Diet composition affects surgery-associated weight loss in rats with a compromised alimentary tract
- PMID: 19932903
- PMCID: PMC2888995
- DOI: 10.1016/j.jss.2009.08.003
Diet composition affects surgery-associated weight loss in rats with a compromised alimentary tract
Abstract
Background: Esophageal adenocarcinoma (EAC) is the fastest growing cancer in terms of incidence and has a high mortality rate. The animal model to study EAC uses esophagoduodenal anastomosis (EDA) to induce mixed-reflux (bile/acid) causing esophagitis, Barrett's esophagus, and EAC sequence within 6 mo. However, the lack of fully functional stomach in these rats leads to the development of malnutrition.
Methods: We have assessed the ability of a chemically pure, purified ingredient diet (AIN-93M) to reduce surgery-associated malnutrition in rats that have undergone the EDA-surgery. Animals were either sham- (SH) or EDA-operated and fed either a grain-based rodent diet (RD) (SH-RD, n=3; EDA-RD, n=10) or a purified diet (PD) (SH-PD, n=4; EDA-PD, n=11). The animals were weighed periodically for assessment of weight gain and euthanized at the end of 24 wk to measure esophageal tumor incidence.
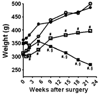
Results: Animals that underwent sham surgery continued to gain weight throughout the study period and no tumors were detected. The EDA-operated animals had significantly lower weight gain compared with sham animals. There was no significant difference in weight gain among EDA animals fed two different types of diets until 9 wk after the surgery. After 9 wk, EDA-RD continued to lose weight significantly, whereas the weight loss leveled in EDA-PD (P<0.001). At termination, neither tissue histopathology nor tumor incidence was significantly different between the groups.
Conclusion: These results show that compared with a natural ingredient diet, a purified ingredient diet can reduce surgery-associated weight loss in rats with a compromised alimentary tract. This reduction in malnutrition has the potential to reduce the confounding effects of weight loss on future animal studies reported.
Copyright © 2011 Elsevier Inc. All rights reserved.
Conflict of interest statement
Disclosure: Authors have no potential conflicts of interest.
Figures

Similar articles
-
Effect of freeze-dried berries on the development of reflux-induced esophageal adenocarcinoma.Nutr Cancer. 2011 Nov;63(8):1256-62. doi: 10.1080/01635581.2011.609307. Epub 2011 Nov 1. Nutr Cancer. 2011. PMID: 22043833
-
Dietary freeze-dried black raspberry's effect on cellular antioxidant status during reflux-induced esophagitis in rats.Nutrition. 2011 Feb;27(2):182-7. doi: 10.1016/j.nut.2010.01.007. Epub 2010 Jun 11. Nutrition. 2011. PMID: 20538426 Free PMC article.
-
Oxidative damage in an esophageal adenocarcinoma model with rats.Carcinogenesis. 2000 Feb;21(2):257-63. doi: 10.1093/carcin/21.2.257. Carcinogenesis. 2000. PMID: 10657966
-
Studies on experimental animals involving surgical procedures and/or nitrosamine treatment related to the etiology of esophageal adenocarcinoma.Cancer Lett. 1997 Aug 19;117(2):161-74. doi: 10.1016/s0304-3835(97)00228-0. Cancer Lett. 1997. PMID: 9377544 Review.
-
Rat Reflux Model of Esophageal Cancer and Its Implication in Human Disease.Ann Surg. 2015 Dec;262(6):910-24. doi: 10.1097/SLA.0000000000001207. Ann Surg. 2015. PMID: 25822684 Review.
Cited by
-
Hepatic protection and anticancer activity of curcuma: a potential chemopreventive strategy against hepatocellular carcinoma.Int J Oncol. 2014 Feb;44(2):505-13. doi: 10.3892/ijo.2013.2184. Epub 2013 Nov 21. Int J Oncol. 2014. PMID: 24270742 Free PMC article.
-
Effect on pro-inflammatory and antioxidant genes and bioavailable distribution of whole turmeric vs curcumin: Similar root but different effects.Food Chem Toxicol. 2012 Feb;50(2):227-31. doi: 10.1016/j.fct.2011.10.070. Epub 2011 Nov 4. Food Chem Toxicol. 2012. PMID: 22079310 Free PMC article.
-
Impact of dietary ingredients on the interpretation of various fecal parameters in rats fed inulin.J Food Drug Anal. 2019 Oct;27(4):869-875. doi: 10.1016/j.jfda.2019.06.005. Epub 2019 Jul 16. J Food Drug Anal. 2019. PMID: 31590758 Free PMC article.
References
-
- Jemal A, Thun MJ, Ries LA, Howe HL, Weir HK, Center MM, Ward E, Wu XC, Eheman C, et al. Annual report to the nation on the status of cancer, 1975–2005, featuring trends in lung cancer, tobacco use, and tobacco control. Journal of the National Cancer Institute. 2008 Dec 3;100:1672–1694. - PMC - PubMed
-
- Jemal A, Siegel R, Ward E, Hao Y, Xu J, Murray T, Thun MJ. Cancer statistics, 2008. CA: a cancer journal for clinicians. 2008 Mar–pr;58:71–96. - PubMed
-
- Freedman ND, Abnet CC, Leitzmann MF, Mouw T, Subar AF, Hollenbeck AR, Schatzkin A. A prospective study of tobacco, alcohol, and the risk of esophageal and gastric cancer subtypes. American journal of epidemiology. 2007 Jun 15;165:1424–1433. - PubMed
-
- Trivers KF, Sabatino SA, Stewart SL. Trends in esophageal cancer incidence by histology, United States, 1998–2003. International journal of cancer. 2008 Sep 15;123:1422–1428. - PubMed
-
- Vaughan TL, Davis S, Kristal A, Thomas DB. Obesity, alcohol, and tobacco as risk factors for cancers of the esophagus and gastric cardia: adenocarcinoma versus squamous cell carcinoma. Cancer Epidemiol Biomarkers Prev. 1995 Mar;4:85–92. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

