Immune responses to measles and tetanus vaccines among Kenyan human immunodeficiency virus type 1 (HIV-1)-infected children pre- and post-highly active antiretroviral therapy and revaccination
- PMID: 19258919
- PMCID: PMC2779204
- DOI: 10.1097/INF.0b013e3181903ed3
Immune responses to measles and tetanus vaccines among Kenyan human immunodeficiency virus type 1 (HIV-1)-infected children pre- and post-highly active antiretroviral therapy and revaccination
Abstract
Background: : HIV-1-infected children have lower response rates after measles and tetanus immunization than uninfected children. We determined the extent to which highly active antiretroviral therapy (HAART) augments vaccine immunity and promotes responses to revaccination.
Methods: : Previously immunized, antiretroviral-naive HIV-1-infected children were evaluated for immunity against measles and tetanus. After 6 months on HAART, children meeting CD4% criteria (>15%) who were persistently antibody negative were revaccinated and immunity was reassessed.
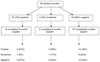
Results: : At enrollment, among 90 children with mean age of 4.9 years, 67% had negative measles IgG and 22% negative tetanus IgG. Among 62 children completing 6 months on HAART, 17 (40%) of 43 without protective measles IgG converted and 10 (53%) of 19 positive children lost measles responses (P = 0.3). Children who lost responses had significantly lower measles antibody concentrations than those who remained measles IgG positive during follow-up (7.1 vs. 20.3 mg/mL; P = 0.003). Three (23%) of 13 children negative for tetanus IgG spontaneously seroconverted on HAART, while 15 (31%) of 49 children lost tetanus antibody (P = 0.008). There was a nonsignificant trend for an association between spontaneous measles seroconversion and lower baseline HIV-1 viral load (P = 0.06). Tetanus seroconversion was associated with older age (P = 0.03). After revaccination, positive responses were observed in 78% and 75% of children reimmunized against measles and tetanus, respectively.
Conclusions: : After 6 months of HAART, more than half of previously immunized children still lacked positive measles antibody. With increased use of HAART in pediatric populations, revaccination against measles and tetanus should be considered to boost response rates and immunization coverage.
Conflict of interest statement
The authors have no associations that pose a conflict of interest.
Figures
References
-
- Taha TE, Graham SM, Kumwenda NI, et al. Morbidity among human immunodeficiency virus-1-infected and -uninfected African children. Pediatrics. 2000;106(6):E77. - PubMed
-
- Zijenah L, Mbizvo MT, Kasule J, et al. Mortality in the first 2 years among infants born to human immunodeficiency virus-infected women in Harare, Zimbabwe. J Infect Dis. 1998;178(1):109–113. - PubMed
-
- Krasinski K, Borkowsky W. Measles and measles immunity in children infected with human immunodeficiency virus. JAMA. 1989;261(17):2512–2516. - PubMed
-
- Sension MG, Quinn TC, Markowitz LE, et al. Measles in hospitalized African children with human immunodeficiency virus. Am J Dis Child. 1988;142(12):1271–1272. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Research Materials