Allogeneic mesenchymal precursor cell therapy to limit remodeling after myocardial infarction: the effect of cell dosage
- PMID: 19231391
- PMCID: PMC3021253
- DOI: 10.1016/j.athoracsur.2008.11.057
Allogeneic mesenchymal precursor cell therapy to limit remodeling after myocardial infarction: the effect of cell dosage
Abstract
Background: This experiment assessed the dose-dependent effect of a unique allogeneic STRO-3-positive mesenchymal precursor cell (MPC) on postinfarction left ventricular (LV) remodeling. The MPCs were administered in a manner that would simulate an off-the-self, early postinfarction, preventative approach to cardiac cell therapy in a sheep transmural myocardial infarct (MI) model.
Methods: Allogeneic MPCs were isolated from male crossbred sheep. Forty-six female sheep underwent coronary ligation to produce a transmural LV anteroapical infarction. One hour after infarction, the borderzone myocardium received an injection of 25, 75, 225, or 450 x 10(6) MPCs, or cell medium. Echocardiography was performed at 4 and 8 weeks after MI to quantify LV end-diastolic (LVEDV) and end-systolic volumes (LVESV), ejection fraction (EF), and infarct expansion. CD31 and smooth muscle actin (SMA) immunohistochemical staining was performed on infarct and borderzone specimens to quantify vascular density.
Results: Compared with controls, low-dose (25 and 75 x 10(6) cells) MPC treatment significantly attenuated infarct expansion and increases in LVEDV and LVESV. EF was improved at all cell doses. CD31 and SMA immunohistochemical staining demonstrated increased vascular density in the borderzone only at the lower cell doses. There was no evidence of myocardial regeneration within the infarct.
Conclusion: Allogeneic STRO-3 positive MPCs attenuate the remodeling response to transmural MI in a clinically relevant large-animal model. This effect is associated with vasculogenesis and arteriogenesis within the borderzone and infarct and is most pronounced at lower cell doses.
Figures



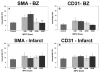


Comment in
-
Invited commentary.Ann Thorac Surg. 2009 Mar;87(3):801-2. doi: 10.1016/j.athoracsur.2008.12.087. Ann Thorac Surg. 2009. PMID: 19231392 No abstract available.
References
-
- Gheorghiade M, Bonow RO. Chronic heart failure in the United States: a manifestation of coronary artery disease. Circulation. 1998;97:282–9. - PubMed
-
- Lipinski MJ, Biondi-Zoccai GG, Abbate A, et al. Impact of intracoronary cell therapy on left ventricular function in the setting of acute myocardial infarction: a collaborative systematic review and meta-analysis of controlled clinical trials. J Am Coll Cardiol. 2007;50:1761–7. - PubMed
-
- Assmus B, Honold J, Schächinger V, et al. Transcoronary transplantation of progenitor cells after myocardial infarction. N Engl J Med. 2006;355:1222–32. - PubMed
-
- Schächinger V, Erbs S, Elsässer A, et al. Intracoronary bone marrow–derived progenitor cells in acute myocardial infarction. N Engl J Med. 2006;355:1210–21. - PubMed
-
- Oettgen P. Cardiac stem cell therapy: need for optimization of efficacy and safety monitoring. Circulation. 2006;114:353–8. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

