Contribution of the carotid body chemoreceptors to eupneic ventilation in the intact, unanesthetized dog
- PMID: 19246650
- PMCID: PMC2681333
- DOI: 10.1152/japplphysiol.91590.2008
Contribution of the carotid body chemoreceptors to eupneic ventilation in the intact, unanesthetized dog
Abstract
We used extracorporeal perfusion of the reversibly isolated carotid sinus region to determine the effects of specific carotid body (CB) chemoreceptor inhibition on eupneic ventilation (Vi) in the resting, awake, intact dog. Four female spayed dogs were studied during wakefulness when CB was perfused with 1) normoxic, normocapnic blood; and 2) hyperoxic (>500 mmHg), hypocapnic ( approximately 20 mmHg) blood to maximally inhibit the CB tonic activity. We found that CB perfusion per se (normoxic-normocapnic) had no effect on Vi. CB inhibition caused marked reductions in Vi (-60%, range 49-80%) and inspiratory flow rate (-58%, range 44-87%) 24-41 s following the onset of CB perfusion. Thereafter, a partial compensatory response was observed, and a steady state in Vi was reached after 50-76 s following the onset of CB perfusion. This steady-state tidal volume-mediated hypoventilation ( approximately 31%) coincided with a significant reduction in mean diaphragm electromyogram (-24%) and increase in mean arterial pressure (+12 mmHg), which persisted for 7-25 min until CB perfusion was stopped, despite a substantial increase in CO(2) retention (+9 Torr, arterial Pco(2)) and systemic respiratory acidosis. We interpret these data to mean that CB chemoreceptors contribute more than one-half to the total eupneic drive to breathe in the normoxic, intact, awake animal. We speculate that this CB contribution consists of both the normal tonic sensory input from the CB chemoreceptors to medullary respiratory controllers, as well as a strong modulatory effect on central chemoreceptor responsiveness to CO(2).
Figures
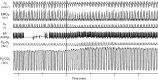




References
-
- Aitken ML, Franklin JL, Pierson DJ, Schoene RB. Influence of body size and gender on control of ventilation. J Appl Physiol 60: 1894–1899, 1986. - PubMed
-
- Bisgard GE, Forster HV, Klein JP. Recovery of peripheral chemoreceptor function after denervation in ponies. J Appl Physiol 49: 964–970, 1980. - PubMed
-
- Bisgard GE, Forster HV, Orr JA, Buss DD, Rawlings CA, Rasmussen B. Hypoventilation in ponies after carotid body denervation. J Appl Physiol 40: 184–190, 1976. - PubMed
-
- Bouverot P, Candas V, Libert JP. Role of the arterial chemoreceptors in ventilatory adaptation to hypoxia of awake dogs and rabbits. Respir Physiol 17: 209–219, 1973. - PubMed
-
- Busch MA, Bisgard GE, Mesina JE, Forster HV. The effects of unilateral carotid body excision on ventilatory control in goats. Respir Physiol 54: 353–361, 1983. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources

