Effects of local anesthetic concentration and dose on continuous interscalene nerve blocks: a dual-center, randomized, observer-masked, controlled study
- PMID: 19258966
- PMCID: PMC2711692
- DOI: 10.1016/j.rapm.2008.05.006
Effects of local anesthetic concentration and dose on continuous interscalene nerve blocks: a dual-center, randomized, observer-masked, controlled study
Abstract
Background and objectives: It is currently unknown if the primary determinant of continuous peripheral nerve block effects is simply total drug dose, or whether local anesthetic concentration and/or volume have an influence. We therefore tested the null hypothesis that providing ropivacaine at different concentrations and rates--but at an equal total basal dose--produces similar effects when used in a continuous interscalene nerve block.
Methods: Preoperatively, an anterolateral interscalene perineural catheter was inserted using the anterolateral approach in patients undergoing moderately painful shoulder surgery. Subjects were randomly assigned to receive a postoperative perineural infusion of either 0.2% ropivacaine (basal 8 mL/h, bolus 4 mL) or 0.4% ropivacaine (basal 4 mL/h, bolus 2 mL) through the second postoperative day. Our primary endpoint was the incidence of an insensate hand/finger during the 24 hours beginning the morning following surgery.
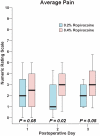
Results: The incidence of an insensate hand/finger did not differ between the treatment groups (n = 50) to a statistically significant degree (0.2% ropivacaine, mean [SD] of 0.8 [1.3] times; 0.4% ropivacaine, mean 0.3 [0.6] times; estimated difference = 0.5 episodes, 95% confidence interval, -0.1 to 1.1 episodes; P = .080). However, this is statistically inconclusive given the confidence interval. In contrast, pain (P = .020) and dissatisfaction (P = .011) were greater in patients given 0.4% ropivacaine.
Conclusions: For continuous interscalene nerve blocks, given the statistically inconclusive primary endpoint results and design limitations of the current study, further research on this topic is warranted. In contrast, providing a lower concentration of local anesthetic at a higher basal rate provided superior analgesia.
Figures

Comment in
-
Volume-concentration studies should first be performed in hospitalized patients.Reg Anesth Pain Med. 2009 Nov-Dec;34(6):605-6. doi: 10.1097/AAP.0b013e3181b4c901. Reg Anesth Pain Med. 2009. PMID: 19901772 No abstract available.
-
Re: Effects of local anesthetic concentration and dose on continuous interscalene nerve blocks: a dual-center, randomized, observer-masked, controlled study. Reply to dr. Borgeat.Reg Anesth Pain Med. 2010 Jan-Feb;35(1):120-2. doi: 10.1097/AAP.0b013e3181c97c6e. Reg Anesth Pain Med. 2010. PMID: 20048670 No abstract available.
References
-
- Rodriguez J, Taboada M, Carceller J, Lagunilla J, Barcena M, Alvarez J. Stimulating popliteal catheters for postoperative analgesia after hallux valgus repair. Anesth Analg. 2006;102:258–262. - PubMed
-
- Capdevila X, Dadure C, Bringuier S, Bernard N, Biboulet P, Gaertner E, Macaire P. Effect of patient-controlled perineural analgesia on rehabilitation and pain after ambulatory orthopedic surgery: a multicenter randomized trial. Anesthesiology. 2006;105:566–573. - PubMed
-
- Ilfeld BM, Enneking FK. Continuous peripheral nerve blocks at home: a review. Anesth Analg. 2005;100:1822–1833. - PubMed
-
- Corda DM, Enneking FK. A unique approach to postoperative analgesia for ambulatory surgery. J Clin Anesth. 2000;12:595–599. - PubMed
-
- Cohen DE, Van Duker B, Siegel S, Keon TP. Common peroneal nerve palsy associated with epidural analgesia. Anesth Analg. 1993;76:429–431. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
