorexia nervosa (AN) and to compare these results with those in normal-weight control subjects.
Materials and methods: The study was approved by the institutional review board and complied with HIPAA guidelines. Informed consent was obtained. Twenty adolescent girls, 10 with mild AN (mean age, 15.9 years; range, 13-18 years) and 10 age- and sex-matched normal-weight control subjects (mean age, 15.9 years; range, 12-18 years) underwent flat-panel volume CT of distal radius to determine apparent trabecular bone volume fraction (BV/TV), apparent trabecular number (TbN), apparent trabecular thickness (TbTh), and apparent trabecular separation (TbSp). All subjects underwent DXA of spine, hip, and whole body to determine BMD and body composition. The means and standard deviations (SDs) of structure parameters were calculated for AN and control groups. Groups were compared (Student t test). Linear regression analysis was performed.
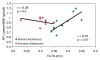
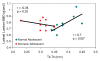
Results: AN subjects compared with control subjects, respectively, showed significantly lower mean values for BV/TV (0.37% +/- 0.05 [SD] vs 0.46% +/- 0.03, P = .0002) and TbTh (0.31 mm +/- 0.03 vs 0.39 mm +/- 0.03, P < .0001) and higher mean values for TbSp (0.54 mm +/- 0.13 vs 0.44 mm +/- 0.04, P = .02). TbN was lower in AN subjects than in control subjects, but the difference was not significant (1.17 mm(-3) +/- 0.15 vs 1.22 mm(-3) +/- 0.07, P = .43). There was no significant difference in BMD between AN and control subjects. BMD parameters showed positive correlation with BV/TV and TbTh in the control group (r = 0.55-0.84, P = .05-.01) but not in AN patients.
Conclusion: Flat-panel volume CT is effective in evaluation of trabecular structure in adolescent girls with AN and demonstrates that bone structure is abnormal in these patients compared with that in normal-weight control subjects despite normal BMD.
Supplemental material: http://radiology.rsnajnls.org/cgi/content/full/249/3/938/DC1.
RSNA, 2008
Figures




Similar articles
-
Women with anorexia nervosa: finite element and trabecular structure analysis by using flat-panel volume CT.Radiology. 2010 Oct;257(1):167-74. doi: 10.1148/radiol.10100222. Epub 2010 Aug 16. Radiology. 2010. PMID: 20713613 Free PMC article.
-
C-arm CT for histomorphometric evaluation of lumbar spine trabecular microarchitecture: a study on anorexia nervosa patients.Br J Radiol. 2013 Jul;86(1027):20120451. doi: 10.1259/bjr.20120451. Epub 2013 May 2. Br J Radiol. 2013. PMID: 23640801 Free PMC article.
-
Suboptimal bone microarchitecure in adolescent girls with obesity compared to normal-weight controls and girls with anorexia nervosa.Bone. 2019 May;122:246-253. doi: 10.1016/j.bone.2019.03.007. Epub 2019 Mar 7. Bone. 2019. PMID: 30853658 Free PMC article.
-
In vivo assessment of architecture and micro-finite element analysis derived indices of mechanical properties of trabecular bone in the radius.Osteoporos Int. 2002 Jan;13(1):6-17. doi: 10.1007/s198-002-8332-0. Osteoporos Int. 2002. PMID: 11878456
-
Adolescent girls with anorexia nervosa have impaired cortical and trabecular microarchitecture and lower estimated bone strength at the distal radius.J Clin Endocrinol Metab. 2013 May;98(5):1923-9. doi: 10.1210/jc.2012-4153. Epub 2013 Mar 18. J Clin Endocrinol Metab. 2013. PMID: 23509107 Free PMC article.
Cited by
-
Managing osteoporosis in ulcerative colitis: something new?World J Gastroenterol. 2014 Oct 21;20(39):14087-98. doi: 10.3748/wjg.v20.i39.14087. World J Gastroenterol. 2014. PMID: 25339798 Free PMC article. Review.
-
New Insights into Calorie Restriction Induced Bone Loss.Endocrinol Metab (Seoul). 2023 Apr;38(2):203-213. doi: 10.3803/EnM.2023.1673. Epub 2023 Apr 27. Endocrinol Metab (Seoul). 2023. PMID: 37150516 Free PMC article.
-
Update on the female athlete triad.Curr Rev Musculoskelet Med. 2013 Jun;6(2):195-204. doi: 10.1007/s12178-013-9168-9. Curr Rev Musculoskelet Med. 2013. PMID: 23613226 Free PMC article.
-
Associations between bone mineral density, body composition and amenorrhoea in females with eating disorders: a systematic review and meta-analysis.J Eat Disord. 2022 Nov 18;10(1):173. doi: 10.1186/s40337-022-00694-8. J Eat Disord. 2022. PMID: 36401318 Free PMC article. Review.
-
Anorexia Nervosa: Analysis of Trabecular Texture with CT.Radiology. 2017 Apr;283(1):178-185. doi: 10.1148/radiol.2016160970. Epub 2016 Oct 31. Radiology. 2017. PMID: 27797678 Free PMC article.
References
-
- Misra M, Aggarwal A, Miller KK, et al. Effects of anorexia nervosa on clinical, hematologic, biochemical, and bone density parameters in community-dwelling adolescent girls. Pediatrics 2004;114:1574–1583. - PubMed
-
- Vestergaard P, Emborg C, Stoving RK, Hagen C, Mosekilde L, Brixen K. Fractures in patients with anorexia nervosa, bulimia nervosa, and other eating disorders: a nationwide register study. Int J Eat Disord 2002;32:301–308. - PubMed
-
- Misra M, Klibanski A. Anorexia nervosa and osteoporosis. Rev Endocr Metab Disord 2006;7:91–99. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Molecular Biology Databases

