Risk factors for neonatal conjunctivitis in babies of HIV-1 infected mothers
- PMID: 19995198
- PMCID: PMC3223245
- DOI: 10.3109/09286580903144746
Risk factors for neonatal conjunctivitis in babies of HIV-1 infected mothers
Abstract
Purpose: To determine the prevalence and correlates of neonatal conjunctivitis in infants born to human immunodeficiency virus type 1 (HIV-1) infected mothers.
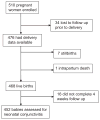
Methods: This was a nested case-control study within a perinatal HIV-1 cohort. HIV-1 seropositive mothers were enrolled during pregnancy and mother-infant pairs followed after delivery with assessment for neonatal conjunctivitis at 48 hours and up to 4 weeks after birth. Genital infections (chlamydia, gonorrhea, syphilis, trichomonas, bacterial vaginosis, and candida) were screened for at 32 weeks gestation. Mothers received treatment for genital infections diagnosed during pregnancy and short-course zidovudine. Newborns did not receive ocular prophylaxis at hospital deliveries. Multivariate logistic regression models were used to determine cofactors for neonatal conjunctivitis overall and stratified for infant HIV-1 status.
Results: Four hundred and fifty-two infants were assessed and 101 (22.3%) had neonatal conjunctivitis during the first month postpartum. In multivariate analyses using odds ratios (OR) and confidence intervals (CI), neonatal conjunctivitis was associated with neonatal sepsis (adjusted OR 21.95, 95% CI 1.76, 274.61), birth before arrival to hospital (adjusted OR 13.91, 95% CI 1.39, 138.78) and birth weight (median 3.4 versus 3.3 kilograms, p=0.016, OR 1.79, 95% CI 1.01, 3.15). Infant HIV-1 infection was not associated with conjunctivitis.
Conclusions: Despite detection and treatment of genital infections during pregnancy, neonatal conjunctivitis was frequently diagnosed in infants born to HIV-1 infected mothers suggesting a need for increased vigilance and prophylaxis for conjunctivitis in these infants. Neonatal sepsis, birth before arrival to hospital, and higher birthweight are factors that may predict higher risk of neonatal conjunctivitis in this population.
Conflict of interest statement
Figures
Similar articles
-
Neonatal predictors of infection status and early death among 332 infants at risk of HIV-1 infection monitored prospectively from birth. New York City Perinatal HIV Transmission Collaborative Study Group.Pediatrics. 1995 Sep;96(3 Pt 1):451-8. Pediatrics. 1995. PMID: 7651777
-
The effect of human immunodeficiency virus infection on birthweight, and infant and child mortality in urban Malawi.Int J Epidemiol. 1995 Oct;24(5):1022-9. doi: 10.1093/ije/24.5.1022. Int J Epidemiol. 1995. PMID: 8557435
-
Identification of levels of maternal HIV-1 RNA associated with risk of perinatal transmission. Effect of maternal zidovudine treatment on viral load.JAMA. 1996 Feb 28;275(8):599-605. JAMA. 1996. PMID: 8594240
-
Antivirals for prevention of hepatitis B virus mother-to-child transmission in human immunodeficiency virus positive pregnant women co-infected with hepatitis B virus.Cochrane Database Syst Rev. 2023 Jun 12;6(6):CD013653. doi: 10.1002/14651858.CD013653.pub2. Cochrane Database Syst Rev. 2023. PMID: 37306558 Free PMC article. Review.
-
Pediatric AIDS and perinatal HIV infection in Zaire: epidemiologic and pathologic findings.Prog AIDS Pathol. 1992;3(1):1-33. Prog AIDS Pathol. 1992. PMID: 1606299 Review.
Cited by
-
The Association between Gestational Age and Risk for Long Term Ophthalmic Morbidities among Offspring Delivered in Different Preterm Subgroups.J Clin Med. 2022 May 2;11(9):2562. doi: 10.3390/jcm11092562. J Clin Med. 2022. PMID: 35566688 Free PMC article.
-
Adverse pregnancy and neonatal outcomes associated with Neisseria gonorrhoeae: systematic review and meta-analysis.Sex Transm Infect. 2021 Mar;97(2):104-111. doi: 10.1136/sextrans-2020-054653. Epub 2021 Jan 12. Sex Transm Infect. 2021. PMID: 33436505 Free PMC article.
-
Preterm infants with positive conjunctival swab culture: risk factors and association with late-onset sepsis-a retrospective cohort study.Front Pediatr. 2023 Nov 15;11:1259558. doi: 10.3389/fped.2023.1259558. eCollection 2023. Front Pediatr. 2023. PMID: 38046677 Free PMC article.
-
Epidemiology of ophthalmia neonatorum: a systematic review and meta-analysis.BMC Pediatr. 2025 Jan 14;25(1):31. doi: 10.1186/s12887-024-05382-x. BMC Pediatr. 2025. PMID: 39810179 Free PMC article.
References
-
- Fransen L, Klauss V. Neonatal ophthalmia in the developing world. Epidemiology, etiology, management and control. Int Ophthalmol. 1988;11(3):189–196. - PubMed
-
- Verma M, Chhatwal J, Varughese PV. Neonatal conjunctivitis: a profile. Indian Pediatr. 1994;31(11):1357–1361. - PubMed
-
- Woods CR. Gonococcal infections in neonates and young children. Semin Pediatr Infect Dis. 2005;16(4):258–270. - PubMed
-
- Zar JH. Neonatal chlamydia infections, prevention and treatment. Pediatr Drugs. 2005;7(2):103–110. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical