Angiotensin II in experimental hyperdynamic sepsis
- PMID: 19948019
- PMCID: PMC2811902
- DOI: 10.1186/cc8185
Angiotensin II in experimental hyperdynamic sepsis
Abstract
Introduction: Angiotensin II (Ang II) is a potential vasopressor treatment for hypotensive hyperdynamic sepsis. However, unlike other vasopressors, its systemic, regional blood flow and renal functional effects in hypotensive hyperdynamic sepsis have not been investigated.
Methods: We performed an experimental randomised placebo-controlled animal study. We induced hyperdynamic sepsis by the intravenous administration of live E. coli in conscious ewes after chronic instrumentation with flow probes around the aorta and the renal, mesenteric, coronary and iliac arteries. We allocated animals to either placebo or angiotensin II infusion titrated to maintain baseline blood pressure.
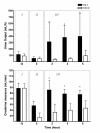
Results: Hyperdynamic sepsis was associated with increased renal blood flow (from 292 +/- 61 to 397 +/- 74 ml/min), oliguria and a decrease in creatinine clearance (from 88.7 +/- 19.6 to 47.7 +/- 21.0 ml/min, P < 0.0001). Compared to placebo, Ang II infusion restored arterial pressure but reduced renal blood flow (from 359 +/- 81 ml/min to 279 +/- 86 ml/min; P < 0.0001). However, despite the reduction in renal blood flow, Ang II increased urine output approximately 7-fold (364 +/- 272 ml/h vs. 48 +/- 18 ml/h; P < 0.0001), and creatinine clearance by 70% (to 80.6 +/- 20.7 ml/min vs.46.0 +/- 26 ml/min; P < 0.0001). There were no major effects of Ang II on other regional blood flows.
Conclusions: In early experimental hypotensive hyperdynamic sepsis, intravenous angiotensin II infusion decreased renal blood while inducing a marked increase in urine output and normalizing creatinine clearance.
Figures



References
-
- Uchino S, Kellum JA, Bellomo R, Doig GS, Morimatsu H, Morgera S, Schetz M, Tan I, Bouman C, Macedo E, Gibney N, Tolwani A, Ronco C. beginning and Ending Supportive Therapy for the kidney (BEST kidney) investigators. Acute renal failure in critically ill patients: a multinational, multicenter study. JAMA. 2005;294:813–818. doi: 10.1001/jama.294.7.813. - DOI - PubMed
-
- Bellomo R, Ronco C. Renal replacement therapy in the intensive care unit. Crit Care Resusc. 1999;1:13–24. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

