The impact of adverse events in the intensive care unit on hospital mortality and length of stay
- PMID: 19091089
- PMCID: PMC2621200
- DOI: 10.1186/1472-6963-8-259
The impact of adverse events in the intensive care unit on hospital mortality and length of stay
Abstract
Background: Adverse events (AEs) are patient injuries caused by medical care. Previous studies have reported increased mortality rates and prolonged hospital length of stay in patients having an AE. However, these studies have not adequately accounted for potential biases which might influence these associations. We performed this study to measure the independent influence of intensive care unit (ICU) based AEs on in-hospital mortality and hospital length of stay.
Methods: Prospective cohort study in an academic tertiary-care ICU. Patients were monitored daily for adverse clinical occurrences. Data about adverse clinical occurrences were reviewed by a multidisciplinary team who rated whether they were AEs and whether they were preventable. We determined the association of AEs in the ICU with time to death and time to hospital discharge using multivariable survival analysis models.
Results: We evaluated 207 critically ill patients (81% required mechanical ventilation, median Glasgow Coma Scale = 8, median predicted mortality = 31%). Observed mortality rate and hospital length of stay were 25% (95% CI 19%-31%) and 15 days (IQR 8-34 days), respectively. ICU-based AEs and preventable AEs occurred in 40 patients (19%, 95% CI 15%-25%) and 21 patients (10%, 95% CI 7%-15%), respectively. ICU-based AEs and preventable AEs were not significantly associated with time to in-hospital death (HR = 0.93, 95% CI 0.44-1.98 and HR = 0.72 95% CI 0.25-2.04, respectively). ICU-based AEs and preventable AEs were independently associated with time to hospital discharge ((HR = 0.50, 95% CI 0.31-0.81 and HR = 0.46 95% CI 0.23-0.91, respectively)). ICU-based AEs were associated with an average increase in hospital length of stay of 31 days.
Conclusion: The impact of AEs on hospital length of stay was clinically relevant. Larger studies are needed to conclusively measure the association between preventable AEs and patient outcomes.
Figures
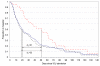
References
-
- The Institute of Medicine . To err is human: building a safer health system. National Academy Press, Washington D.C.; 2000.
-
- Brennan TA, Leape LL, Laird NM, Hebert L, Localio AR, Lawthers AG, Newhouse JP, Weiler PC, Hiatt HH. Incidence of adverse events and negligence in hospitalized patients. Results of the Harvard Medical Practice Study I. New England Journal of Medicine. 1991;324:370–376. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources

