Endovascular management of the popliteal artery: comparison of atherectomy and angioplasty
- PMID: 19942598
- PMCID: PMC4429911
- DOI: 10.1177/1538574409345028
Endovascular management of the popliteal artery: comparison of atherectomy and angioplasty
Abstract
Purpose: Symptomatic atherosclerotic disease of the popliteal artery presents challenges for endovascular therapy. We evaluated the technical success, complications, and midterm outcomes of atherectomy and angioplasty involving the popliteal segment.
Methods: We conducted a retrospective review of outcomes of popliteal artery intervention using atherectomy or angioplasty performed between 2003 and 2008.
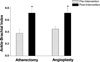
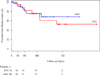
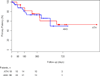
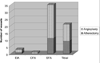
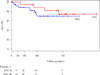
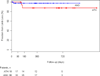
Results: A total of 56 patients (36% women, age 72.8 +/- 12.2 years, 77% critical limb ischemia) underwent popliteal atherectomy (n = 18) or angioplasty (n = 38). These patients had similar clinical characteristics, TransAtlantic Intersociety Consensus (TASC)/ TASC II classification, mean lesion length, and runoff scores. We observed a trend toward higher rates of technical success defined as <30% residual stenosis after atherectomy compared to angioplasty (94% vs 71%, P = .08). While angioplasty was associated with a higher frequency of arterial dissection (23% vs 0%, P = .003), atherectomy was associated with a higher rate of thromboembolic events (22% vs 0%, P = 0.01). Adjunctive stenting was used more frequently following angioplasty compared to atherectomy (45% vs 6%, P = .005). Thrombolysis was used to treat embolization in 4 patients in the atherectomy group. The improvement in the ankle-brachial index (ABI) was similar between the 2 treatment groups. Primary patency of the popliteal artery at 3, 6, and 12 months was 94%, 88%, and 75% in the atherectomy group and 89%, 82%, and 73% in the angioplasty group (P = not significant [NS]). There were no significant differences in limb salvage and freedom from reintervention at 1 year between the atherectomy and angioplasty groups.
Conclusions: Our experience with popliteal artery endovascular therapy indicates a distinct pattern of procedural complications with atherectomy compared to angioplasty but similar midterm patency, limb salvage, and freedom from intervention.
Figures
Similar articles
-
Endovascular Management of Severe Peripheral Artery Disease Isolated to the Popliteal Artery Shows Comparable Outcomes Regardless of Treatment Modality.Ann Vasc Surg. 2025 May;114:203-211. doi: 10.1016/j.avsg.2025.01.046. Epub 2025 Mar 5. Ann Vasc Surg. 2025. PMID: 40054603
-
Primary stenting of the superficial femoral and popliteal artery.J Vasc Surg. 2009 Sep;50(3):542-7. doi: 10.1016/j.jvs.2009.04.019. Epub 2009 Jun 21. J Vasc Surg. 2009. PMID: 19540706
-
Late outcomes of balloon angioplasty and angioplasty with selective stenting for superficial femoral-popliteal disease are equivalent.J Vasc Surg. 2011 Oct;54(4):1051-1057.e1. doi: 10.1016/j.jvs.2011.03.283. Epub 2011 Jun 2. J Vasc Surg. 2011. PMID: 21636240
-
Critical appraisal of the contemporary use of atherectomy to treat femoropopliteal atherosclerotic disease.J Vasc Surg. 2022 Feb;75(2):697-708.e9. doi: 10.1016/j.jvs.2021.07.106. Epub 2021 Jul 22. J Vasc Surg. 2022. PMID: 34303802
-
Contemporary endovascular treatment for disease of the superficial femoral and popliteal arteries: an integrated device-based strategy.J Endovasc Ther. 2006 Feb;13 Suppl 2:II41-51. doi: 10.1177/15266028060130S208. J Endovasc Ther. 2006. PMID: 16472010 Review.
Cited by
-
Efficacy of endoluminal interventional therapy in diabetic peripheral arterial occlusive disease: a retrospective trial.Cardiovasc Diabetol. 2012 Feb 28;11:17. doi: 10.1186/1475-2840-11-17. Cardiovasc Diabetol. 2012. PMID: 22373102 Free PMC article.
-
An Endovascular Strategy for Occlusion or Stenosis with Severe Calcification in the Non-Stenting Zone, creatinG Lumens And SlitS with Crosser in Unique Technique (GLASS CUT): A Case Report.Ann Vasc Dis. 2017 Dec 25;10(4):426-429. doi: 10.3400/avd.cr.17-00041. Ann Vasc Dis. 2017. PMID: 29515708 Free PMC article.
-
Twelve-Month Outcomes of Intravascular Lithotripsy for Treatment of Calcified Popliteal and Infrapopliteal Lesions in Patients With Chronic Limb-Threatening Ischemia.J Endovasc Ther. 2025 Aug;32(4):1127-1134. doi: 10.1177/15266028231205421. Epub 2023 Oct 18. J Endovasc Ther. 2025. PMID: 37853746 Free PMC article.
-
Intravascular Lithotripsy in Calcified Peripheral Lesions: Single-Center JEN-Experience.Int J Angiol. 2022 Aug 25;32(1):11-20. doi: 10.1055/s-0042-1751229. eCollection 2023 Mar. Int J Angiol. 2022. PMID: 36727147 Free PMC article.
-
Treatment extent of femoropopliteal disease and clinical outcomes following endovascular therapy.EuroIntervention. 2024 Sep 16;20(18):e1154-e1162. doi: 10.4244/EIJ-D-24-00037. EuroIntervention. 2024. PMID: 39279516
References
-
- Anderson PL, Gelijns A, Moskowitz A, et al. Understanding trends in inpatient surgical volume: Vascular interventions, 1980–2000. J Vasc Surg. 2004;39:1200–1208. - PubMed
-
- TASC. Management of Peripheral Arterial Disease (PAD) TransAtlantic Intersociety Consensus (TASC) J Vasc Surg. 2000;31(1part 2):S1–S287. - PubMed
-
- Norgren L, Hiatt WR, Dormandy JA, et al. Inter-Society Consensus for the Management of Peripheral Artery Disease (TASC II) J Vasc Surg. 2007 Jan;45(Suppl S):S1–S67. - PubMed
-
- Zeller T, Rastan A, Sixt S, et al. Long-term results after directional atherectomy of femoro-popliteal lesions. J Am Coll Cardiol. 2006;48:1573–1578. - PubMed
-
- Zeller T, Rastan A, Schwarzwälder U, et al. Percutaneous peripheral atherectomy of femoropopliteal stenoses using a new-generation device: six-month results from a single-center experience. J Endovasc Ther. 2004;11:676–685. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

