Arginase inhibition in airways from normal and nitric oxide synthase 2-knockout mice exposed to ovalbumin
- PMID: 19800904
- PMCID: PMC3221650
- DOI: 10.1016/j.taap.2009.09.018
Arginase inhibition in airways from normal and nitric oxide synthase 2-knockout mice exposed to ovalbumin
Abstract
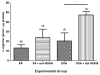
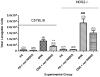
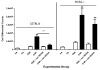
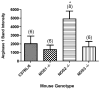
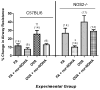
Arginase1 and nitric oxide synthase2 (NOS2) utilize l-arginine as a substrate, with both enzymes expressed at high levels in the asthmatic lung. Inhibition of arginase in ovalbumin-exposed C57BL/6 mice with the transition state inhibitor N(omega)-hydroxy-nor-l-arginine (nor-NOHA) significantly increased total l-arginine content in the airway compartment. We hypothesized that such an increase in l-arginine content would increase the amount of nitric oxide (NO) being produced in the airways and thereby decrease airway hyperreactivity and eosinophilic influx. We further hypothesized that despite arginase inhibition, NOS2 knockout (NOS2-/-) mice would be unable to up-regulate NO production in response to allergen exposure and would demonstrate higher amounts of airway hyperreactivity and eosinophilia under conditions of arginase inhibition than C57BL/6 animals. We found that administration of nor-NOHA significantly decreased airway hyperreactivity and eosinophilic airway inflammation in ovalbumin-exposed C57BL/6 mice, but these parameters were unchanged in ovalbumin-exposed NOS2-/- mice. Arginase1 protein content was increased in mice exposed to ovalbumin, an effect that was reversed upon nor-NOHA treatment in C57BL/6 mice. Arginase1 protein content in the airway compartment directly correlated with the degree of airway hyperreactivity in all treatment groups. NOS2-/- mice had significantly greater arginase1 and arginase2 concentrations compared to their respective C57BL/6 groups, indicating that inhibition of arginase may be dependent upon NOS2 expression. Arginase1 and 2 content were not affected by nor-NOHA administration in the NOS2-/- mice. We conclude that l-arginine metabolism plays an important role in the development of airway hyperreactivity and eosinophilic airway inflammation. Inhibition of arginase early in the allergic inflammatory response decreases the severity of the chronic inflammatory phenotype. These effects appear to be attributable to NOS2, which is a major source of NO production in the inflamed airway, although arginase inhibition may also be affecting the turnover of arginine by the other NOS isoforms, NOS1 and NOS3. The increased l-arginine content in the airway compartment of mice treated with nor-NOHA may directly or indirectly, through NOS2, control arginase expression both in response to OVA exposure and at a basal level.
Figures
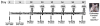




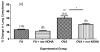
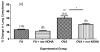

Similar articles
-
Arginase enzymes in isolated airways from normal and nitric oxide synthase 2-knockout mice exposed to ovalbumin.Toxicol Appl Pharmacol. 2009 Feb 1;234(3):273-80. doi: 10.1016/j.taap.2008.10.007. Epub 2008 Nov 5. Toxicol Appl Pharmacol. 2009. PMID: 19027033 Free PMC article.
-
Nitric oxide synthase enzymes in the airways of mice exposed to ovalbumin: NOS2 expression is NOS3 dependent.Mediators Inflamm. 2010;2010:321061. doi: 10.1155/2010/321061. Epub 2010 Oct 5. Mediators Inflamm. 2010. PMID: 20953358 Free PMC article.
-
Increased arginase activity underlies allergen-induced deficiency of cNOS-derived nitric oxide and airway hyperresponsiveness.Br J Pharmacol. 2002 Jun;136(3):391-8. doi: 10.1038/sj.bjp.0704725. Br J Pharmacol. 2002. PMID: 12023942 Free PMC article.
-
[Arginine metabolism in bronchial asthma].Postepy Hig Med Dosw (Online). 2007;61:156-66. Postepy Hig Med Dosw (Online). 2007. PMID: 17410056 Review. Polish.
-
Regulation of nitric oxide production in health and disease.Curr Opin Clin Nutr Metab Care. 2010 Jan;13(1):97-104. doi: 10.1097/MCO.0b013e328332f99d. Curr Opin Clin Nutr Metab Care. 2010. PMID: 19841582 Free PMC article. Review.
Cited by
-
Effect of trigger point injection on lumbosacral radiculopathy source.Anesth Pain Med. 2014 Sep 8;4(4):e15500. doi: 10.5812/aapm.15500. eCollection 2014 Oct. Anesth Pain Med. 2014. PMID: 25337469 Free PMC article.
-
Requirement for inducible nitric oxide synthase in chronic allergen exposure-induced pulmonary fibrosis but not inflammation.J Immunol. 2010 Sep 1;185(5):3076-85. doi: 10.4049/jimmunol.0904214. Epub 2010 Jul 28. J Immunol. 2010. PMID: 20668217 Free PMC article.
-
A physiologic and biochemical profile of clinically rejected lungs on a normothermic ex vivo lung perfusion platform.J Surg Res. 2013 Jul;183(1):75-83. doi: 10.1016/j.jss.2012.11.012. Epub 2012 Nov 27. J Surg Res. 2013. PMID: 23218735 Free PMC article.
-
Arginine as host directed therapy in tuberculosis: insights from modulating arginine metabolism by supplementation and arginase inhibition.One Health Adv. 2025;3(1):5. doi: 10.1186/s44280-025-00070-6. Epub 2025 Mar 21. One Health Adv. 2025. PMID: 40124736 Free PMC article.
-
Simvastatin inhibits goblet cell hyperplasia and lung arginase in a mouse model of allergic asthma: a novel treatment for airway remodeling?Transl Res. 2010 Dec;156(6):335-49. doi: 10.1016/j.trsl.2010.09.003. Transl Res. 2010. PMID: 21078495 Free PMC article.
References
-
- Bagnost T, Berthelot A, Bouhaddi M, Laurant P, André C, Guillaume Y, Demougeot C. Treatment with the arginase inhibitor N(omega)-hydroxy-nor-L-arginine improves vascular function and lowers blood pressure in adult spontaneously hypertensive rat. J Hypertens. 2008;26:1110–1118. - PubMed
-
- Belik J, Shehnaz D, Pan J, Grasemann H. Developmental changes in arginase expression and activity in the lung. Am J Physiol Lung Cell Mol Physiol. 2008;294:L498–504. - PubMed
-
- Berkowitz DE, White R, Li D, Minhas KM, Cernetich A, Kim S, Burke S, Shoukas AA, Nyhan D, Champion HC, Hare JM. Arginase reciprocally regulates nitric oxide synthase activity and contributes to endothelial dysfunction in aging blood vessels. Circulation. 2003;108:2000–2006. - PubMed
-
- Ckless K, Lampert A, Reiss J, Kasahara D, Poynter ME, Irvin CG, Lundblad LK, Norton R, van der Vliet A, Janssen-Heininger YM. Inhibition of arginase activity enhances inflammation in mice with allergic airway disease, in association with increases in protein S-nitrosylation and tyrosine nitration. J Immunol. 2008;181:4255–4264. - PMC - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources

