Clinical practice guidelines for hospital-acquired pneumonia and ventilator-associated pneumonia in adults
- PMID: 19145262
- PMCID: PMC2610276
- DOI: 10.1155/2008/593289
Clinical practice guidelines for hospital-acquired pneumonia and ventilator-associated pneumonia in adults
Erratum in
-
Erratum.Can J Infect Dis Med Microbiol. 2008 Nov;19(6):438. Can J Infect Dis Med Microbiol. 2008. PMID: 19436576 Free PMC article.
Abstract
Hospital-acquired pneumonia (HAP) and ventilator-associated pneumonia (VAP) are important causes of morbidity and mortality, with mortality rates approaching 62%. HAP and VAP are the second most common cause of nosocomial infection overall, but are the most common cause documented in the intensive care unit setting. In addition, HAP and VAP produce the highest mortality associated with nosocomial infection. As a result, evidence-based guidelines were prepared detailing the epidemiology, microbial etiology, risk factors and clinical manifestations of HAP and VAP. Furthermore, an approach based on the available data, expert opinion and current practice for the provision of care within the Canadian health care system was used to determine risk stratification schemas to enable appropriate diagnosis, antimicrobial management and nonantimicrobial management of HAP and VAP. Finally, prevention and risk-reduction strategies to reduce the risk of acquiring these infections were collated. Future initiatives to enhance more rapid diagnosis and to effect better treatment for resistant pathogens are necessary to reduce morbidity and improve survival.
La pneumonie nosocomiale (PN) et la pneumonie sous ventilation assistée (PVA) sont d’importantes causes de morbidité et de mortalité, les taux de mortalité avoisinant les 62 %. Dans l’ensemble, la PN et la PVA constituent la deuxième cause d’infection nosocomiale en importance, mais la principale cause documentée à l’unité de soins intensifs. De plus, la PN et la PVA produisent le plus fort taux de mortalité imputable à une infection nosocomiale. C’est pourquoi on a préparé des lignes directrices probantes détaillant l’épidémiologie, l’étiologie microbienne, les facteurs de risque et les manifestations cliniques de la PN et de la PVA. De plus, une démarche axée sur les données disponibles, l’opinion d’experts et les pratiques courantes de prestation des soins au sein du système de santé canadien ont permis de déterminer les schèmes de stratification des risques afin de favoriser un diagnostic pertinent, la prise en charge antimicrobienne et la prise en charge non antimicrobienne de la PN et de la PVA. Enfin, on a colligé des stratégies de prévention et de réduction des risques afin de réduire le risque d’acquérir ces infections. De futures initiatives en vue de favoriser un diagnostic plus rapide et d’assurer le meilleur traitement des pathogènes résistants s’imposent pour réduire la morbidité et accroître le taux de survie.
Keywords: Guidelines; Hospital-acquired; Pneumonia; Ventilator-associated.
Figures

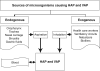
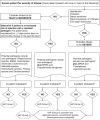



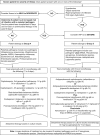
References
-
- Tablan OC, Anderson LJ, Besser R, Bridges C, Hajjeh R. Guidelines for preventing health-care-associated pneumonia, 2003: Recommendations of CDC and the Healthcare Infection Control Practices Advisory Committee. MMWR Recomm Rep. 2004;53:1–36. - PubMed
-
- Hospital-acquired pneumonia in adults: Diagnosis, assessment of severity, initial antimicrobial therapy, and preventive strategies. A consensus statement, American Thoracic Society, November 1995. Am J Respir Crit Care Med. 1996;153:1711–25. - PubMed
-
- Garner JS, Jarvis WR, Emori TG, Horan TC, Hughes JM. CDC definitions for nosocomial infections, 1988. Am J Infect Control. 1988;16:128–40. (Erratum in 1988 Aug;16:177.) - PubMed
-
- Ibrahim EH, Ward S, Sherman G, Kollef MH. A comparative analysis of patients with early-onset vs late-onset nosocomial pneumonia in the ICU setting. Chest. 2000;117:1434–42. - PubMed
-
- Trouillet JL, Chastre J, Vuagnat A, et al. Ventilator-associated pneumonia caused by potentially drug-resistant bacteria. Am J Respir Crit Care Med. 1998;157:531–9. - PubMed
LinkOut - more resources
Full Text Sources
Medical
Research Materials

