Integration of skeletal muscle resistance arteriolar reactivity for perfusion responses in the metabolic syndrome
- PMID: 19386988
- PMCID: PMC2692785
- DOI: 10.1152/ajpregu.00096.2009
Integration of skeletal muscle resistance arteriolar reactivity for perfusion responses in the metabolic syndrome
Abstract
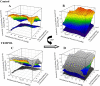
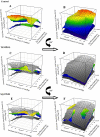
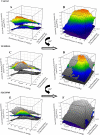
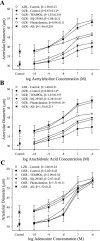
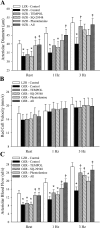
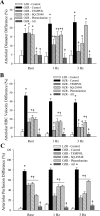
Previous study suggests that with evolution of the metabolic syndrome, patterns of arteriolar reactivity are profoundly altered and may constrain functional hyperemia. This study investigated interactions between parameters of vascular reactivity at two levels of resistance arterioles in obese Zucker rats (OZR), translating these observations into perfusion regulation for in situ skeletal muscle. Dilation of isolated and in situ resistance arterioles from OZR to acetylcholine, arachidonic acid (AA), and hypoxia (isolated arterioles only) were blunted vs. lean Zucker rats (LZR), although dilation to adenosine was intact. Increased adrenergic tone (phenylephrine) or intralumenal pressure (ILP) impaired dilation in both strains (OZR>LZR). Treatment of OZR arterioles with Tempol (superoxide dismutase mimetic) or SQ-29548 (prostaglandin H2/thromboxane A2 receptor antagonist) improved dilator reactivity under control conditions and with increased ILP, but had minimal effect with increased adrenergic tone. Arteriolar dilation to adenosine was well maintained in both strains under all conditions. For in situ cremasteric arterioles, muscle contraction-induced elevations in metabolic demand elicited arteriolar dilations and hyperemic responses that were blunted in OZR vs. LZR, although distal parallel arterioles were characterized by heterogeneous dilator and perfusion responses. alpha-Adrenoreceptor blockade improved outcomes at rest but had minimal effect with elevated metabolic demand. Treatment with Tempol or SQ-29548 had minimal impact at rest, but lessened distal arteriolar perfusion heterogeneity with increased metabolic demand. In blood-perfused gastrocnemius of OZR, perfusion was constrained primarily by adrenergic tone, while myogenic activation and endothelium-dependent dilation did not appear to contribute significantly to ischemia. These results of this novel, integrated approach suggest that adrenergic tone and metabolic dilation are robust determinants of bulk perfusion to skeletal muscle of OZR, while endothelial dysfunction may more strongly regulate perfusion distribution homogeneity via the impact of oxidant stress and AA metabolism.
Figures
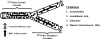
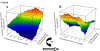
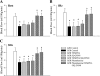
References
-
- Baker M, Wayland H. On-line volume-flow rates and velocity profile measurements for blood in microvessels. Microvasc Res 7: 131–143, 1974. - PubMed
-
- Baumbach GL, Hajdu MA. Mechanics and composition of cerebral arterioles in renal and spontaneously hypertensive rats. Hypertension 21: 816–826, 1993. - PubMed
-
- Bohlen HG Protein kinase beta II in Zucker obese rats compromises oxygen and flow-mediated regulation of nitric oxide formation. Am J Physiol Heart Circ Physiol 286: H492–H497, 2004. - PubMed
-
- Cannon CP Cardiovascular disease and modifiable cardiometabolic risk factors. Clin Cornerstone 8: 11–28, 2007. - PubMed
-
- Chen D, Wang MW. Development and application of rodent models for type 2 diabetes. Diabetes Obes Metab 7: 307–317, 2005. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

