Hypopyon in patients with uveitis
- PMID: 20006905
- PMCID: PMC2819583
- DOI: 10.1016/j.ophtha.2009.07.025
Hypopyon in patients with uveitis
Abstract
Purpose: To evaluate the risk of and risk factors for hypopyon among patients with uveitis and to evaluate the risk of visual changes and complications after hypopyon.
Design: Retrospective cohort study.
Participants: Patients with uveitis at 4 academic ocular inflammation subspecialty practices.
Methods: Data were ascertained by standardized chart review.
Main outcome measures: Prevalence and incidence of hypopyon, risk factors for hypopyon, and incidence of visual acuity changes and ocular complications after hypopyon.
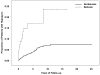
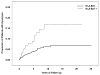
Results: Among 4911 patients with uveitis, 41 (8.3/1000) cases of hypopyon were identified at the time of cohort entry. Of these, 2885 initially free of hypopyon were followed over 9451 person-years, during which 81 patients (2.8%) developed hypopyon (8.57/1000 person-years). Risk factors for incident hypopyon included Behçet's disease (adjusted relative risk [RR]=5.30; 95% confidence interval [CI], 2.76-10.2), spondyloarthropathy (adjusted RR=2.86; 95% CI, 1.48-5.52), and human leukocyte antigen (HLA)-B27 positivity (adjusted RR=2.04; 95% CI, 1.17-3.56). Patients with both a spondyloarthropathy and HLA-B27 had a higher risk than either factor alone (crude RR=4.39; 95% CI, 2.26-8.51). Diagnosis of intermediate uveitis (+/- anterior uveitis) was associated with a lower risk of hypopyon (with respect to anterior uveitis only, adjusted RR=0.35; 95% CI, 0.15-0.85). Hypopyon incidence tended to be lower among patients with sarcoidosis (crude RR=0.22; 95% CI, 0.06-0.90; adjusted RR=-0.28; 95% CI, 0.07-1.15). Post-hypopyon eyes and eyes not developing hypopyon had a similar incidence of band keratopathy, posterior synechiae, ocular hypertension, hypotony, macular edema, epiretinal membrane, cataract surgery, or glaucoma surgery. Post-hypopyon eyes were more likely than eyes not developing hypopyon to gain 3 lines of vision (crude RR=1.54; 95% CI, 1.05-2.24) and were less likely to develop 20/200 or worse visual acuity (crude RR=0.41; 95% CI, 0.17-0.99); otherwise, visual outcomes were similar in these groups.
Conclusions: Hypopyon is an uncommon occurrence in patients with uveitis. Risk factors included Behçet's disease, HLA-B27 positivity, and spondyloarthropathy. Intermediate uveitis cases (+/- anterior uveitis) had a lower risk of hypopyon. On average, post-hypopyon eyes were no more likely than other eyes with uveitis to develop structural ocular complications or lose visual acuity.
Copyright (c) 2010 American Academy of Ophthalmology. Published by Elsevier Inc. All rights reserved.
Figures
References
-
- D’Alessandro LP, Forster DJ, Rao NA. Anterior uveitis and hypopyon. Am J Ophthalmol. 1991;112:317–21. - PubMed
-
- Nussenblatt RB. Uveitis in Behcet’s disease. Int Rev Immunol. 1997;14:67–79. - PubMed
-
- Kempen JH, Daniel E, Gangaputra S, et al. Methods for identifying long-term adverse effects of treatment in patients with eye diseases: the Systemic Immunosuppressive Therapy for Eye Diseases (SITE) Cohort Study. Ophthalmic Epidemiol. 2008;15:47–55. - PubMed
-
- Cox DR, Oakes D. Analysis of Survival Data. London: Chapman and Hall; 1984. pp. 91–107. Monographs on Statistics and Applied Probability.
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Research Materials