Prospective evaluation of chronic pain associated with posterior autologous iliac crest bone graft harvest and its effect on postoperative outcome
- PMID: 19480692
- PMCID: PMC2693524
- DOI: 10.1186/1477-7525-7-49
Prospective evaluation of chronic pain associated with posterior autologous iliac crest bone graft harvest and its effect on postoperative outcome
Abstract
Background: Autogenous Iliac Crest Bone Graft (ICBG) has been the "gold standard" for spinal fusion. However, bone graft harvest may lead to complications, such as chronic pain, numbness, and poor cosmesis. The long-term impact of these complications on patient function and well-being has not been established but is critical in determining the value of expensive bone graft substitutes such as recombinant bone morphogenic protein. We thus aimed to investigate the long-term complications of ICBG. Our second aim was to evaluate the psychometric properties of a new measure of ICBG morbidity that would be useful for appropriately gauging spinal surgery outcomes.
Methods: Prospective study of patients undergoing spinal fusion surgery with autologous ICBG. The SF-36v2, Oswestry Disability Index, and a new 14-item follow-up questionnaire addressing persistent pain, functional limitation, and cosmesis were administered with an 83% response rate. Multiple regression analyses examined the independent effect of ICBG complications on physical and mental health and disability.
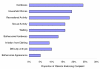
Results: The study population included 170 patients with a mean age of 51.1 years (SD = 12.2) and balanced gender (48% male). Lumbar fusion patients predominated (lumbar = 148; cervical n = 22). At 3.5 years mean follow-up, 5% of patients reported being bothered by harvest site scar appearance, 24% reported harvest site numbness, and 13% reported the numbness as bothersome. Harvest site pain resulted in difficulty with household chores (19%), recreational activity (18%), walking (16%), sexual activity (16%), work activity (10%), and irritation from clothing (9%). Multivariate regression analyses revealed that persistent ICBG complications 3.5 years post-surgery were associated with significantly worse disability and showed a trend association with worse physical health, after adjusting for age, workers' compensation status, surgical site pain, and arm or leg pain. There was no association between ICBG complications and mental health in the multivariate model.
Conclusion: Chronic ICBG harvest site pain and discomfort is reported by a significant percentage of patients undergoing this procedure more than three years following surgery, and these complications are associated with worse patient-reported disability. Future studies should consider employing a control group that does not include autologous bone graft harvest, e.g., a group utilizing rhBMP, to determine whether eliminating harvest-site morbidity does indeed lead to observable improvement in clinical outcome sufficient to justify the increased cost of bone graft substitutes.
Figures
References
-
- Ahlmann E, Patzakis M, Roidis N, Shepherd L, Holtom P. Comparison of anterior and posterior iliac crest bone grafts in terms of harvest-site morbidity and functional outcomes. J Bone Joint Surg Am. 2002;84-A:716–720. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

