Abnormal insulin sensitivity persists up to three years in pediatric patients post-burn
- PMID: 19240154
- PMCID: PMC2684478
- DOI: 10.1210/jc.2008-1947
Abnormal insulin sensitivity persists up to three years in pediatric patients post-burn
Abstract
Context: The acute hypermetabolic response post-burn is associated with insulin resistance and hyperglycemia, significantly contributing to adverse outcome of these patients.
Objective: The aim of the study was to examine the persistence of abnormalities of various clinical parameters commonly utilized to assess the degree of insulin resistance in severely burned children for up to 3 yr after the burn injury.
Design, setting and patients: A total of 194 severely burned pediatric patients, admitted to our institute between 2002 and 2007, were enrolled in this prospective study and compared to a cohort of 95 nonburned, noninjured children.
Main outcome measures: Urinary cortisol, epinephrine, and norepinephrine, serum cytokines, and resting energy requirements were determined at admission and 1, 2, 6, 9, 12, 18, 24, and 36 months post-burn. A 75-g oral glucose tolerance test was performed at similar time points; serum glucose, insulin, and C-peptide were measured; and insulin sensitivity indices, such as ISI Matsuda, homeostasis model assessment, quantitative insulin sensitivity check index, and ISI Cederholm, were calculated. Statistical analysis was performed by ANOVA with Bonferroni correction with significance accepted at P < 0.05.
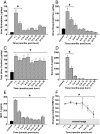
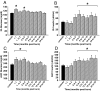
Results: Urinary cortisol and catecholamines, serum IL-7, IL-10, IL-12, macrophage inflammatory protein-1b, monocyte chemoattractant protein-1, and resting energy requirements were significantly increased for up to 36 months post-burn (P < 0.05). Glucose values were significantly augmented for 6 months post-burn (P < 0.05), associated with significant increases in serum C-peptide and insulin that remained significantly increased for 36 months compared to nonburned children (P < 0.05). Insulin sensitivity indices, ISI Matsuda, ISI quantitative insulin sensitivity check index, and homeostasis model assessment were abnormal throughout the whole study period, indicating peripheral and whole body insulin resistance. The insulinogenic index displayed physiological values, indicating normal pancreatic beta-cell function.
Conclusions: A severe burn is associated with stress-induced insulin resistance that persists not only during the acute phase but also for up to 3 yr post-burn.
Trial registration: ClinicalTrials.gov NCT00673309.
Figures


References
-
- Hart DW, Wolf SE, Mlcak R, Chinkes DL, Ramzy PI, Obeng MK, Ferrando AA, Wolfe RR, Herndon DN 2000 Persistence of muscle catabolism after severe burn. Surgery 128:312–319 - PubMed
-
- Przkora R, Barrow RE, Jeschke MG, Suman OE, Celis M, Sanford AP, Chinkes DL, Mlcak RP, Herndon DN 2006 Body composition changes with time in pediatric burn patients. J Trauma 60:968–971 - PubMed
-
- Herndon DN, Tompkins RG 2004 Support of the metabolic response to burn injury. Lancet 363:1895–1902 - PubMed
Publication types
MeSH terms
Substances
Associated data
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Research Materials

