Retinal ion regulation in a mouse model of diabetic retinopathy: natural history and the effect of Cu/Zn superoxide dismutase overexpression
- PMID: 19074809
- PMCID: PMC2688071
- DOI: 10.1167/iovs.08-2918
Retinal ion regulation in a mouse model of diabetic retinopathy: natural history and the effect of Cu/Zn superoxide dismutase overexpression
Abstract
Purpose: To test the hypotheses that manganese-enhanced MRI (MEMRI) is useful in evaluating intraretinal ion dysregulation in wild-type (WT) and Cu/Zn superoxide dismutase (SOD1) overexpressor mice.
Methods: Central intraretinal ion activity and retinal thickness were measured from high-resolution data of light- and dark-adapted WT C57BL/6 mice (to gauge MEMRI sensitivity to normal visual processing in mice) and dark-adapted diabetic and nondiabetic WT and Cu/Zn superoxide dismutase overexpressor (SOD1OE) mice. Glycated hemoglobin and retinal vascular histopathology were also determined.
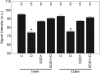
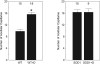
Results: In WT mice, light adaptation reduced outer retinal manganese uptake compared with that in dark adaptation; no effect on inner retinal uptake was found. In diabetic WT mice, intraretinal manganese uptake became subnormal between 1.5 and 4 months of diabetes onset and then relatively increased. Central retinal thickness, as determined with MEMRI, decreased as a function of age in diabetic mice but remained constant in control mice. Nondiabetic SOD1OE mice had normal retinal manganese uptake but subnormal retinal thickness and supernormal acellular capillary density. At 4.2 months of diabetes, SOD1OE mice had normal manganese uptake and no further thinning; acellular capillaries frequency did not increase by 9 to 10 months of diabetes.
Conclusions: In emerging diabetic retinopathy, MEMRI provided an analytic measure of an ionic dysregulatory pattern that was sensitive to SOD1 overexpression. The potential benefit of SOD1 overexpression to inhibit retinal abnormality in this model is limited by the retinal and vascular degeneration that develops independently of diabetes.
Figures


Similar articles
-
Acute systemic 11-cis-retinal intervention improves abnormal outer retinal ion channel closure in diabetic mice.Mol Vis. 2012;18:372-6. Epub 2012 Feb 7. Mol Vis. 2012. PMID: 22355248 Free PMC article.
-
Quantitative mapping of ion channel regulation by visual cycle activity in rodent photoreceptors in vivo.Invest Ophthalmol Vis Sci. 2009 Apr;50(4):1880-5. doi: 10.1167/iovs.08-2958. Epub 2008 Dec 5. Invest Ophthalmol Vis Sci. 2009. PMID: 19060264 Free PMC article.
-
Impaired apparent ion demand in experimental diabetic retinopathy: correction by lipoic Acid.Invest Ophthalmol Vis Sci. 2007 Oct;48(10):4753-8. doi: 10.1167/iovs.07-0433. Invest Ophthalmol Vis Sci. 2007. PMID: 17898301
-
Oxidative damage in the retinal mitochondria of diabetic mice: possible protection by superoxide dismutase.Invest Ophthalmol Vis Sci. 2007 Aug;48(8):3805-11. doi: 10.1167/iovs.06-1280. Invest Ophthalmol Vis Sci. 2007. PMID: 17652755
-
Retinopathy is reduced during experimental diabetes in a mouse model of outer retinal degeneration.Invest Ophthalmol Vis Sci. 2006 Dec;47(12):5561-8. doi: 10.1167/iovs.06-0647. Invest Ophthalmol Vis Sci. 2006. PMID: 17122149
Cited by
-
Adrenergic and serotonin receptors affect retinal superoxide generation in diabetic mice: relationship to capillary degeneration and permeability.FASEB J. 2015 May;29(5):2194-204. doi: 10.1096/fj.14-269431. Epub 2015 Feb 9. FASEB J. 2015. PMID: 25667222 Free PMC article.
-
Photobiomodulation Mitigates Diabetes-Induced Retinopathy by Direct and Indirect Mechanisms: Evidence from Intervention Studies in Pigmented Mice.PLoS One. 2015 Oct 1;10(10):e0139003. doi: 10.1371/journal.pone.0139003. eCollection 2015. PLoS One. 2015. PMID: 26426815 Free PMC article.
-
Evidence for diffuse central retinal edema in vivo in diabetic male Sprague Dawley rats.PLoS One. 2012;7(1):e29619. doi: 10.1371/journal.pone.0029619. Epub 2012 Jan 11. PLoS One. 2012. PMID: 22253747 Free PMC article.
-
Low-intensity far-red light inhibits early lesions that contribute to diabetic retinopathy: in vivo and in vitro.Invest Ophthalmol Vis Sci. 2013 May 1;54(5):3681-90. doi: 10.1167/iovs.12-11018. Invest Ophthalmol Vis Sci. 2013. PMID: 23557732 Free PMC article.
-
Successful induction of diabetes in mice demonstrates no gender difference in development of early diabetic retinopathy.PLoS One. 2020 Sep 17;15(9):e0238727. doi: 10.1371/journal.pone.0238727. eCollection 2020. PLoS One. 2020. PMID: 32941450 Free PMC article.
References
-
- Grunwald JE, Riva CE, Brucker AJ, Sinclair SH, Petrig BL. Altered retinal vascular response to 100% oxygen breathing in diabetes mellitus. Ophthalmology. 1984;91(12):1447–1452. - PubMed
-
- Sinclair SH, Grunwald JE, Riva CE, Braunstein SN, Nichols CW, Schwartz SS. Retinal vascular autoregulation in diabetes mellitus. Ophthalmology. 1982;89(7):748–750. - PubMed
-
- Trick GL, Berkowitz BA. Retinal oxygenation response and retinopathy. Prog Retin Eye Res. 2005;24(2):259–274. - PubMed
-
- Phipps JA, Fletcher EL, Vingrys AJ. Paired-flash identification of rod and cone dysfunction in the diabetic rat. Invest Ophthalmol Vis Sci. 2004;45(12):4592–4600. - PubMed
-
- Han Y, Bearse MA, Jr, Schneck ME, Barez S, Jacobsen CH, Adams AJ. Multifocal electroretinogram delays predict sites of subsequent diabetic retinopathy. Invest Ophthalmol Vis Sci. 2004;45(3):948–954. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Molecular Biology Databases
Miscellaneous

