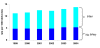Trends in adverse maternal outcomes during childbirth: a population-based study of severe maternal morbidity
- PMID: 19243578
- PMCID: PMC2653462
- DOI: 10.1186/1471-2393-9-7
Trends in adverse maternal outcomes during childbirth: a population-based study of severe maternal morbidity
Abstract
Background: Maternal mortality is too rare in high income countries to be used as a marker of the quality of maternity care. Consequently severe maternal morbidity has been suggested as a better indicator. Using the maternal morbidity outcome indicator (MMOI) developed and validated for use in routinely collected population health data, we aimed to determine trends in severe adverse maternal outcomes during the birth admission and in particular to examine the contribution of postpartum haemorrhage (PPH).
Methods: We applied the MMOI to the linked birth-hospital discharge records for all women who gave birth in New South Wales, Australia from 1999 to 2004 and determined rates of severe adverse maternal outcomes. We used frequency distributions and contingency table analyses to examine the association between adverse outcomes and maternal, pregnancy and birth characteristics, among all women and among only those with PPH. Using logistic regression, we modelled the effects of these characteristics on adverse maternal outcomes. The impact of adverse outcomes on duration of hospital admission was also examined.
Results: Of 500,603 women with linked birth and hospital records, 6242 (12.5 per 1,000) suffered an adverse outcome, including 22 who died. The rate of adverse maternal outcomes increased from 11.5 in 1999 to 13.8 per 1000 deliveries in 2004, an annual increase of 3.8% (95%CI 2.3-5.3%). This increase occurred almost entirely among women with a PPH. Changes in pregnancy and birth factors during the study period did not account for increases in adverse outcomes either overall, or among the subgroup of women with PPH. Among women with severe adverse outcomes there was a 12% decrease in hospital days over the study period, whereas women with no severe adverse outcome occupied 23% fewer hospital days in 2004 than in 1999.
Conclusion: Severe adverse maternal outcomes associated with childbirth have increased in Australia and the increase was entirely among women who experienced a PPH. Reducing or stabilising PPH rates would halt the increase in adverse maternal outcomes.
Figures
References
-
- CEMACH Saving Mothers' Lives: Reviewing maternal deaths to make motherhood safer 2003–2005. London. 2007. http://www.cemach.org.uk/Publications/CEMACH-Publications/Maternal-and-P...
-
- Slaytor EK, Sullivan EA, King JF. Maternal deaths in Australia 1997–1999. Sydney: AIHW National Perinatal Statistics Unit (Maternal Deaths Series No. 1); 2004. pp. 14–16.
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources