Secondary hepatic resection as a therapeutic goal in advanced colorectal cancer
- PMID: 19701965
- PMCID: PMC2731247
- DOI: 10.3748/wjg.15.3855
Secondary hepatic resection as a therapeutic goal in advanced colorectal cancer
Abstract
Surgery is the only curative option for patients with liver metastases of colorectal cancer, but few patients present with resectable hepatic lesions. Chemotherapy is increasingly used to downstage initially unresectable disease and allow for potentially curative surgery. Standard chemotherapy regimens convert 10%-20% of cases to resectable disease in unselected populations and 30%-40% of those with disease confined to the liver. One strategy to further increase the number of candidates eligible for surgery is the addition of active targeted agents such as cetuximab and bevacizumab to standard chemotherapy. Data from a phase III trial indicate that cetuximab increases the number of patients eligible for secondary hepatic resection, as well as the rate of complete resection when combined with first-line treatment with the FOLFIRI regimen. The safety profiles of preoperative cetuximab or bevacizumab have not been thoroughly assessed, but preliminary evidence indicates that these agents do not increase surgical mortality or exacerbate chemotherapy-related hepatotoxicity, such as steatosis (5-fluorouracil), steatohepatitis (irinotecan), and sinusoidal obstruction (oxaliplatin). Secondary resection is a valid treatment goal for certain patients with initially unresectable liver metastases and an important end point for future clinical trials.
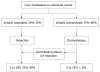
Figures
Similar articles
-
Tumour response and secondary resectability of colorectal liver metastases following neoadjuvant chemotherapy with cetuximab: the CELIM randomised phase 2 trial.Lancet Oncol. 2010 Jan;11(1):38-47. doi: 10.1016/S1470-2045(09)70330-4. Epub 2009 Nov 26. Lancet Oncol. 2010. PMID: 19942479 Clinical Trial.
-
Cost-effectiveness of targeted therapy with cetuximab in patients with K-ras wild-type colorectal cancer presenting with initially unresectable metastases limited to the liver in a German setting.Clin Ther. 2011 Apr;33(4):482-97. doi: 10.1016/j.clinthera.2011.04.010. Clin Ther. 2011. PMID: 21635994
-
Chemotherapy of metastatic colorectal cancer.Prescrire Int. 2010 Oct;19(109):219-24. Prescrire Int. 2010. PMID: 21180382 Review.
-
[Recent results of irinotecan therapy in colorectal cancer].Magy Onkol. 2004;48(4):281-8. Epub 2005 Jan 17. Magy Onkol. 2004. PMID: 15655572 Review. Hungarian.
-
Is resection of colorectal liver metastases after a second-line chemotherapy regimen justified?Cancer. 2011 Oct 1;117(19):4484-92. doi: 10.1002/cncr.26036. Epub 2011 Mar 28. Cancer. 2011. PMID: 21446046 Free PMC article.
Cited by
-
Neoadjuvant and conversion treatment of patients with colorectal liver metastasis: the potential role of bevacizumab and other antiangiogenic agents.Target Oncol. 2015 Dec;10(4):453-65. doi: 10.1007/s11523-015-0362-0. Epub 2015 Mar 11. Target Oncol. 2015. PMID: 25752908 Free PMC article. Review.
-
Consensus report from the 7th International Forum for Liver Magnetic Resonance Imaging.Eur Radiol. 2016 Mar;26(3):674-82. doi: 10.1007/s00330-015-3873-2. Epub 2015 Jun 13. Eur Radiol. 2016. PMID: 26070500 Free PMC article.
-
Integrating molecular diagnostics into anticancer drug discovery.Nat Rev Drug Discov. 2010 Jul;9(7):523-35. doi: 10.1038/nrd3135. Epub 2010 Jun 7. Nat Rev Drug Discov. 2010. PMID: 20531274
-
Perioperative complications after neoadjuvant chemotherapy with and without bevacizumab for colorectal liver metastases.J Gastrointest Surg. 2013 Mar;17(3):527-32. doi: 10.1007/s11605-012-2108-y. Epub 2013 Jan 9. J Gastrointest Surg. 2013. PMID: 23299220
References
-
- Nordlinger B, Sorbye H, Glimelius B, Poston GJ, Schlag PM, Rougier P, Bechstein WO, Primrose JN, Walpole ET, Finch-Jones M, et al. Perioperative chemotherapy with FOLFOX4 and surgery versus surgery alone for resectable liver metastases from colorectal cancer (EORTC Intergroup trial 40 983): a randomised controlled trial. Lancet. 2008;371:1007–1016. - PMC - PubMed
-
- Weiss L, Grundmann E, Torhorst J, Hartveit F, Moberg I, Eder M, Fenoglio-Preiser CM, Napier J, Horne CH, Lopez MJ. Haematogenous metastatic patterns in colonic carcinoma: an analysis of 1541 necropsies. J Pathol. 1986;150:195–203. - PubMed
-
- National Comprehensive Cancer Network. Colon cancer practice guidelines in oncology. Version 2. 2008. Available from: URL: http://www.nccn.org.
-
- Borner MM. Neoadjuvant chemotherapy for unresectable liver metastases of colorectal cancer--too good to be true? Ann Oncol. 1999;10:623–626. - PubMed
Publication types
MeSH terms
Substances
Supplementary concepts
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical