Right ventricular performance in the fetus with hypoplastic left heart syndrome
- PMID: 19324154
- PMCID: PMC4436030
- DOI: 10.1016/j.athoracsur.2008.11.032
Right ventricular performance in the fetus with hypoplastic left heart syndrome
Abstract
Background: In the fetus with hypoplastic left heart syndrome (HLHS), the single right ventricle (RV) pumps the entire cardiac output in utero. By investigating RV performance in utero, we sought to determine the inherent capabilities of a single RV before the increased metabolic demands of postnatal life and surgical palliation. In addition, we sought to determine whether the presence or absence of a left ventricular cavity impacts on RV performance in fetal life.
Methods: Between November 2004 and December 2006, Doppler flow-derived measures of ventricular performance were obtained with echocardiography in 76 fetuses with normal cardiovascular system and in 48 age-matched fetuses with HLHS from 17 weeks until 40 weeks of gestation. The myocardial performance index, ventricular ejection force, and cardiac output were determined for both groups and compared using unpaired Student's t tests and regression analysis.
Results: In fetuses with HLHS, cardiac output was diminished by 20%, RV ejection force was elevated, and RV myocardial performance index was elevated compared with those of normal fetuses. The presence of a left ventricular cavity did not impact on RV performance in utero.
Conclusions: Fetuses with HLHS have preserved systolic performance but impaired diastolic performance compared with normal fetuses. The heart of a fetus with HLHS is less efficient than the normal heart in that ejection force of the RV is increased, but overall delivery of cardiac output is lower than normal. We conclude that patients with HLHS have inherent limitations in cardiac performance even before birth.
Figures
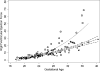
Comment in
-
Invited commentary.Ann Thorac Surg. 2009 Apr;87(4):1219. doi: 10.1016/j.athoracsur.2008.12.046. Ann Thorac Surg. 2009. PMID: 19324155 No abstract available.
Similar articles
-
Right Ventricular Systolic-to-Diastolic Time Index: Hypoplastic Left Heart Fetuses Differ Significantly from Normal Fetuses.J Am Soc Echocardiogr. 2016 Feb;29(2):143-9. doi: 10.1016/j.echo.2015.08.014. Epub 2015 Sep 26. J Am Soc Echocardiogr. 2016. PMID: 26394829
-
Perinatal Cardiac Functional Adaptation in Hypoplastic Left Heart Syndrome: A Longitudinal Analysis.J Am Soc Echocardiogr. 2024 Nov;37(11):1062-1072. doi: 10.1016/j.echo.2024.06.020. Epub 2024 Jul 10. J Am Soc Echocardiogr. 2024. PMID: 38997074
-
Evaluation of right ventricular function in fetal hypoplastic left heart syndrome using spatio-temporal image correlation (STIC).Cardiovasc Ultrasound. 2016 Apr 11;14:12. doi: 10.1186/s12947-016-0056-5. Cardiovasc Ultrasound. 2016. PMID: 27066831 Free PMC article.
-
Role of cardiac magnetic resonance strain analysis in patients with hypoplastic left heart syndrome in evaluating right ventricular (dys)function: a systematic review.Eur J Cardiothorac Surg. 2021 Sep 11;60(3):497-505. doi: 10.1093/ejcts/ezab105. Eur J Cardiothorac Surg. 2021. PMID: 34331061
-
Cardiac fibroma presenting as hypoplastic left heart syndrome in a foetus: causal or coincidental?BMJ Case Rep. 2024 Mar 21;17(3):e258742. doi: 10.1136/bcr-2023-258742. BMJ Case Rep. 2024. PMID: 38514154 Review.
Cited by
-
Prenatal Diagnosis of Fetal Heart Failure.Diagnostics (Basel). 2023 Feb 18;13(4):779. doi: 10.3390/diagnostics13040779. Diagnostics (Basel). 2023. PMID: 36832267 Free PMC article. Review.
-
New Aspects in the Diagnosis and Therapy of Fetal Hypoplastic Left Heart Syndrome.Geburtshilfe Frauenheilkd. 2019 Aug;79(8):863-872. doi: 10.1055/a-0828-7968. Epub 2019 Aug 12. Geburtshilfe Frauenheilkd. 2019. PMID: 31423021 Free PMC article.
-
Vasoreactive response to maternal hyperoxygenation in the fetus with hypoplastic left heart syndrome.Circ Cardiovasc Imaging. 2010 Mar;3(2):172-8. doi: 10.1161/CIRCIMAGING.109.848432. Epub 2009 Dec 31. Circ Cardiovasc Imaging. 2010. PMID: 20044513 Free PMC article.
-
Fetal circulatory physiology and brain development in complex congenital heart disease: A multi-modal imaging study.Prenat Diagn. 2024 Jun;44(6-7):856-864. doi: 10.1002/pd.6450. Epub 2023 Oct 10. Prenat Diagn. 2024. PMID: 37817395 Free PMC article.
-
Characterization of the Placenta in the Newborn with Congenital Heart Disease: Distinctions Based on Type of Cardiac Malformation.Pediatr Cardiol. 2018 Aug;39(6):1165-1171. doi: 10.1007/s00246-018-1876-x. Epub 2018 May 4. Pediatr Cardiol. 2018. PMID: 29728721 Free PMC article.
References
-
- Hirsch JC, Ohye RG, Devaney EJ, Goldberg CS, Bove EL. The lateral tunnel fontan procedure for hypoplastic left heart syndrome: results of 100 consecutive patients. Pediatr Cardiol. 2007;28:426–32. - PubMed
-
- Mitchell ME, Ittenbach RF, Gaynor JW, et al. Intermediate outcomes after the Fontan procedure in the current era. J Thorac Cardiovasc Surg. 2006;131:172–80. - PubMed
-
- Kaltman JR, Di H, Tian Z, Rychik J. Impact of congenital heart disease on cerebrovascular blood flow dynamics in the fetus. Ultrasound Obstet Gynecol. 2005;25:32–6. - PubMed
-
- Miller SP, McQuillen PS, Hamrick S, et al. Abnormal brain development in newborns with congenital heart disease. N Engl J Med. 2007;357:1928–38. - PubMed
-
- Donofrio MT, Bremer YA, Schieken RM, et al. Autoregulation of cerebral blood flow in fetuses with congenital heart disease: the brain sparing effect. Pediatr Cardiol. 2003;24:436–43. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

