Joint torques and powers are reduced during ambulation for both limbs in patients with unilateral claudication
- PMID: 19837536
- PMCID: PMC4465243
- DOI: 10.1016/j.jvs.2009.07.117
Joint torques and powers are reduced during ambulation for both limbs in patients with unilateral claudication
Abstract
Objectives: Symptomatic peripheral arterial disease (PAD) results in significant gait impairment. In an attempt to fully delineate and quantify these gait alterations, we analyzed joint kinematics, torques (rotational forces), and powers (rotational forces times angular velocity) in patients with PAD with unilateral claudication for both the affected and nonaffected legs.
Methods: Twelve patients with unilateral PAD (age, 61.69 +/- 10.53 years, ankle-brachial index [ABI]: affected limb 0.59 +/- 0.25; nonaffected limb 0.93 +/- 0.12) and 10 healthy controls (age, 67.23 +/- 12.67 years, ABI >1.0 all subjects) walked over a force platform to acquire gait kinetics, while joint kinematics were recorded simultaneously. Data were collected for the affected and nonaffected limbs during pain free (PAD-PF) and pain induced (PAD-P) trials. Kinetics and kinematics were combined to quantify torque and powers during the stance period from the hip, knee, and ankle joints.
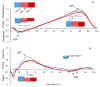
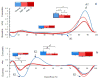
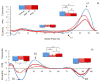
Results: The affected limb demonstrated significantly (P <.05) reduced ankle plantar flexion torque compared to controls during late stance in both PAD-PF and PAD-P trials. There were significant reductions in ankle plantar flexion power generation during late stance for both the affected (P <.05) and nonaffected limbs (P <.05) compared to control during PAD-PF and PAD-P trials. No significant differences were noted in torque comparing the nonaffected limbs in PAD-PF and PAD-P conditions to control for knee and hip joints throughout the stance phase. Significant reductions were found in knee power absorption in early stance and knee power generation during mid stance for both limbs of the patients with PAD as compared to control (P <.05).
Conclusion: Patients with PAD with unilateral claudication demonstrate significant gait impairments in both limbs that are present even before they experience any claudication symptoms. Overall, our data demonstrate significantly reduced ankle plantar flexion torque and power during late stance with reduced knee power during early and mid stance for the affected limb. Further studies are needed to determine if these findings are dependent on the location and the severity of lower extremity ischemia and whether the changes in the nonaffected limb are the result of underlying PAD or compensatory changes from the affected limb dysfunction.
Copyright 2010 Society for Vascular Surgery. Published by Mosby, Inc. All rights reserved.
Figures
References
-
- Hooi JD, Kester AD, Stoffers HE, Overdijk MM, van Ree JW, Knottnerus JA. Incidence of and risk factors for asymptomatic peripheral arterial occlusive disease: a longitudinal study. Am J Epidemiol. 2001;153(7):666–672. - PubMed
-
- Atkins LM, Gardner AW. The relationship between lower extremity functional strength and severity of peripheral arterial disease. Angiology. 2004;55(4):347–355. - PubMed
-
- Gardner AW, Clancy RJ. The relationship between ankle-brachial index and leisure-time physical activity in patients with intermittent claudication. Angiology. 2006;57(5):539–545. - PubMed
-
- Liles DR, Kallen MA, Petersen LA, Bush RL. Quality of life and peripheral arterial disease. J Surg Res. 2006;136(2):294–301. - PubMed
-
- Regensteiner JG, Stewart KJ. Established and evolving medical therapies for claudication in patients with peripheral arterial disease. Nat Clin Pract Cardiovasc Med. 2006;3(11):604–610. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources

