Insulin resistance and hyperinsulinaemia in the development and progression of cancer
- PMID: 19922415
- PMCID: PMC2782313
- DOI: 10.1042/CS20090399
Insulin resistance and hyperinsulinaemia in the development and progression of cancer
Abstract
Experimental, epidemiological and clinical evidence implicates insulin resistance and its accompanying hyperinsulinaemia in the development of cancer, but the relative importance of these disturbances in cancer remains unclear. There are, however, theoretical mechanisms by which hyperinsulinaemia could amplify such growth-promoting effects as insulin may have, as well as the growth-promoting effects of other, more potent, growth factors. Hyperinsulinaemia may also induce other changes, particularly in the IGF (insulin-like growth factor) system, that could promote cell proliferation and survival. Several factors can independently modify both cancer risk and insulin resistance, including subclinical inflammation and obesity. The possibility that some of the effects of hyperinsulinaemia might then augment pro-carcinogenic changes associated with disturbances in these factors emphasizes how, rather than being a single causative factor, insulin resistance may be most usefully viewed as one strand in a network of interacting disturbances that promote the development and progression of cancer.
Figures


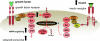


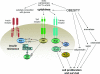
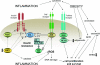
References
-
- Giovannucci E., Colditz G. A., Stampfer M. J., Willett W. C. Physical activity, obesity, and risk of colorectal adenoma in women (United States) Cancer Causes Control. 1996;7:253–263. - PubMed
-
- Calle E. E., Thun M. J. Obesity and cancer. Oncogene. 2004;23:6365–6378. - PubMed
-
- Schoen R. E., Tangen C. M., Kuller L. H., Burke G. L., Cushman M., Tracy R. P., Dobs A., Savage P. J. Increased blood glucose and insulin, body size, and incident colorectal cancer. J. Natl. Cancer Inst. 1999;91:1147–1154. - PubMed
-
- Coughlin S. S., Calle E. E., Teras L. R., Petrelli J., Thun M. J. Diabetes mellitus as a predictor of cancer mortality in a large cohort of US adults. Am. J. Epidemiol. 2004;159:1160–1167. - PubMed
-
- Rapp K., Schroeder J., Klenk J., Ulmer H., Concin H., Diem G., Oberaigner W., Weiland S. K. Fasting blood glucose and cancer risk in a cohort of more than 140,000 adults in Austria. Diabetologia. 2006;49:945–952. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources

