Effects of the SOD mimic nitroxide 3-carbamoyl-PROXYL on oxidative stress markers and endothelial dysfunction in streptozotocin-induced diabetic rats
- PMID: 19649229
- PMCID: PMC2719166
Effects of the SOD mimic nitroxide 3-carbamoyl-PROXYL on oxidative stress markers and endothelial dysfunction in streptozotocin-induced diabetic rats
Abstract
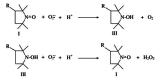
Objective: To evaluate the effects of 3-carbamoyl-PROXYL (CP), a stable superoxide dismutase (SOD) mimic compound, on oxidative stress markers and endothelial dysfunction in diabetic rats.
Animals and methods: Rats were made diabetic by a single vein injection of streptozotocin (65 mg/kg) and diabetes was verified by the existence of excessive hyperglycemia a week after the treatment. Control and diabetic rats received vehicle or drug for eight weeks, after which the vascular tissue was examined for relaxation and oxidative stress markers.
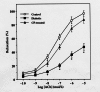
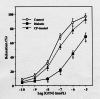
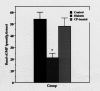
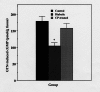
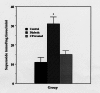
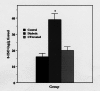
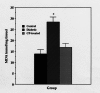
Results: Diabetic rats showed increased vascular levels of superoxide that were accompanied by increased tissue levels of the oxidative stress markers malondialdehyde (MDA) and 8-iso-prostaglandin F2alpha (8-ISO). The vasorelaxant as well as the cyclic guanosine 5'-monophosphate (cGMP)-producing effects of acetylcholine (ACh) and nitroglycerine were reduced in diabetic rats. Treatment of diabetic rats with CP (50 mg/kg intraperitoneally, bid) abolished not only the differences in superoxide, MDA and 8-ISO levels, but also the differences in the relaxation and cGMP responses of vascular tissue between control and diabetic rats to both ACh and nitroglycerine.
Conclusions: These results support the involvement of reactive oxygen species in mediation of diabetes-induced endothelial dysfunction in vivo, and provide the rationale for the potential use of SOD mimics in the treatment of diabetes.
Keywords: Endothelial dysfunction; Isoprostanes; Lipid peroxidation; Nitric oxide; Relaxation; Superoxide; cGMP.
Figures

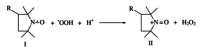


Similar articles
-
Effects of the superoxide dismutase-mimetic compound tempol on endothelial dysfunction in streptozotocin-induced diabetic rats.Eur J Pharmacol. 2002 Feb 1;436(1-2):111-8. doi: 10.1016/s0014-2999(01)01566-7. Eur J Pharmacol. 2002. PMID: 11834254
-
Oxidative stress measurement by in vivo electron spin resonance spectroscopy in rats with streptozotocin-induced diabetes.Diabetologia. 1998 Nov;41(11):1355-60. doi: 10.1007/s001250051076. Diabetologia. 1998. PMID: 9833944
-
Effects of the superoxide dismutase-mimic compound TEMPOL on oxidant stress-mediated endothelial dysfunction.Antioxid Redox Signal. 1999 Summer;1(2):221-32. doi: 10.1089/ars.1999.1.2-221. Antioxid Redox Signal. 1999. PMID: 11228749
-
Molecular Mechanism of Fucoidan Nanoparticles as Protector on Endothelial Cell Dysfunction in Diabetic Rats' Aortas.Nutrients. 2023 Jan 21;15(3):568. doi: 10.3390/nu15030568. Nutrients. 2023. PMID: 36771275 Free PMC article.
-
Chronic administration of daidzein, a soybean isoflavone, improves endothelial dysfunction and attenuates oxidative stress in streptozotocin-induced diabetic rats.Phytother Res. 2013 Jan;27(1):112-7. doi: 10.1002/ptr.4699. Epub 2012 Apr 17. Phytother Res. 2013. PMID: 22511255
Cited by
-
Development of a novel molecular probe for the detection of liver mitochondrial redox metabolism.Sci Rep. 2020 Oct 5;10(1):16489. doi: 10.1038/s41598-020-73336-1. Sci Rep. 2020. PMID: 33020535 Free PMC article.
References
-
- Giugliano D, Ceriello A, Paolisso G. Diabetes mellitus, hypertension, and cardiovascular disease: Which role for oxidative stress? Metabolism. 1995;44:363–8. - PubMed
-
- Cannon RO., III Role of nitric oxide in cardiovascular disease: focus on the endothelium. Clin Chem. 1988;44:1809–19. - PubMed
-
- Oyama Y, Kawasaki H, Hattori Y, Kanno M. Attenuation of endothelium-dependent relaxation in aorta from diabetic rats. Eur J Pharmacol. 1986;131:75–8. - PubMed
-
- Pieper GM, Gross GJ. Oxygen free radicals abolish endothelium-dependent relaxation in diabetic aorta. Am J Physiol. 1988;255:H825–33. - PubMed
-
- Diederich D, Skopec J, Diederich A, Dai FX. Endothelial dysfunction in mesenteric resistance arteries of diabetic rat: role of free radicals. Am J Physiol. 1994;266:H1153–61. - PubMed
LinkOut - more resources
Full Text Sources
Miscellaneous
