Left ventricular remodeling after myocardial infarction: characterization of a swine model on beta-blocker therapy
- PMID: 19619418
- PMCID: PMC2733287
Left ventricular remodeling after myocardial infarction: characterization of a swine model on beta-blocker therapy
Abstract
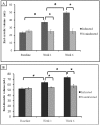
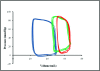
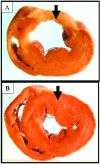
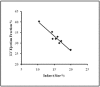
Current guidelines recommend beta blockers for patients after myocardial infarction (MI). Novel therapies for heart failure should be tested in combination with this medication before entering clinical trials. In this methodologic study, we sought to describe the time course of systolic and diastolic parameters of cardiac performance over a 6-wk period in closed-chest model of swine MI treated with a beta blocker. Myocardial infarction in pigs (n = 10) was induced by 90-min balloon occlusion of the left anterior descending coronary artery. Echocardiography and pressure-volume data were collected before and at 1 and 6 wk after MI; histopathology was assessed at 6 wk. Left-ventricular (LV) volume increased significantly over 6 wk, with significant decreases in ejection fraction, wall motion index, stroke work, rate of pressure development (dP/dt(max)), preload recruitable stroke work, and mechanical efficiency. Impairment of diastolic function was manifested by a significant increase in the exponential beta coefficient of the LV end-diastolic pressure-volume relation and reduction of LV pressure decay. At 6 wk, histopathologic analysis showed that the size of the infarct area was 16.3% +/- 4.4%, and the LV mass and myocyte cross-sectional area in both the infarct border and remote zones were increased compared with those of noninfarcted pigs (n = 5). These findings suggest a dynamic pattern of remodeling over time in a closed-chest ischemia-reperfusion swine model of acute MI on beta-blocker therapy and may guide future studies.
Figures
Similar articles
-
Regional left ventricular wall stress postmyocardial infarction with magnetic resonance imaging in swine.Am J Physiol Heart Circ Physiol. 2025 Jun 1;328(6):H1391-H1399. doi: 10.1152/ajpheart.00120.2025. Epub 2025 May 7. Am J Physiol Heart Circ Physiol. 2025. PMID: 40331882
-
Endothelial nitric oxide synthase limits left ventricular remodeling after myocardial infarction in mice.Circulation. 2001 Sep 11;104(11):1286-91. doi: 10.1161/hc3601.094298. Circulation. 2001. PMID: 11551881
-
Pioglitazone, a peroxisome proliferator-activated receptor-gamma agonist, attenuates left ventricular remodeling and failure after experimental myocardial infarction.Circulation. 2002 Dec 10;106(24):3126-32. doi: 10.1161/01.cir.0000039346.31538.2c. Circulation. 2002. PMID: 12473562
-
Clinical aspects of left ventricular diastolic function assessed by Doppler echocardiography following acute myocardial infarction.Dan Med Bull. 2001 Nov;48(4):199-210. Dan Med Bull. 2001. PMID: 11767125 Review.
-
Searching for Preclinical Models of Acute Decompensated Heart Failure: a Concise Narrative Overview and a Novel Swine Model.Cardiovasc Drugs Ther. 2022 Aug;36(4):727-738. doi: 10.1007/s10557-020-07096-5. Epub 2020 Oct 24. Cardiovasc Drugs Ther. 2022. PMID: 33098053 Free PMC article. Review.
Cited by
-
In vivo magnetic resonance elastography to estimate left ventricular stiffness in a myocardial infarction induced porcine model.J Magn Reson Imaging. 2017 Apr;45(4):1024-1033. doi: 10.1002/jmri.25432. Epub 2016 Aug 17. J Magn Reson Imaging. 2017. PMID: 27533317 Free PMC article.
-
Modeling Electrophysiological Coupling and Fusion between Human Mesenchymal Stem Cells and Cardiomyocytes.PLoS Comput Biol. 2016 Jul 25;12(7):e1005014. doi: 10.1371/journal.pcbi.1005014. eCollection 2016 Jul. PLoS Comput Biol. 2016. PMID: 27454812 Free PMC article.
-
Cardioprotective effect of silicon-built restraint device (ASD), for left ventricular remodeling in rat heart failure model.J Mater Sci Mater Med. 2022 May 10;33(5):42. doi: 10.1007/s10856-022-06663-6. J Mater Sci Mater Med. 2022. PMID: 35536369 Free PMC article.
-
Development of a closed chest model of chronic myocardial infarction in Swine: magnetic resonance imaging and pathological evaluation.ISRN Cardiol. 2013 Oct 27;2013:781762. doi: 10.1155/2013/781762. eCollection 2013. ISRN Cardiol. 2013. PMID: 24282645 Free PMC article.
-
Cytokine combination therapy with erythropoietin and granulocyte colony stimulating factor in a porcine model of acute myocardial infarction.Cardiovasc Drugs Ther. 2010 Dec;24(5-6):409-20. doi: 10.1007/s10557-010-6263-7. Cardiovasc Drugs Ther. 2010. PMID: 20809214 Free PMC article.
References
-
- Amado LC, Saliaris AP, Schuleri KH, St John M, Xie JS, Cattaneo S, Durand DJ, Fitton T, Kuang JQ, Stewart G, Lehrke S, Baumgartner WW, Martin BJ, Heldman AW, Hare JM. 2005. Cardiac repair with intramyocardial injection of allogeneic mesenchymal stem cells after myocardial infarction. Proc Natl Acad Sci USA 102:11474–11479 - PMC - PubMed
-
- Antman EM, Hand M, Armstrong PW, Bates ER, Green LA, Halasyamani LK, Hochman JS, Krumholz HM, Lamas GA, Mullany CJ, Pearle DL, Sloan MA, Smith SC, Jr, Anbe DT, Kushner FG, Ornato JP, Jacobs AK, Adams CD, Anderson JL, Buller CE, Creager MA, Ettinger SM, Halperin JL, Hunt SA, Lytle BW, Nishimura R, Page RL, Riegel B, Tarkington LG, Yancy CW. 2008. 2007 focused update of the ACC/AHA 2004 guidelines for the management of patients with ST-elevation myocardial infarction: a report of the American College of Cardiology/American Heart Association Task Force on practice guidelines: developed in collaboration with the Canadian Cardiovascular Society endorsed by the American Academy of Family Physicians: 2007 Writing Group to review new evidence and update the ACC/AHA 2004 guidelines for the management of patients with ST-elevation myocardial infarction, writing on behalf of the 2004 Writing Committee. Circulation 117:296–329 - PubMed
-
- Blom AS, Pilla JJ, Gorman RC, 3rd, Gorman JH, Mukherjee R, Spinale FG, Acker MA. 2005. Infarct size reduction and attenuation of global left ventricular remodeling with the CorCap cardiac support device following acute myocardial infarction in sheep. Heart Fail Rev 10:125–139 - PubMed
-
- Borlaug BA, Kass DA. 2006. Mechanisms of diastolic dysfunction in heart failure. Trends Cardiovasc Med 16:273–279 - PubMed
-
- Burkhoff D, Mirsky I, Suga H. 2005. Assessment of systolic and diastolic ventricular properties via pressure-volume analysis: a guide for clinical, translational, and basic researchers. Am J Physiol Heart Circ Physiol 289:H501–H512 - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
