Hypocalcemia following resuscitation from cardiac arrest revisited
- PMID: 19913975
- PMCID: PMC2815084
- DOI: 10.1016/j.resuscitation.2009.10.002
Hypocalcemia following resuscitation from cardiac arrest revisited
Abstract
Objective: Hypocalcemia associated with cardiac arrest has been reported. However, mechanistic hypotheses for the decrease in ionized calcium (iCa) vary and its importance unknown. The objective of this study was to assess the relationships of iCa, pH, base excess (BE), and lactate in two porcine cardiac arrest models, and to determine the effect of exogenous calcium administration on post-resuscitation hemodynamics.
Methods: Swine were instrumented and VF was induced either electrically (EVF, n=65) or spontaneously, ischemically induced (IVF) with balloon occlusion of the LAD (n=37). Animals were resuscitated after 7 min of VF. BE, iCa, and pH, were determined prearrest and at 15, 30, 60, 90, 120 min after ROSC. Lactate was also measured in 26 animals in the EVF group. Twelve EVF animals were randomized to receive 1g of CaCl(2) infused over 20 min after ROSC or normal saline.
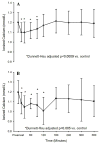
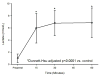
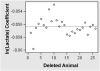
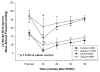
Results: iCa, BE, and pH declined significantly over the 60 min following ROSC, regardless of VF type, with the lowest levels observed at the nadir of left ventricular stroke work post-resuscitation. Lactate was strongly correlated with BE (r=-0.89, p<0.0001) and iCa (r=-0.40, p<0.0001). In a multivariate generalized linear mixed model, iCa was 0.005 mg/dL higher for every one unit increase in BE (95% CI 0.003-0.007, p<0.0001), while controlling for type of induced VF. While there was a univariate correlation between iCa and BE, when BE was included in the regression analysis with lactate, only lactate showed a statistically significant relationship with iCa (p=0.02). Post-resuscitation CaCl(2) infusion improved post-ROSC hemodynamics when compared to saline infusion (LV stroke work control 8+/-5 gm vs 23+/-4, p=0.014, at 30 min) with no significant difference in tau between groups.
Conclusions: Ionized hypocalcemia occurs following ROSC. CaCl(2) improves post-ROSC hemodynamics suggesting that hypocalcemia may play a role in early post-resuscitation myocardial dysfunction.
Copyright 2009 Elsevier Ireland Ltd. All rights reserved.
Conflict of interest statement
Conflicts of Interest: None
Figures
References
-
- Neumar RW, Nolan JP, Adrie C, et al. Post-cardiac arrest syndrome. Epidemiology, pathophysiology, treatment, and prognostication. Circulation. 2008;79:350–79. - PubMed
-
- Kern KB, Hilwig RW, Rhee KH, Berg RA. Myocardial dysfunction after resuscitation from cardiac arrest; An example of global myocardial stunning. J Am Coll Cardiol. 1996;28:232–240. - PubMed
-
- Walcott GP, Killingsworth CR, Ideker RE. Do clinically relevant transthoracic defibrillation energies cause myocardial damage dysfunction? Resuscitation. 2003;59:59–70. - PubMed
-
- Tang W, Weil MH, Sun S, Noc M, Yang L, Gazmuri RJ. Epinephrine increases the severity of postresuscitation myocardial dysfunction. Circulation. 1995;92:3089–2093. - PubMed
-
- Morgan JP, Perreault CL, Morgan KG. The cellular basis of contraction and relaxation in cardiac and vascular smooth muscle. Am Heart J. 1991;121:961–968. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

