Hypoxia and the expression of HIF-1alpha and HIF-2alpha in the retina of streptozotocin-injected mice and rats
- PMID: 20005221
- PMCID: PMC2824016
- DOI: 10.1016/j.exer.2009.12.002
Hypoxia and the expression of HIF-1alpha and HIF-2alpha in the retina of streptozotocin-injected mice and rats
Abstract
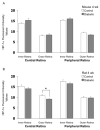
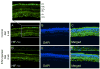
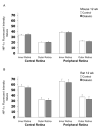
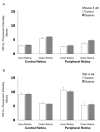
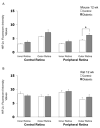
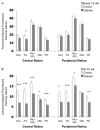
Decreases in retinal blood flow in diabetics could render the retina hypoxic. In mouse and rat models of diabetes, a decrease in retinal blood flow occurs early, within 3-4 weeks of the induction of hyperglycemia, although information is scarce on whether this early decrease in flow induces hypoxia. The purpose of the current study was to determine whether hypoxia-inducible factor (HIF) levels increase following 4 and/or 12 weeks of hyperglycemia in streptozotocin (STZ)-injected mouse (C57BL/6) and rat (Wistar) retinas. Additionally, retinal tissue hypoxia was measured with pimonidazole following 12 weeks of hyperglycemia. These aims were accomplished via immunostaining of cross-sections from enucleated eyes. In mice, staining for HIF-1alpha and HIF-2alpha showed a contrasting pattern, with HIF-1alpha higher in the inner retina than outer, but HIF-2alpha higher in the outer retina than inner. However, in rats, staining for both HIF-1alpha and HIF-2alpha was more intense in the inner retina. The HIF-1alpha staining intensities and patterns were similar between diabetic animals and their non-diabetic counterparts following 4 and 12 weeks of hyperglycemia. The same was true for HIF-2alpha except for a trend toward an increase following 12 weeks of hyperglycemia in mice. Pimonidazole staining showed significant decreases throughout all layers of the central retina and most layers of the peripheral retina of rats (but not mice), following 12 weeks of hyperglycemia. In summary, despite early decreases in flow in rats and mice, retinal HIF-1alpha and HIF-2alpha were not found to be increased, and the extent of hypoxia may even decrease after 12 weeks of hyperglycemia in rats.
Figures


Similar articles
-
PACAP Modulates Expression of Hypoxia-Inducible Factors in Streptozotocin-Induced Diabetic Rat Retina.J Mol Neurosci. 2015 Dec;57(4):501-9. doi: 10.1007/s12031-015-0621-7. Epub 2015 Jul 23. J Mol Neurosci. 2015. PMID: 26202258
-
Increase in retinal hypoxia-inducible factor-2α, but not hypoxia, early in the progression of diabetes in the rat.Exp Eye Res. 2011 Oct;93(4):437-41. doi: 10.1016/j.exer.2011.06.003. Epub 2011 Jun 15. Exp Eye Res. 2011. PMID: 21689648 Free PMC article.
-
HIF-1alpha and HIF-2alpha are differentially activated in distinct cell populations in retinal ischaemia.PLoS One. 2010 Jun 14;5(6):e11103. doi: 10.1371/journal.pone.0011103. PLoS One. 2010. PMID: 20559438 Free PMC article.
-
Mechanisms Leading to Differential Hypoxia-Inducible Factor Signaling in the Diabetic Kidney: Modulation by SGLT2 Inhibitors and Hypoxia Mimetics.Am J Kidney Dis. 2021 Feb;77(2):280-286. doi: 10.1053/j.ajkd.2020.04.016. Epub 2020 Jul 23. Am J Kidney Dis. 2021. PMID: 32711072 Review.
-
Dietary hyperglycemia, glycemic index and metabolic retinal diseases.Prog Retin Eye Res. 2011 Jan;30(1):18-53. doi: 10.1016/j.preteyeres.2010.09.001. Epub 2010 Sep 22. Prog Retin Eye Res. 2011. PMID: 20868767 Free PMC article. Review.
Cited by
-
PACAP Modulates Expression of Hypoxia-Inducible Factors in Streptozotocin-Induced Diabetic Rat Retina.J Mol Neurosci. 2015 Dec;57(4):501-9. doi: 10.1007/s12031-015-0621-7. Epub 2015 Jul 23. J Mol Neurosci. 2015. PMID: 26202258
-
Ischaemia-induced retinal neovascularisation and diabetic retinopathy in mice with conditional knockout of hypoxia-inducible factor-1 in retinal Müller cells.Diabetologia. 2011 Jun;54(6):1554-66. doi: 10.1007/s00125-011-2081-0. Epub 2011 Mar 1. Diabetologia. 2011. PMID: 21360191 Free PMC article.
-
Photoreceptor cells are major contributors to diabetes-induced oxidative stress and local inflammation in the retina.Proc Natl Acad Sci U S A. 2013 Oct 8;110(41):16586-91. doi: 10.1073/pnas.1314575110. Epub 2013 Sep 25. Proc Natl Acad Sci U S A. 2013. PMID: 24067647 Free PMC article.
-
Inhibition of 20-HETE attenuates diabetes-induced decreases in retinal hemodynamics.Exp Eye Res. 2011 Jul;93(1):108-13. doi: 10.1016/j.exer.2011.05.011. Epub 2011 May 30. Exp Eye Res. 2011. PMID: 21658386 Free PMC article.
-
Inner Retinal Oxygen Delivery, Metabolism, and Extraction Fraction in Ins2Akita Diabetic Mice.Invest Ophthalmol Vis Sci. 2016 Nov 1;57(14):5903-5909. doi: 10.1167/iovs.16-20082. Invest Ophthalmol Vis Sci. 2016. PMID: 27802520 Free PMC article.
References
-
- Arjamaa O, Nikinmaa M. Oxygen-dependent diseases in the retina: role of hypoxia-inducible factors. Exp Eye Res. 2006;83:473–483. - PubMed
-
- Ayalasomayajula SP, Kompella UB. Celecoxib, a selective cyclooxygenase-2 inhibitor, inhibits retinal vascular endothelial growth factor expression and vascular leakage in a streptozotocin-induced diabetic rat model. Eur J Pharmacol. 2003;458:283–289. - PubMed
-
- Chen J, Nathans J. Genetic ablation of cone photoreceptors eliminates retinal folds in the retinal degeneration 7 (rd7) mouse. Invest Ophthalmol Vis Sci. 2007;48:2799–2805. - PubMed
-
- Clermont AC, Aiello LP, Mori F, Aiello LM, Bursell SE. Vascular endothelial growth factor and severity of nonproliferative diabetic retinopathy mediate retinal hemodynamics in vivo: a potential role for vascular endothelial growth factor in the progression of nonproliferative diabetic retinopathy. Am J Ophthalmol. 1997;124:433–446. - PubMed
-
- Cringle SJ, Yu DY, Yu PK, Su EN. Intraretinal oxygen consumption in the rat in vivo. Invest Ophthalmol Vis Sci. 2002;43:1922–1927. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

