Primary intraocular lymphoma
- PMID: 19653715
- PMCID: PMC2732907
- DOI: 10.5858/133.8.1228
Primary intraocular lymphoma
Abstract
Primary intraocular lymphoma, recently suggested to be renamed primary retinal lymphoma, is a subset of primary central nervous system lymphoma and is usually an aggressive diffuse large B-cell lymphoma. Between 56% and 85% of patients who initially present with primary intraocular lymphoma alone will develop cerebral lesions. Patients typically complain of decreased vision and floaters, most likely secondary to the chronic vitritis and subretinal lesions. The diagnosis of primary intraocular lymphoma can be difficult to make and requires tissue for diagnosis. The atypical lymphoid cells are large and display a high nuclear to cytoplasmic ratio, prominent nucleoli, and basophilic cytoplasm. Flow cytometry, immunohistochemistry, cytokine analysis, and gene rearrangements also aid in the diagnosis. Local and systemic treatments, such as chemotherapy and radiation, are employed, although the relapse rate remains high.
Figures


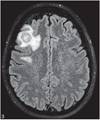

References
-
- Chan CC, Gonzalez JA. Primary Intraocular Lymphoma. Hackensack, NJ: World Scientific Publishing Co Pte Ltd; 2007.
-
- Coupland SE, Damato B. Understanding intraocular lymphoma. Clin Experiment Ophthalmol. 2008;36(6):564–578. - PubMed
-
- Hoffman PM, McKelvie P, Hall AJ, et al. Intraocular lymphoma: a series of 14 patients with clinicopathological features and treatment outcomes. Eye. 2003;17:513–521. - PubMed
-
- Grimm SA, Pulido JS, Jahnke K, et al. Primary intraocular lymphoma: an international primary central nervous system lymphoma collaborative group report. Ann Oncol. 2007;18(11):1851–1855. - PubMed
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

