Video-assisted thoracic surgery (VATS) as a safe alternative for the resection of pulmonary metastases: a retrospective cohort study
- PMID: 19239710
- PMCID: PMC2654561
- DOI: 10.1186/1749-8090-4-13
Video-assisted thoracic surgery (VATS) as a safe alternative for the resection of pulmonary metastases: a retrospective cohort study
Abstract
Background: VATS has become a preferred method for benign surgical conditions, yet still remains controversial for malignancies. The purpose of this study was to review our results of pulmonary metastasectomies using both conventional open thoracotomy and VATS techniques.
Methods: This is a retrospective chart review of pulmonary metastasectomies performed from 1986 to 2006. The surgical approach used for the initial pulmonary metastasectomy was either open thoracotomy or VATS. Main outcomes were overall survival and recurrence free survival, evaluated using Kaplan Meier analysis. A non-inferiority margin was set at 0.2.
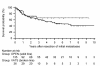
Results: A total of 280 surgical procedures were performed on 186 patients. From 171 eligible individuals, 135 patients were treated with thoracotomy (82 M, 53 F; median age 49 years), and 36 with VATS (18 M, 18 F; median age 58.5 years). Primary cancers were mainly: 81 sarcoma (47%), 26 colorectal adenocarcinoma (15%) and 22 renal cell carcinoma (13%). Median postoperative follow was 26.2 months. The conversion rate was 10.3% and there were no cases of pleural cavity seeding. The 5-year overall survival rates were 58.8% for thoracotomy and 69.6% for VATS, with median overall survival of 53.2 months and 30.1 months, respectively (p = 0.03). The estimated difference in 5-year overall survival was 10.8%. Second occurrences were noted in 59 thoracotomy and 10 VATS patients. The 5-year recurrence free survival rates were 51% in thoracotomy and 67% in VATS (p = 0.27), with median recurrence free survival of 24.8 months and 25.6 months, respectively.
Conclusion: In cases of pulmonary metastases, VATS is an acceptable alternative that is both safe and efficacious. Non-inferiority analysis of 5-year overall survival demonstrates that VATS is equivalent to thoracotomy. VATS patients also have a longer recurrence free survival. Based on our experience, it is permissible to use VATS resection in these circumstances: small tumor, fewer nodules, single lesion, age < or = 53, unilateral, tumor size amenable to wedge resection, and non-recurrent disease.
Figures

References
-
- Whitson B, Andrade R, Boettcher A, Bardales R, Kratzke R, Dahlberg P, Maddaus M. Video-assisted thoracoscopic surgery is more favorable than thoracotomy for resection of clinical stage I non-small cell lung cancer. Ann Thorac Surg. 2007;83:1965–1970. doi: 10.1016/j.athoracsur.2007.01.049. - DOI - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

