Minimal hepatic encephalopathy is associated with motor vehicle crashes: the reality beyond the driving test
- PMID: 19670416
- PMCID: PMC2757520
- DOI: 10.1002/hep.23128
Minimal hepatic encephalopathy is associated with motor vehicle crashes: the reality beyond the driving test
Abstract
Patients with minimal hepatic encephalopathy (MHE) have impaired driving skills, but association of MHE with motor vehicle crashes is unclear. Standard psychometric tests (SPT) or inhibitory control test (ICT) can be used to diagnose MHE. The aim was to determine the association of MHE with crashes and traffic violations over the preceding year and on 1-year follow-up. Patients with cirrhosis were diagnosed with MHE by ICT (MHEICT) and SPT (MHESPT). Self and department-of-transportation (DOT)-reports were used to determine crashes and violations over the preceding year. Agreement between self and DOT-reports was analyzed. Patients then underwent 1-year follow-up for crash/violation occurrence. Crashes in those with/without MHEICT and MHESPT were compared. 167 patients with cirrhosis had DOT-reports, of which 120 also had self-reports. A significantly higher proportion of MHEICT patients with cirrhosis experienced crashes in the preceding year compared to those without MHE by self-report (17% vs 0.0%, P = 0.0004) and DOT-reports (17% vs 3%, P = 0.004, relative risk: 5.77). SPT did not differentiate between those with/without crashes. A significantly higher proportion of patients with crashes had MHEICT compared to MHESPT, both self-reported (100% vs 50%, P = 0.03) and DOT-reported (89% vs 44%, P = 0.01). There was excellent agreement between self and DOT-reports for crashes and violations (Kappa 0.90 and 0.80). 109 patients were followed prospectively. MHEICT patients had a significantly higher future crashes/violations compared to those without (22% vs 7%, P = 0.03) but MHESPT did not. MHEICT (Odds ratio: 4.51) and prior year crash/violation (Odds ratio: 2.96) were significantly associated with future crash/violation occurrence.
Conclusion: Patients with cirrhosis and MHEICT have a significantly higher crash rate over the preceding year and on prospective follow-up compared to patients without MHE. ICT, but not SPT performance is significantly associated with prior and future crashes and violations. There was an excellent agreement between self- and DOT-reports.
Figures
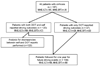
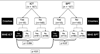



Comment in
-
Minimal hepatic encephalopathy and driving.Hepatology. 2009 Oct;50(4):1007-8. doi: 10.1002/hep.23269. Hepatology. 2009. PMID: 19787810 No abstract available.
References
-
- Hartmann IJ, Groeneweg M, Quero JC, Beijeman SJ, de Man RA, Hop WC, Schalm SW. The prognostic significance of subclinical hepatic encephalopathy. Am J Gastroenterol. 2000;95:2029–2034. - PubMed
-
- Romero-Gomez M, Boza F, Garcia-Valdecasas MS, Garcia E, Aguilar-Reina J. Subclinical hepatic encephalopathy predicts the development of overt hepatic encephalopathy. Am J Gastroenterol. 2001;96:2718–2723. - PubMed
-
- Groeneweg M, Quero JC, De Bruijn I, Hartmann IJ, Essink-bot ML, Hop WC, Schalm SW. Subclinical hepatic encephalopathy impairs daily functioning. Hepatology. 1998;28:45–49. - PubMed
-
- Ortiz M, Jacas C, Cordoba J. Minimal hepatic encephalopathy: diagnosis, clinical significance and recommendations. J Hepatol. 2005;42 Suppl:S45–S53. - PubMed
-
- Ferenci P, Lockwood A, Mullen K, Tarter R, Weissenborn K, Blei AT. Hepatic encephalopathy--definition, nomenclature, diagnosis, and quantification: final report of the working party at the 11th World Congresses of Gastroenterology, Vienna, 1998. Hepatology. 2002;35:716–721. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
