Biliary atresia
- PMID: 20011467
- PMCID: PMC2788439
- DOI: 10.4103/0971-9261.43015
Biliary atresia
Abstract
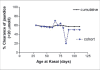
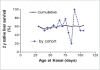
Biliary atresia (BA) is a cholangiodestructive disease affecting biliary tract, which ultimately leads to cirrhosis, liver failure and death if not treated. The incidence is higher in Asian countries than in Europe. Up to 10% of cases have other congenital anomalies, such as polysplenia, asplenia, situs inversus, absence of inferior vena cava and pre-duodenal portal vein, for which we have coined the term Biliary Atresia Splenic Malformation (BASM) syndrome. For these infants the aetiology lies within the first trimester of gestation. For others affected with BA, aetiology is more obscure and perinatal destruction of fully-formed ducts perhaps by the action of hepatotropic viruses has been suggested. Whatever the cause, the lumen of the extrahepatic duct is obliterated at a variable level and this forms the basis for the commonest classification (Types I, II, III). All patients with BA present with varying degree of conjugated jaundice, pale non-pigmented stools and dark urine. Key diagnostic tests include ultrasonography, biochemical liver function tests, viral serology, and (in our centre) a percutaneous liver biopsy. In some centres, duodenal intubation and measurement of intralumenal bile is the norm. Currently BA is being managed in two stages. The first stage involves the Kasai operation, which essentially excises all extrahepatic biliary remnants leaving a transected portal plate, followed by biliary reconstruction using a Roux loop onto that plate as a portoenterostomy. If bile flow is not restored by Kasai procedure or life-threatening complications of cirrhosis ensue then consideration should be given to liver transplantation as a second stage. The outcome following the Kasai operation can be assessed in two ways: clearance of jaundice to normal values and the proportion who survive with their native liver. Clearance of jaundice (<2 mg/dL or <34 micromol/L) after Kasai has been reported to be around 60%, whereas five years survival with native liver ranges from 40% to 65%.
Keywords: Biliary atresia; surgical jaundice.
Conflict of interest statement
Figures
References
-
- Davenport M. Biliary atresia. Semin Pediatr Surg. 2005;14:42–8. - PubMed
-
- Nio M, Ohi R, Miyano T, Saeki M, Shiraki K, Tanaka K, et al. Five and 10 year survival rates after surgery for biliary atresia: A report from the Japanese Biliary Atresia Registry. J Pediatr Surg. 2003;38:997–1000. - PubMed
-
- McKiernan PJ, Baker AJ, Kelly DA. The frequency and outcome of biliary atresia in the UK and Ireland. Lancet. 2000;355:25–9. - PubMed
-
- Balistreri WF, Grand R, Hoofnagle JH, Suchy FJ, Ryckman FC, Perlmutter DH, et al. Biliary atresia: Current concepts and research directions. Hepatology. 1996;23:1682–92. - PubMed
-
- Fischler B, Haglund B, Hjern A. A population based study on the incidence and possible pre- and perinatal etiological risk factors of biliary atresia. J Pediatr. 2002;141:217–22. - PubMed