Intensity-modulated proton therapy reduces the dose to normal tissue compared with intensity-modulated radiation therapy or passive scattering proton therapy and enables individualized radical radiotherapy for extensive stage IIIB non-small-cell lung cancer: a virtual clinical study
- PMID: 19660879
- PMCID: PMC2868090
- DOI: 10.1016/j.ijrobp.2009.04.028
Intensity-modulated proton therapy reduces the dose to normal tissue compared with intensity-modulated radiation therapy or passive scattering proton therapy and enables individualized radical radiotherapy for extensive stage IIIB non-small-cell lung cancer: a virtual clinical study
Abstract
Purpose: To compare dose volume histograms of intensity-modulated proton therapy (IMPT) with those of intensity-modulated radiation therapy (IMRT) and passive scattering proton therapy (PSPT) for the treatment of stage IIIB non-small-cell lung cancer (NSCLC) and to explore the possibility of individualized radical radiotherapy.
Methods and materials: Dose volume histograms designed to deliver IMRT at 60 to 63 Gy, PSPT at 74 Gy, and IMPT at the same doses were compared and the use of individualized radical radiotherapy was assessed in patients with extensive stage IIIB NSCLC (n = 10 patients for each approach). These patients were selected based on their extensive disease and were considered to have no or borderline tolerance to IMRT at 60 to 63 Gy, based on the dose to normal tissue volume constraints (lung volume receiving 20 Gy [V20] of <35%, total mean lung dose <20 Gy; spinal cord dose, <45 Gy). The possibility of increasing the total tumor dose with IMPT for each patient without exceeding the dose volume constraints (maximum tolerated dose [MTD]) was also investigated.
Results: Compared with IMRT, IMPT spared more lung, heart, spinal cord, and esophagus, even with dose escalation from 63 Gy to 83.5 Gy, with a mean MTD of 74 Gy. Compared with PSPT, IMPT allowed further dose escalation from 74 Gy to a mean MTD of 84.4 Gy (range, 79.4-88.4 Gy) while all parameters of normal tissue sparing were kept at lower or similar levels. In addition, IMPT prevented lower-dose target coverage in patients with complicated tumor anatomies.
Conclusions: IMPT reduces the dose to normal tissue and allows individualized radical radiotherapy for extensive stage IIIB NSCLC.
Copyright 2010 Elsevier Inc. All rights reserved.
Conflict of interest statement
Figures
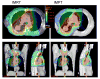

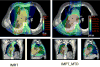

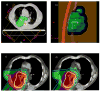
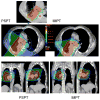


References
-
- Curran W, Scott C, Langer C, et al. Long term benefit is observed in a phase III comparison of sequential vs concurrent chemo-radiation for patients with unresectable NSCLC: RTOG 9410. Proc Am Soc Clin Oncol. 2003:621a.
-
- Kong F, Ten Haken R, Schipper M, et al. High-dose radiation improved local tumor control and overall survival in patients with inoperable/unresectable non-small-cell lung cancer: Long-term results of a radiation dose escalation study. Int J Radiat Oncol Biol Phys. 2005;63:324–333. - PubMed
-
- Murshed H, Liu H, Liao Z, et al. Dose and volume reduction for normal lung using intensity-modulated radiotherapy for advanced-stage non-small-cell lung cancer. Int J Radiat Oncol Biol Phys. 2004;58:1258–1267. - PubMed
-
- Yom S, Liao Z, Liu H, et al. Initial evaluation of treatment-related pneumonitis in advanced- stage non-small-cell lung cancer patients treated with concurrent chemotherapy and intensity-modulated radiotherapy. Int J Radiat Oncol Biol Phys. 2007;68:94–102. - PubMed
-
- Bush DA, Slater JD, Shin BB, Cheek G, Miller DW, Slater JM. Hypofractionated proton beam radiotherapy for stage I lung cancer. Chest. 2004;126(4):1198–1203. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

