Perineal wound complications after abdominoperineal resection
- PMID: 20011400
- PMCID: PMC2780192
- DOI: 10.1055/s-2008-1055325
Perineal wound complications after abdominoperineal resection
Abstract
Perineal wound complications following abdominoperineal resection (APR) is a common occurrence. Risk factors such as operative technique, preoperative radiation therapy, and indication for surgery (i.e., rectal cancer, anal cancer, or inflammatory bowel disease [IBD]) are strong predictors of these complications. Patient risk factors include diabetes, obesity, and smoking. Intraoperative perineal wound management has evolved from open wound packing to primary closure with closed suctioned transabdominal pelvic drains. Wide excision is used to gain local control in cancer patients, and coupled with the increased use of pelvic radiation therapy, we have experienced increased challenges with primary closure of the perineal wound. Tissue transfer techniques such as omental pedicle flaps, and vertical rectus abdominis and gracilis muscle or myocutaneous flaps are being used to reconstruct large perineal defects and decrease the incidence of perineal wound complications. Wound failure is frequently managed by wet to dry dressing changes, but can result in prolonged hospital stay, hospital readmission, home nursing wound care needs, and the expenditure of significant medical costs. Adjuvant therapies to conservative wound care have been suggested, but evidence is still lacking. The use of the vacuum-assisted closure device has shown promise in chronic soft tissue wounds; however, experience is lacking, and is likely due to the difficulty in application techniques.
Keywords: Abdominoperineal resection; perineal wound complication; tissue transfer; vacuum-assisted closure device; wound management.
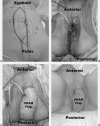
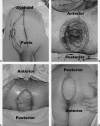
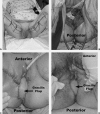
Figures
Similar articles
-
Immediate reconstruction of the perineal wound with gracilis muscle flaps following abdominoperineal resection and intraoperative radiation therapy for recurrent carcinoma of the rectum.Ann Surg Oncol. 1999 Jan-Feb;6(1):33-7. doi: 10.1007/s10434-999-0033-4. Ann Surg Oncol. 1999. PMID: 10030413
-
Vacuum-assisted closure for open perineal wound after abdominoperineal resection.Int J Surg Case Rep. 2015;11:87-90. doi: 10.1016/j.ijscr.2015.04.031. Epub 2015 Apr 29. Int J Surg Case Rep. 2015. PMID: 25942750 Free PMC article.
-
Feasibility of Perineal Defect Reconstruction with Simplified Fasciocutaneous Inferior Gluteal Artery Perforator (IGAP) Flaps after Tumor Resection of the Lower Rectum: Incidence and Outcome in an Interdisciplinary Approach.Cancers (Basel). 2023 Jun 26;15(13):3345. doi: 10.3390/cancers15133345. Cancers (Basel). 2023. PMID: 37444455 Free PMC article.
-
Ten-Year experience with vertical rectus abdominis myocutaneous flap for reconstruction of abdominoperineal resection defects.JPRAS Open. 2020 Nov 30;27:90-98. doi: 10.1016/j.jpra.2020.11.010. eCollection 2021 Mar. JPRAS Open. 2020. PMID: 33376767 Free PMC article. Review.
-
Primary vs myocutaneous flap closure of perineal defects following abdominoperineal resection for colorectal disease: a systematic review and meta-analysis.Colorectal Dis. 2019 Feb;21(2):138-155. doi: 10.1111/codi.14471. Epub 2019 Jan 11. Colorectal Dis. 2019. PMID: 30428157
Cited by
-
Clinical effectiveness of omental transposition in facilitating perineal wound healing after abdominoperineal resection: a systematic review.Yeungnam Univ J Med. 2021 Jul;38(3):219-224. doi: 10.12701/yujm.2020.00871. Epub 2021 Feb 9. Yeungnam Univ J Med. 2021. PMID: 33557001 Free PMC article.
-
Incisional negative pressure wound therapy to reduce perineal wound infection after abdominoperineal resection.Int Wound J. 2021 Feb;18(1):103-111. doi: 10.1111/iwj.13499. Epub 2020 Nov 25. Int Wound J. 2021. PMID: 33236842 Free PMC article.
-
Surgical Outcomes of VRAM vs. Gracilis Flaps in Vulvo-Perineal Reconstruction Following Oncologic Resection: A Proportional Meta-Analysis.Cancers (Basel). 2022 Sep 1;14(17):4300. doi: 10.3390/cancers14174300. Cancers (Basel). 2022. PMID: 36077834 Free PMC article. Review.
-
Case control study investigating the clinical utility of NPWT in the perineal region following abdominoperineal resection for rectal adenocarcinoma: a single center study.BMC Surg. 2022 Jul 30;22(1):296. doi: 10.1186/s12893-022-01746-1. BMC Surg. 2022. PMID: 35907824 Free PMC article. Clinical Trial.
-
Primary closure versus vertical rectus abdominis myocutaneous (VRAM) flap closure of perineal wound following abdominoperineal resection-a systematic review and meta-analysis.Ir J Med Sci. 2024 Aug;193(4):1721-1728. doi: 10.1007/s11845-024-03651-3. Epub 2024 Mar 27. Ir J Med Sci. 2024. PMID: 38532236 Free PMC article.
References
-
- Woods J E, Beart R W., Jr Reconstruction of nonhealing perineal wounds with gracilis muscle flaps. Ann Plast Surg. 1983;11:513–516. - PubMed
-
- Kressner U, Graf W, Mahteme H, Pahlman L, Glimelius B. Septic complications and prognosis after surgery for rectal cancer. Dis Colon Rectum. 2002;45:316–321. - PubMed
-
- Pollard C W, Nivatvongs S, Rojanasakul A, Ilstrup D M. Carcinoma of the rectum: profiles of intraoperative and early postoperative complications. Dis Colon Rectum. 1994;37:866–874. - PubMed
-
- Rothenberger D A, Wong W D. Abdominoperineal resection for adenocarcinoma of the low rectum. World J Surg. 1992;16:478–485. - PubMed
-
- Rosen L, Veiderheimer M, Coller J, Corman M. Mortality, morbidity, and patterns of recurrence after abdominoperineal resection for cancer of the rectum. Dis Colon Rectum. 1982;25:202–208. - PubMed
LinkOut - more resources
Full Text Sources
Miscellaneous

