Survival benefit-based deceased-donor liver allocation
- PMID: 19341419
- PMCID: PMC2895923
- DOI: 10.1111/j.1600-6143.2009.02571.x
Survival benefit-based deceased-donor liver allocation
Abstract
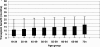
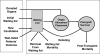
Currently, patients awaiting deceased-donor liver transplantation are prioritized by medical urgency. Specifically, wait-listed chronic liver failure patients are sequenced in decreasing order of Model for End-stage Liver Disease (MELD) score. To maximize lifetime gained through liver transplantation, posttransplant survival should be considered in prioritizing liver waiting list candidates. We evaluate a survival benefit based system for allocating deceased-donor livers to chronic liver failure patients. Under the proposed system, at the time of offer, the transplant survival benefit score would be computed for each patient active on the waiting list. The proposed score is based on the difference in 5-year mean lifetime (with vs. without a liver transplant) and accounts for patient and donor characteristics. The rank correlation between benefit score and MELD score is 0.67. There is great overlap in the distribution of benefit scores across MELD categories, since waiting list mortality is significantly affected by several factors. Simulation results indicate that over 2000 life-years would be saved per year if benefit-based allocation was implemented. The shortage of donor livers increases the need to maximize the life-saving capacity of procured livers. Allocation of deceased-donor livers to chronic liver failure patients would be improved by prioritizing patients by transplant survival benefit.
Figures
References
-
- Merion RM, Schaubel DE, Dykstra DM, Freeman RB, Port FK, Wolfe RA. The survival benefit of liver transplantation. Am J Transplant. 2005;5:307–313. - PubMed
-
- Miles CD, Schaubel DE, Jia X, Ojo AO, Port FK, Rao PS. Mortality experience in recipients undergoing repeat transplantation with expanded criteria donor and non-ECD deceased-donor kidneys. Am J Transplant. 2007;7:1140–1147. - PubMed
-
- Wolfe RA, Ashby VB, Milford EL, et al. Comparison of mortality in all patients on dialysis, patients on dialysis awaiting transplantation, and recipients of a first cadaveric transplant. N Eng J Med. 1999;341:1725–1730. - PubMed
-
- Malinchoc M, Kamath PS, Gordon FD, Peine CJ, Rank J, ter Borg PC. A model to predict poor survival in patients undergoing transjugular intrahepatic portosystemic shunts. Hepatology. 2000;31:864–871. - PubMed
-
- Kamath PS, Wiesner RH, Malinchoc M, et al. A model to predict survival in patients with end-stage liver disease. Hepatology. 2001;33:464–470. - PubMed