Resolution of established cardiac hypertrophy and fibrosis and prevention of systolic dysfunction in a transgenic rabbit model of human cardiomyopathy through thiol-sensitive mechanisms
- PMID: 19255346
- PMCID: PMC2773801
- DOI: 10.1161/CIRCULATIONAHA.108.790501
Resolution of established cardiac hypertrophy and fibrosis and prevention of systolic dysfunction in a transgenic rabbit model of human cardiomyopathy through thiol-sensitive mechanisms
Abstract
Background: Cardiac hypertrophy, the clinical hallmark of hypertrophic cardiomyopathy (HCM), is a major determinant of morbidity and mortality not only in HCM but also in a number of cardiovascular diseases. There is no effective therapy for HCM and generally for cardiac hypertrophy. Myocardial oxidative stress and thiol-sensitive signaling molecules are implicated in pathogenesis of hypertrophy and fibrosis. We posit that treatment with N-acetylcysteine, a precursor of glutathione, the largest intracellular thiol pool against oxidative stress, could reverse cardiac hypertrophy and fibrosis in HCM.
Methods and results: We treated 2-year-old beta-myosin heavy-chain Q403 transgenic rabbits with established cardiac hypertrophy and preserved systolic function with N-acetylcysteine or a placebo for 12 months (n=10 per group). Transgenic rabbits in the placebo group had cardiac hypertrophy, fibrosis, systolic dysfunction, increased oxidized to total glutathione ratio, higher levels of activated thiol-sensitive active protein kinase G, dephosphorylated nuclear factor of activated T cells (NFATc1) and phospho-p38, and reduced levels of glutathiolated cardiac alpha-actin. Treatment with N-acetylcysteine restored oxidized to total glutathione ratio, normalized levels of glutathiolated cardiac alpha-actin, reversed cardiac and myocyte hypertrophy and interstitial fibrosis, reduced the propensity for ventricular arrhythmias, prevented cardiac dysfunction, restored myocardial levels of active protein kinase G, and dephosphorylated NFATc1 and phospho-p38.
Conclusions: Treatment with N-acetylcysteine, a safe prodrug against oxidation, reversed established cardiac phenotype in a transgenic rabbit model of human HCM. Because there is no effective pharmacological therapy for HCM and given that hypertrophy, fibrosis, and cardiac dysfunction are common and major predictors of clinical outcomes, the findings could have implications in various cardiovascular disorders.
Figures
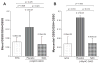





Similar articles
-
Prevention of cardiac hypertrophy by atorvastatin in a transgenic rabbit model of human hypertrophic cardiomyopathy.Circ Res. 2005 Aug 5;97(3):285-92. doi: 10.1161/01.RES.0000177090.07296.ac. Epub 2005 Jul 14. Circ Res. 2005. PMID: 16020756 Free PMC article.
-
Hypertrophy Regression With N-Acetylcysteine in Hypertrophic Cardiomyopathy (HALT-HCM): A Randomized, Placebo-Controlled, Double-Blind Pilot Study.Circ Res. 2018 Apr 13;122(8):1109-1118. doi: 10.1161/CIRCRESAHA.117.312647. Epub 2018 Mar 14. Circ Res. 2018. PMID: 29540445 Free PMC article. Clinical Trial.
-
Evolution of expression of cardiac phenotypes over a 4-year period in the beta-myosin heavy chain-Q403 transgenic rabbit model of human hypertrophic cardiomyopathy.J Mol Cell Cardiol. 2004 May;36(5):663-73. doi: 10.1016/j.yjmcc.2004.02.010. J Mol Cell Cardiol. 2004. PMID: 15135661 Free PMC article.
-
Experimental therapies in hypertrophic cardiomyopathy.J Cardiovasc Transl Res. 2009 Dec;2(4):483-92. doi: 10.1007/s12265-009-9132-7. Epub 2009 Oct 1. J Cardiovasc Transl Res. 2009. PMID: 20560006 Free PMC article. Review.
-
An insight of novel pharmacological therapies in hypertrophic cardiomyopathy.Med Chem. 2011 Jul;7(4):275-85. doi: 10.2174/157340611796150941. Med Chem. 2011. PMID: 21568880 Review.
Cited by
-
N-acetylcysteine Plus Deferoxamine Improves Cardiac Function in Wistar Rats After Non-reperfused Acute Myocardial Infarction.J Cardiovasc Transl Res. 2015 Jul;8(5):328-37. doi: 10.1007/s12265-015-9633-5. Epub 2015 Jun 18. J Cardiovasc Transl Res. 2015. PMID: 26085187
-
Pushing the Limits of Medical Management in HCM: A Review of Current Pharmacological Therapy Options.Int J Mol Sci. 2021 Jul 5;22(13):7218. doi: 10.3390/ijms22137218. Int J Mol Sci. 2021. PMID: 34281272 Free PMC article. Review.
-
Mechano-energetic uncoupling in hypertrophic cardiomyopathy: Pathophysiological mechanisms and therapeutic opportunities.J Mol Cell Cardiol Plus. 2023 May 6;4:100036. doi: 10.1016/j.jmccpl.2023.100036. eCollection 2023 Jun. J Mol Cell Cardiol Plus. 2023. PMID: 39801694 Free PMC article. Review.
-
Human cardiomyopathy mutations induce myocyte hyperplasia and activate hypertrophic pathways during cardiogenesis in zebrafish.Dis Model Mech. 2011 May;4(3):400-10. doi: 10.1242/dmm.006148. Epub 2011 Jan 18. Dis Model Mech. 2011. PMID: 21245263 Free PMC article.
-
Muscle dysfunction in hypertrophic cardiomyopathy: what is needed to move to translation?J Muscle Res Cell Motil. 2014 Feb;35(1):37-45. doi: 10.1007/s10974-014-9374-0. Epub 2014 Feb 4. J Muscle Res Cell Motil. 2014. PMID: 24493262 Free PMC article. Review.
References
-
- Haider AW, Larson MG, Benjamin EJ, Levy D. Increased left ventricular mass and hypertrophy are associated with increased risk for sudden death. J Am Coll Cardiol. 1998;32:1454–1459. - PubMed
-
- Levy D, Garrison RJ, Savage DD, Kannel WB, Castelli WP. Prognostic implications of echocardiographically determined left ventricular mass in the Framingham Heart Study. N Engl J Med. 1990;322:1561–1566. - PubMed
-
- Spirito P, Bellone P, Harris KM, Bernabo P, Bruzzi P, Maron BJ. Magnitude of left ventricular hypertrophy and risk of sudden death in hypertrophic cardiomyopathy. N Engl J Med. 2000;342:1778–1785. - PubMed
-
- Zile MR, Brutsaert DL. New concepts in diastolic dysfunction and diastolic heart failure, part II: causal mechanisms and treatment. Circulation. 2002;105:1503–1508. - PubMed
-
- Hill JA, Olson EN. Cardiac plasticity. N Engl J Med. 2008;358:1370–1380. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

