Kallikreins and lupus nephritis
- PMID: 19348047
- PMCID: PMC2662572
- DOI: 10.1172/jci38786
Kallikreins and lupus nephritis
Abstract
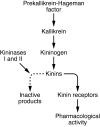
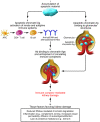
The kidney kallikrein-kinin system plays important roles in inflammation, coagulation, angiogenesis, and regulation of vessel tone and permeability. In this issue of the JCI, Liu et al. provide data that suggest a protective role for kallikrein in animal models of anti-glomerular basement membrane(GBM) antibody-induced nephritis, an experimental model of Goodpasture disease (see the related article beginning on page 911). Furthermore, human systemic lupus erythematosus and lupus nephritis were shown to be associated with kallikrein 1 (KLK1) and the KLK3 promoter. The authors suggest that kallikrein genes are involved in the development of SLE and lupus nephritis and may exert a renoprotective role. It is possible, however, that the kallikrein-kinin system may play dual roles: protecting the kidney against ischemia and interstitial fibrosis while also mediating vasodilation, inflammation, and activation of the innate immune response.
Figures
Comment on
-
Kallikrein genes are associated with lupus and glomerular basement membrane-specific antibody-induced nephritis in mice and humans.J Clin Invest. 2009 Apr;119(4):911-23. doi: 10.1172/JCI36728. J Clin Invest. 2009. PMID: 19307730 Free PMC article.
References
-
- Margolius H.S., Horwitz D., Pisano J.J., Keiser H.R. Urinary kallikrein excretion in hypertensive man. Relationship to sodium intake and sodium-retaining steroids. Circ. Res. 1974;35:820–825. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Miscellaneous

