Coronary artery anomalies detected by MSCT-coronary angiography in the adult
- PMID: 19065275
- PMCID: PMC2584765
- DOI: 10.1007/BF03086181
Coronary artery anomalies detected by MSCT-coronary angiography in the adult
Abstract
Background: Before coronary evaluation by modern imaging techniques was feasible, premorbid diagnoses of coronary artery anomalies (CAAs) were usually made fortuitously by invasive coronary angiography (ICA). However, this technique is limited by its invasive and projectional nature. Coronary magnetic resonance angiography (CMRA) and multi-slice computed tomography (MSCT) broadened clinical information by enabling visualisation of the coronary arteries in their anatomical environment.
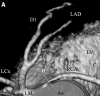
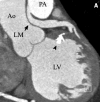
Methods: This case series visualises and reviews anomalous coronary artery from the opposite sinus (ACAOS) and coronary artery fistulae. All CAAs were detected by means of 64-slice dual source computed tomography after 1000 cardiac scans at the Erasmus MC, Rotterdam, the Netherlands.
Results: Eight ACAOS cases, one anomalous left coronary artery from the pulmonary artery (ALCAPA) and one congenital aneurysm of an aortic sinus were found. Seven out often detected CAAs were considered malignant whereas three CAAs of the ACAOS type (retroaortic path) were considered benign. Significant coronary artery disease was found in three out of eight ACAOS cases. In one of the ACAOS cases complete evaluation of the anomalous coronary artery was limited by motion artifacts. All five cases of right ACAOS were referred for MSCT because the right coronary artery could not be located by invasive angiography.
Conclusion: All CAAs were easy to diagnose because of 3D imaging and high temporal and spatial resolution. High resolution made it possible to not only depict coronary artery abnormalities, but also to quantify luminal and vessel properties such as stenosis grade, aspects of plaque, anomalous vessel length, luminal area ratio and the asymmetry ratio. Because of its comprehensiveness, MSCT can be an effective imaging modality in patients suspected of coronary artery abnormalities caused by coronary artery disease, CAAs, or a combination of both. (Neth Heart J 2008;16:369-75.).
Keywords: anomalous coronary artery from the opposite sinus; computed tomography; coronary anomalies; coronary artery fistulae; invasive coronary angiography.
Figures
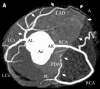


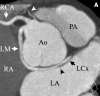


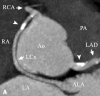


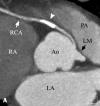








Similar articles
-
Prognostic value of dual-source computed tomography (DSCT) angiography characteristics in anomalous coronary artery from the opposite sinus (ACAOS) patients: a large-scale retrospective study.BMC Cardiovasc Disord. 2020 Jan 17;20(1):25. doi: 10.1186/s12872-019-01285-3. BMC Cardiovasc Disord. 2020. PMID: 31952479 Free PMC article.
-
Anomalous origin of coronary artery from the opposite aortic sinus of Valsalva-a single center experience with a therapeutic conundrum.Indian Heart J. 2021 May-Jun;73(3):289-294. doi: 10.1016/j.ihj.2021.03.012. Epub 2021 Apr 3. Indian Heart J. 2021. PMID: 34154744 Free PMC article.
-
Prevalence and characteristics of coronary anomalies originating from the opposite sinus of Valsalva in 8,522 patients referred for coronary computed tomography angiography.Am J Cardiol. 2013 May 1;111(9):1361-7. doi: 10.1016/j.amjcard.2013.01.280. Epub 2013 Feb 11. Am J Cardiol. 2013. PMID: 23411107
-
Therapeutic Management of Anomalous Coronary Arteries Originating From the Opposite Sinus of Valsalva: Current Evidence, Proposed Approach, and the Unknowing.J Am Heart Assoc. 2022 Oct 18;11(20):e027098. doi: 10.1161/JAHA.122.027098. Epub 2022 Oct 7. J Am Heart Assoc. 2022. PMID: 36205254 Free PMC article. Review.
-
Critical update and discussion of the prevalence, nature, mechanisms of action, and treatment options in potentially serious coronary anomalies.Trends Cardiovasc Med. 2023 Nov;33(8):518-528. doi: 10.1016/j.tcm.2022.05.007. Epub 2022 May 26. Trends Cardiovasc Med. 2023. PMID: 35643274 Review.
Cited by
-
Fingertip digital thermal monitoring: a fingerprint for cardiovascular disease?Int J Cardiovasc Imaging. 2010 Feb;26(2):249-52. doi: 10.1007/s10554-009-9552-0. Epub 2009 Dec 12. Int J Cardiovasc Imaging. 2010. PMID: 20012695 Free PMC article. No abstract available.
-
CT perfusion angiography; beware of artifacts!Int J Cardiovasc Imaging. 2010 Mar;26(3):355-8. doi: 10.1007/s10554-009-9559-6. Epub 2009 Dec 24. Int J Cardiovasc Imaging. 2010. PMID: 20033784 Free PMC article. No abstract available.
-
Non-significant left main disease; truly non-significant?Int J Cardiovasc Imaging. 2009 Apr;25(4):439-42. doi: 10.1007/s10554-009-9436-3. Epub 2009 Feb 17. Int J Cardiovasc Imaging. 2009. PMID: 19221891 No abstract available.
-
CT angiography; no collateral damage.Int J Cardiovasc Imaging. 2009 Mar;25(3):339-42. doi: 10.1007/s10554-009-9426-5. Epub 2009 Jan 22. Int J Cardiovasc Imaging. 2009. PMID: 19160068 No abstract available.
-
Anomalous aortic origin of coronary arteries from the opposite sinus: a critical appraisal of risk.BMC Cardiovasc Disord. 2012 Oct 1;12:83. doi: 10.1186/1471-2261-12-83. BMC Cardiovasc Disord. 2012. PMID: 23025810 Free PMC article. Review.
References
-
- Shi H Aschoff AJ, Brambs HJ, Hoffman MH. Multislice CT Imaging of anomalous coronary arteries. Eur Radiol 2004;14:2172-81. - PubMed
-
- Angelini P. Coronary Artery Anomalies; An Entity in search of an Identity. Circulation 2007;115:1296-305. - PubMed
-
- Angelini P, Trivellato M, Donis J, Leachman RD. Myocardial bridges: a review. Prog Cardiovasc Dis 1983;26:75-88. - PubMed
-
- Angelini P, Velasco JA, Ott D, Khoshnevis GR. Anomalous coronary artery arising from the opposite sinus: descriptive features and pathophysiologic mechanisms, as documented by intravascular ultrasonography. J Invasive Cardiol 2003;15:507-14. - PubMed
LinkOut - more resources
Full Text Sources
Miscellaneous
