Increasing risk of revision due to deep infection after hip arthroplasty
- PMID: 19995313
- PMCID: PMC2823304
- DOI: 10.3109/17453670903506658
Increasing risk of revision due to deep infection after hip arthroplasty
Abstract
Background and purpose: Over the decades, improvements in surgery and perioperative routines have reduced the incidence of deep infections after total hip arthroplasty (THA). There is, however, some evidence to suggest that the incidence of infection is increasing again. We assessed the risk of revision due to deep infection for primary THAs reported to the Norwegian Arthroplasty Register (NAR) over the period 1987-2007.
Method: We included all primary cemented and uncemented THAs reported to the NAR from September 15, 1987 to January 1, 2008 and performed adjusted Cox regression analyses with the first revision due to deep infection as endpoint. Changes in revision rate as a function of the year of operation were investigated.
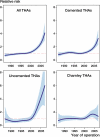
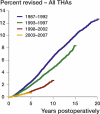
Results: Of the 97,344 primary THAs that met the inclusion criteria, 614 THAs had been revised due to deep infection (5-year survival 99.46%). Risk of revision due to deep infection increased throughout the period studied. Compared to the THAs implanted in 1987-1992, the risk of revision due to infection was 1.3 times higher (95%CI: 1.0-1.7) for those implanted in 1993-1997, 1.5 times (95% CI: 1.2-2.0) for those implanted in 1998-2002, and 3.0 times (95% CI: 2.2-4.0) for those implanted in 2003-2007. The most pronounced increase in risk of being revised due to deep infection was for the subgroup of uncemented THAs from 2003-2007, which had an increase of 5 times (95% CI: 2.6-11) compared to uncemented THAs from 1987-1992.
Interpretation: The incidence of deep infection after THA increased during the period 1987-2007. Concomitant changes in confounding factors, however, complicate the interpretation of the results.
Figures
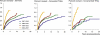
Comment in
-
Joint prosthetic infections: a success story or a continuous concern?Acta Orthop. 2009 Dec;80(6):629-32. doi: 10.3109/17453670903487016. Acta Orthop. 2009. PMID: 19995311 Free PMC article. No abstract available.
References
-
- Anderson DJ, Sexton DJ, Kanafani ZA, Auten G, Kaye KS. Severe surgical site infection in community hospitals: epidemiology, key procedures. and the changing prevalence of methicillin-resistant Staphylococcus aureus. Infect Control Hosp Epidemiol. 2007;28:1047–53. - PubMed
-
- Arthursson AJ, Furnes O, Espehaug B, Havelin LI, Soreide JA. Validation of data in the Norwegian Arthroplasty Register and the Norwegian Patient Register: 5,134 primary total hip arthroplasties and revisions operated at a single hospital between 1987 and 2003. Acta Orthop. 2005;76:823–8. - PubMed
-
- Block JE, Stubbs HA. Reducing the risk of deep wound infection in primary joint arthroplasty with antibiotic bone cement. Orthopedics. 2005;28:1334–45. - PubMed
-
- Charnley J. Postoperative infection after total hip replacement with special reference to air contamination in the operating room. Clin Orthop. 1972;((87)):167–87. - PubMed
-
- Dempsey KE, Riggio MP, Lennon A, Hannah VE, Ramage G, Allan D, Bagg J. Identification of bacteria on the surface of clinically infected and non-infected prosthetic hip joints removed during revision arthroplasties by 16S rRNA gene sequencing and by microbiological culture. Arthritis Res Ther. 2007;9:R46. - PMC - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous
