Plasma ATP concentration and venous oxygen content in the forearm during dynamic handgrip exercise
- PMID: 20003530
- PMCID: PMC2801472
- DOI: 10.1186/1472-6793-9-24
Plasma ATP concentration and venous oxygen content in the forearm during dynamic handgrip exercise
Abstract
Background: It has been proposed that adenosine triphosphate (ATP) released from red blood cells (RBCs) may contribute to the tight coupling between blood flow and oxygen demand in contracting skeletal muscle. To determine whether ATP may contribute to the vasodilatory response to exercise in the forearm, we measured arterialised and venous plasma ATP concentration and venous oxygen content in 10 healthy young males at rest, and at 30 and 180 seconds during dynamic handgrip exercise at 45% of maximum voluntary contraction (MVC).
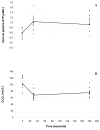
Results: Venous plasma ATP concentration was elevated above rest after 30 seconds of exercise (P < 0.05), and remained at this higher level 180 seconds into exercise (P < 0.05 versus rest). The increase in ATP was mirrored by a decrease in venous oxygen content. While there was no significant relationship between ATP concentration and venous oxygen content at 30 seconds of exercise, they were moderately and inversely correlated at 180 seconds of exercise (r = -0.651, P = 0.021). Arterial ATP concentration remained unchanged throughout exercise, resulting in an increase in the venous-arterial ATP difference.
Conclusions: Collectively these results indicate that ATP in the plasma originated from the muscle microcirculation, and are consistent with the notion that deoxygenation of the blood perfusing the muscle acts as a stimulus for ATP release. That ATP concentration was elevated just 30 seconds after the onset of exercise also suggests that ATP may be a contributing factor to the blood flow response in the transition from rest to steady state exercise.
Figures
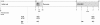
Similar articles
-
Mechanical effects of muscle contraction increase intravascular ATP draining quiescent and active skeletal muscle in humans.J Appl Physiol (1985). 2013 Apr;114(8):1085-93. doi: 10.1152/japplphysiol.01465.2012. Epub 2013 Feb 21. J Appl Physiol (1985). 2013. PMID: 23429876 Free PMC article.
-
Rho-kinase inhibition improves haemodynamic responses and circulating ATP during hypoxia and moderate intensity handgrip exercise in healthy older adults.J Physiol. 2022 Jul;600(14):3265-3285. doi: 10.1113/JP282730. Epub 2022 May 29. J Physiol. 2022. PMID: 35575293 Free PMC article. Clinical Trial.
-
Sources of intravascular ATP during exercise in humans: critical role for skeletal muscle perfusion.Exp Physiol. 2013 May;98(5):988-98. doi: 10.1113/expphysiol.2012.071555. Epub 2013 Jan 11. Exp Physiol. 2013. PMID: 23315195 Free PMC article.
-
ATP as a mediator of erythrocyte-dependent regulation of skeletal muscle blood flow and oxygen delivery in humans.J Physiol. 2012 Oct 15;590(20):5001-13. doi: 10.1113/jphysiol.2012.235002. Epub 2012 Jun 18. J Physiol. 2012. PMID: 22711955 Free PMC article. Review.
-
Regulation of the skeletal muscle blood flow in humans.Exp Physiol. 2014 Dec 1;99(12):1552-8. doi: 10.1113/expphysiol.2014.081620. Epub 2014 Sep 5. Exp Physiol. 2014. PMID: 25192730 Review.
Cited by
-
Dynamic increase in extracellular ATP accelerates photoreceptor cell apoptosis via ligation of P2RX7 in subretinal hemorrhage.PLoS One. 2013;8(1):e53338. doi: 10.1371/journal.pone.0053338. Epub 2013 Jan 8. PLoS One. 2013. PMID: 23308196 Free PMC article.
-
Potential role of passively increased muscle temperature on contractile function.Eur J Appl Physiol. 2022 Oct;122(10):2153-2162. doi: 10.1007/s00421-022-04991-7. Epub 2022 Jun 30. Eur J Appl Physiol. 2022. PMID: 35771296 Free PMC article. Review.
-
Mechanical effects of muscle contraction increase intravascular ATP draining quiescent and active skeletal muscle in humans.J Appl Physiol (1985). 2013 Apr;114(8):1085-93. doi: 10.1152/japplphysiol.01465.2012. Epub 2013 Feb 21. J Appl Physiol (1985). 2013. PMID: 23429876 Free PMC article.
-
Effectiveness of high intensity and sprint interval training on metabolic biomarkers, body composition, and physical fitness in adolescents: randomized controlled trial.Front Public Health. 2024 Jul 31;12:1425191. doi: 10.3389/fpubh.2024.1425191. eCollection 2024. Front Public Health. 2024. PMID: 39157534 Free PMC article. Clinical Trial.
-
In pursuit of P2X3 antagonists: novel therapeutics for chronic pain and afferent sensitization.Purinergic Signal. 2012 Feb;8(Suppl 1):3-26. doi: 10.1007/s11302-011-9271-6. Epub 2011 Nov 18. Purinergic Signal. 2012. PMID: 22095157 Free PMC article.
References
-
- Ellsworth ML, Forrester T, Ellis CG, Dietrich HH. The erythrocyte as a regulator of vascular tone. Am J Physiol Heart Circ Physiol. 1995;269:H2155–2161. - PubMed
-
- Jagger JE, Bateman RM, Ellsworth ML, Ellis CG. Role of erythrocyte in regulating local O2 delivery mediated by hemoglobin oxygenation. Am J Physiol Heart Circ Physiol. 2001;280:H2833–2839. - PubMed
-
- Sprague RS, Stephenson AH, Ellsworth ML, Keller C, Lonigro AJ. Impaired Release of ATP from Red Blood Cells of Humans with Primary Pulmonary Hypertension. Experimental Biology and Medicine. 2001;226:434–439. - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources

