Adherence to first-line antiretroviral therapy affects non-virologic outcomes among patients on treatment for more than 12 months in Lusaka, Zambia
- PMID: 19223334
- PMCID: PMC2689395
- DOI: 10.1093/ije/dyp004
Adherence to first-line antiretroviral therapy affects non-virologic outcomes among patients on treatment for more than 12 months in Lusaka, Zambia
Abstract
Background: High-level adherence to antiretroviral therapy (ART) is associated with favourable patient outcomes. In resource-constrained settings, however, there are few validated measures. We examined the correlation between clinical outcomes and the medication possession ratio (MPR), a pharmacy-based measure of adherence.
Methods: We analysed data from a large programmatic cohort across 18 primary care centres providing ART in Lusaka, Zambia. Patients were stratified into three categories based on MPR-calculated adherence over the first 12 months: optimal (> or =95%), suboptimal (80-94%) and poor (<80%).
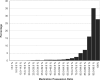
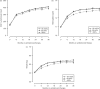
Results: Overall, 27 115 treatment-naïve adults initiated and continued ART for > or =12 months: 17 060 (62.9%) demonstrated optimal adherence, 7682 (28.3%) had suboptimal adherence and 2373 (8.8%) had poor adherence. When compared with those with optimal adherence, post-12-month mortality risk was similar among patients with sub-optimal adherence [adjusted hazard ratio (AHR) = 1.0; 95% CI: 0.9-1.2] but higher in patients with poor adherence (AHR = 1.7; 95% CI: 1.4-2.2). Those <80% MPR also appeared to have an attenuated CD4 response at 18 months (185 cells/microl vs 217 cells/microl; P < 0.001), 24 months (213 cells/microl vs 246 cells/microl; P < 0.001), 30 months (226 cells/microl vs 261 cells/microl; P < 0.001) and 36 months (245 cells/microl vs 275 cells/microl; P < 0.01) when compared with those above this threshold.
Conclusions: MPR was predictive of clinical outcomes and immunologic response in this large public sector antiretroviral treatment program. This marker may have a role in guiding programmatic monitoring and clinical care in resource-constrained settings.
Figures

References
-
- Sethi AK, Celentano DD, Gange SJ, Moore RD, Gallant JE. Association between adherence to antiretroviral therapy and human immunodeficiency virus drug resistance. Clin Infect Dis. 2003;37:1112–18. - PubMed
-
- Moatti JP, Spire B, Kazatchkine M. Drug resistance and adherence to HIV/AIDS antiretroviral treatment: against a double standard between the north and the south. AIDS. 2004;18(Suppl 3):S55–61. - PubMed
-
- Wainberg MA, Friedland G. Public health implications of antiretroviral therapy and HIV drug resistance. JAMA. 1998;279:1977–83. - PubMed
-
- Harries AD, Nyangulu DS, Hargreaves NJ, Kaluwa O, Salaniponi FM. Preventing antiretroviral anarchy in sub-Saharan Africa. Lancet. 2001;358:410–14. - PubMed
-
- Nieuwkerk PT, Sprangers MA, Burger DM, et al. Limited patient adherence to highly active antiretroviral therapy for HIV-1 infection in an observational cohort study. Arch Intern Med. 2001;161:1962–68. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Research Materials

